-
Články
- Vzdělávání
- Časopisy
Top články
Nové číslo
- Témata
- Kongresy
- Videa
- Podcasty
Nové podcasty
Reklama- Práce v oboru
Doporučené pozice
Reklama- Praxe
Activation of Mutant Enzyme Function by Proteasome Inhibitors and Treatments that Induce Hsp70
Missense mutant proteins, such as those produced in individuals with genetic diseases, are often misfolded and subject to processing by intracellular quality control systems. Previously, we have shown using a yeast system that enzymatic function could be restored to I278T cystathionine β-synthase (CBS), a cause of homocystinuria, by treatments that affect the intracellular chaperone environment. Here, we extend these studies and show that it is possible to restore significant levels of enzyme activity to 17 of 18 (94%) disease causing missense mutations in human cystathionine β-synthase (CBS) expressed in Saccharomyces cerevisiae by exposure to ethanol, proteasome inhibitors, or deletion of the Hsp26 small heat shock protein. All three of these treatments induce Hsp70, which is necessary but not sufficient for rescue. In addition to CBS, these same treatments can rescue disease-causing mutations in human p53 and the methylene tetrahydrofolate reductase gene. These findings do not appear restricted to S. cerevisiae, as proteasome inhibitors can restore significant CBS enzymatic activity to CBS alleles expressed in fibroblasts derived from homocystinuric patients and in a mouse model for homocystinuria that expresses human I278T CBS. These findings suggest that proteasome inhibitors and other Hsp70 inducing agents may be useful in the treatment of a variety of genetic diseases caused by missense mutations.
Published in the journal: . PLoS Genet 6(1): e32767. doi:10.1371/journal.pgen.1000807
Category: Research Article
doi: https://doi.org/10.1371/journal.pgen.1000807Summary
Missense mutant proteins, such as those produced in individuals with genetic diseases, are often misfolded and subject to processing by intracellular quality control systems. Previously, we have shown using a yeast system that enzymatic function could be restored to I278T cystathionine β-synthase (CBS), a cause of homocystinuria, by treatments that affect the intracellular chaperone environment. Here, we extend these studies and show that it is possible to restore significant levels of enzyme activity to 17 of 18 (94%) disease causing missense mutations in human cystathionine β-synthase (CBS) expressed in Saccharomyces cerevisiae by exposure to ethanol, proteasome inhibitors, or deletion of the Hsp26 small heat shock protein. All three of these treatments induce Hsp70, which is necessary but not sufficient for rescue. In addition to CBS, these same treatments can rescue disease-causing mutations in human p53 and the methylene tetrahydrofolate reductase gene. These findings do not appear restricted to S. cerevisiae, as proteasome inhibitors can restore significant CBS enzymatic activity to CBS alleles expressed in fibroblasts derived from homocystinuric patients and in a mouse model for homocystinuria that expresses human I278T CBS. These findings suggest that proteasome inhibitors and other Hsp70 inducing agents may be useful in the treatment of a variety of genetic diseases caused by missense mutations.
Introduction
Missense mutations are genetic alterations that result in the production of proteins with single amino acid changes and are an especially common cause of a variety of diseases [1]. Most disease causing missense mutations do not target key catalytic residues, but rather cause problems in protein folding. It is thought that missense mutations affect protein folding by “trapping” the protein in a non-functional intermediate state, preventing it from folding into its lowest-free energy native state. These trapped misfolded protein intermediates can either be degraded or form large molecular weight aggregates [2]. In theory, treatments that could reverse these protein-folding defects and promote proper folding would be of great utility in the treatment of a wide variety of genetic diseases.
Three genetic diseases in which missense mutations are common include cystathionine β-synthase (CBS) deficiency, Li Fraumeni syndrome, and methylenetetrahydrofolate reductase deficiency. CBS deficiency is an inborn error of sulfur metabolism characterized by very high levels of plasma total homocysteine (tHcy). CBS catalyzes the condensation of homocysteine with serine to form cystathionine and is the first step in the de novo production of cysteine. In healthy adults, tHcy concentration in plasma ranges from 5 to 15 µM, but untreated patients with CBS deficiency often have tHcy in excess of 200 µM [3]. CBS deficient patients suffer from various pathologies including arteriosclerosis, osteoporosis, mental retardation, and dislocated lenses [4]. The major cause of mortality in these patients is stroke. Treatments that lower tHcy such as B-vitamins, dietary methionine restriction, and betaine supplementation, can significantly reduce the incidences of vascular events in these patients despite the fact that post-treatment homocysteine levels are still several times higher than levels found in the normal population [5],[6],[7]. Mouse models for CBS deficiency also indicate that there is a threshold effect for tHcy toxicity and support the notion that a small increase in residual CBS activity may have large clinical benefits [8].
Li-Fraumeni syndrome is a dominant cancer susceptibility syndrome disorder caused by missense mutations in the TP53 tumor suppressor gene [9]. Li-Fraumeni patients suffer from a variety of cancers, including sarcomas, adrenocorticol carcinomas, breast cancer, leukemia, and brain tumors [10]. In general, TP53 behaves as a classic tumor suppressor gene, with the tumors losing or inactivating the wild-type copy of TP53, resulting in expression of only the mutant form. Mutant forms of p53 tend to be stable, resulting in increased accumulation of protein [11]. Of the 165 mutations in the TP53 gene described in the Human Gene Mutation Database [12], 110 are of the missense variety (68%).
MTHFR is a critical enzyme in the remethylation of homocysteine to methionine. Its biochemical function is to catalyze the formation of 5-methyltetrahydrofolate, which is the methyl-group donor for the subsequent reaction catalyzed by methionine synthase. Mutations in MTHFR are known to cause MTHFR deficiency. MTHFR deficiency symptoms include developmental delay, motor or gait abnormalities, seizures, and premature vascular disease [13]. Thirty-four mutations have been described in MTHFR deficient patients, and 23 are predicted to encode missense mutations (67%) [12].
Previously, work from our lab has shown that it is possible to restore significant enzymatic function to human CBS containing an isoleucine to threonine substitution at position 278 (I278T) by growth of cells in ethanol containing media [14]. This rescue was shown to require the induction of Hsp70, a key cellular chaperone protein [15]. Hsp70 protein interacts with misfolded polypeptides along with co-chaperones and promotes refolding by repeated cycles of binding and release requiring the hydrolysis of ATP [16]. In the work described here, we have extended our observations by showing that treatments that induce Hsp70 can greatly increase enzymatic function from 17 additional mutant CBS proteins, as well as mutant forms of p53 and MTHFR. In addition we show that proteasome inhibitors can induce Hsp70 and that these drugs can greatly increase mutant CBS activity in human cells and in a mouse model of CBS deficiency. Our findings support the idea that drugs that induce Hsp70 may be useful in the treatment of genetic disorders caused by missense mutations.
Results
Ethanol and deletion of HSP26 restores enzymatic activity to mutant human CBS
We initially examined the effect of ethanol on a panel of 17 additional missense CBS mutations found in homocystinuric patients [17]. Each of these mutations was expressed in a yeast strain (WY35) that is deleted for the endogenous CBS gene (cys4Δ) and growth was examined on cysteine-free media either lacking or containing 4% ethanol (Figure 1A). In addition, we prepared total cellular lysates from the strains grown in cysteine-supplemented media with or without ethanol and measured both the steady state level of each mutant protein by Western blot and CBS enzyme activity (Figure 1B and 1C, 1, Table 1). We found that 4/17 (24%) of the mutants exhibited significant growth and greatly increased CBS enzyme activity (8 to 50-fold) when grown in ethanol-containing media. Interestingly, like I278T, ethanol had a much more modest effect on steady state protein levels compared to enzyme activity, indicating that the treatment caused the specific activity of the enzyme to increase. Ethanol exposure also increased steady state Hsp70 levels, consistent with our previous observations (Figure 1B).
Fig. 1. Functional rescue of mutant CBS by ethanol and hsp26Δ. 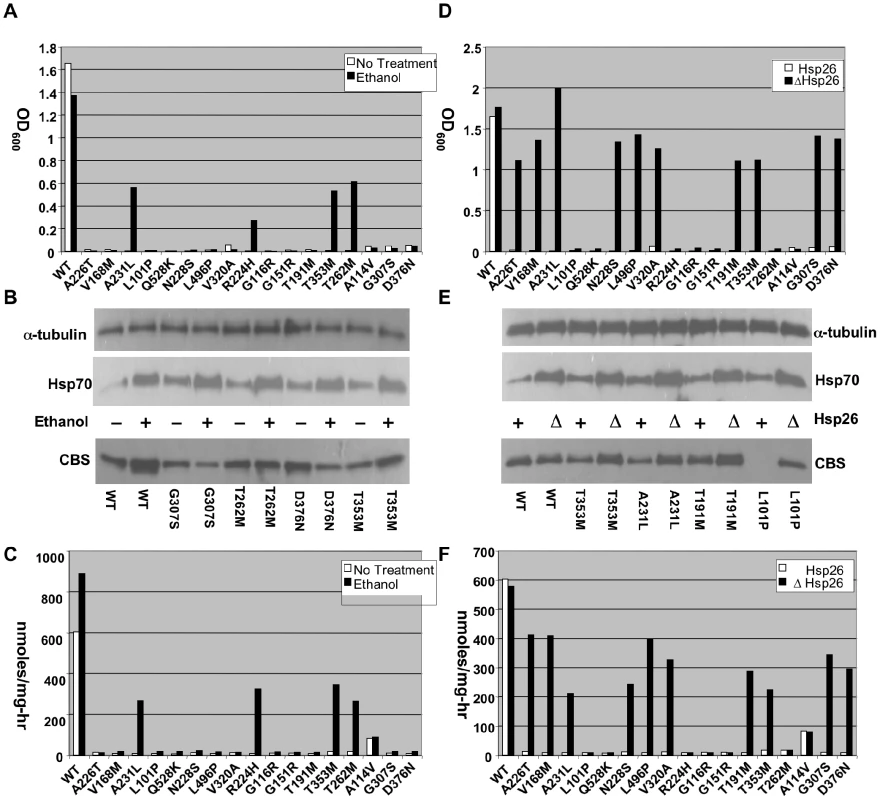
(A) A stationary phase culture of yeast (WY35) transformed with a plasmid expressing the indicated human CBS allele was diluted 1∶1000 in SC–Cys media with or without 4% ethanol and grown at 30°C for 24 h. Growth was determined by measuring OD at 600 nm. (B). Western analysis of two representative ethanol rescuable (T353M, T262M) and two non-rescuable (G307S, D376N) mutants. Cells were grown in SC+CYS media with or without ethanol and extracts were probed with indicated antibody. (C) CBS enzyme activity of each of the mutant alleles in the presence and absence of ethanol. (D) Growth of HSP26 (WY35) or hsp26Δ (LS2) yeast expressing the indicated CBS allele. (E) Western analysis of two representative hsp26Δ rescuable (T353M, A231L) and two non-rescuable (T191M, L101P) mutants. (F) CBS enzyme activity of each of the mutant alleles in the presence and absence of Hsp26. Tab. 1. Relative levels are shown for CBS protein and activity in yeast. 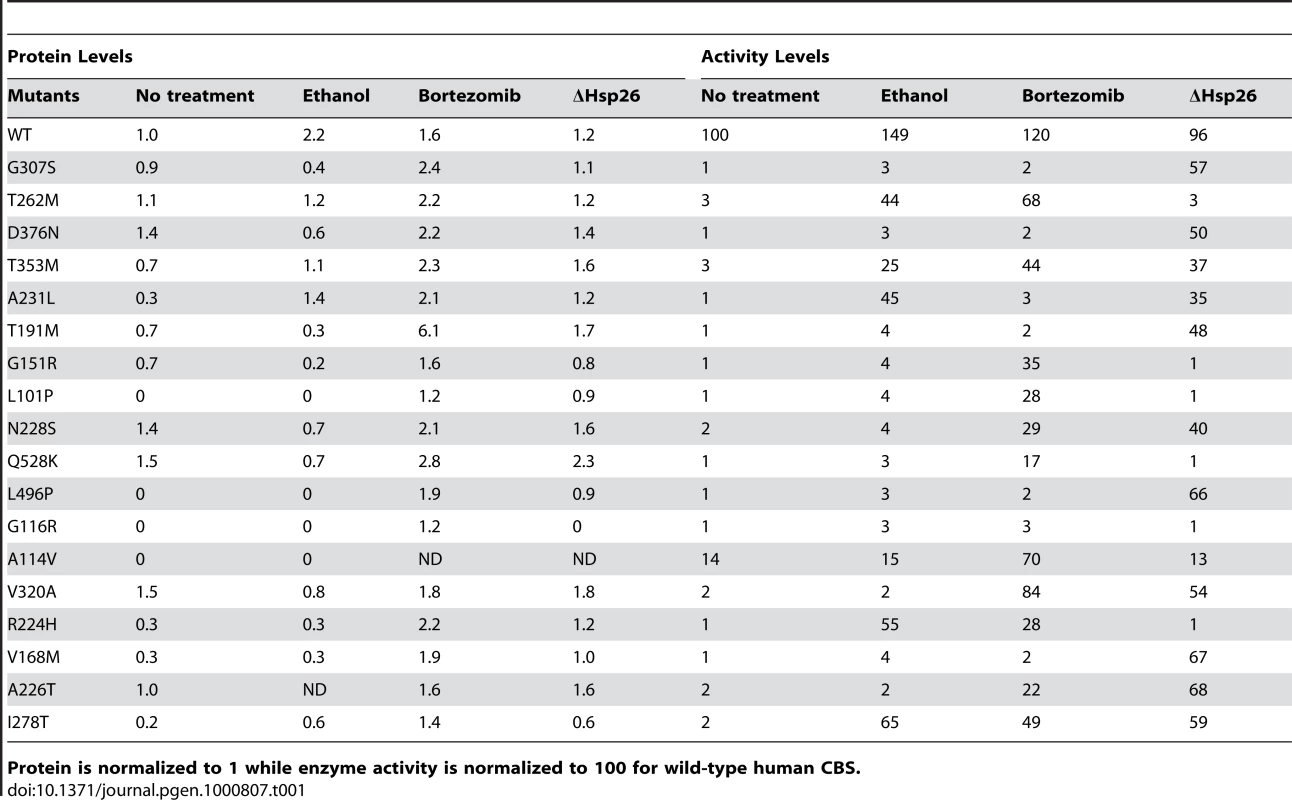
Protein is normalized to 1 while enzyme activity is normalized to 100 for wild-type human CBS. Previously, we had also shown that deletion of the small heat shock protein HSP26 (hsp26Δ) could effectively suppress the functional effects of I278T CBS mutation in yeast [14]. Therefore, we introduced our panel of additional missense mutants into a cys4Δ hsp26Δ double mutant strain and examined function. As with ethanol, hsp26Δ resulted in increased steady state levels of Hsp70 (Figure 1E). Deletion of Hsp26 could rescue the cysteine growth auxotrophy and restore significant levels of enzymatic activity to 10/17 (59%) of the mutants tested (Figure 1D–1F, Figure S2, Table 1). Again, the increased level of enzyme activity in the suppressible mutants was impressive, ranging from an 8 to 55-fold increase resulting in levels that were between 25% and 58% of wild-type CBS. Like ethanol, most of the increased enzyme activity appears to be due to increased functionality of the mutant protein as opposed in increased protein levels.
In our earlier work, we had shown that expression of I278T CBS drove down levels of Hsp26 protein and that I278T CBS, but not wild-type CBS, physically interacted with Hsp26 [14]. We tested two of the newer mutants (G307S, D376N) for these properties and found that they also caused decreased steady state levels of Hsp26 and co-immunoprecipitated Hsp26 (Figure S3). These results indicate that like I278T, G307S and D376N form a complex with Hsp26.
Bortezomib rescues several forms of mutant human CBS expressed in S. cerevisiae
Since proteasome inhibitors have previously been shown to induce Hsp70 in both yeast and mammalian cells [18],[19], we tested if these agents might be able to restore function to missense mutant CBS proteins in vivo. Bortezomib (also known as PS-341 or Velcade) is a potent proteasome inhibitor that is currently used to treat humans with multiple myeloma [20]. We first tested the effects of bortezomib on mutant human I278T CBS function in yeast. We found that addition of bortezomib to yeast media strongly rescued, in a dose-dependent fashion, the cysteine auxotrophy of WY35 cells carrying a plasmid expressing human I278T CBS (pI278T) (Figure 2A). After 24 hours, 75 µM bortezomib allowed WY35pI278T cells to achieve growth that was at least equivalent to WY35 expressing wild type human CBS (phCBS). Examination of I278T protein and activity from treated vs. untreated cells indicated that bortezomib increased steady-state levels of I278T by 7-fold and increased I278T activity by 27-fold, to about 50% of that observed in untreated cells expressing wild-type CBS (Figure 2B). These results show that bortezomib can both stabilize and restore function to I278T CBS expressed in yeast.
Fig. 2. Functional rescue of mutant human CBS expressed in S. cerevisiae by bortezomib treatment. 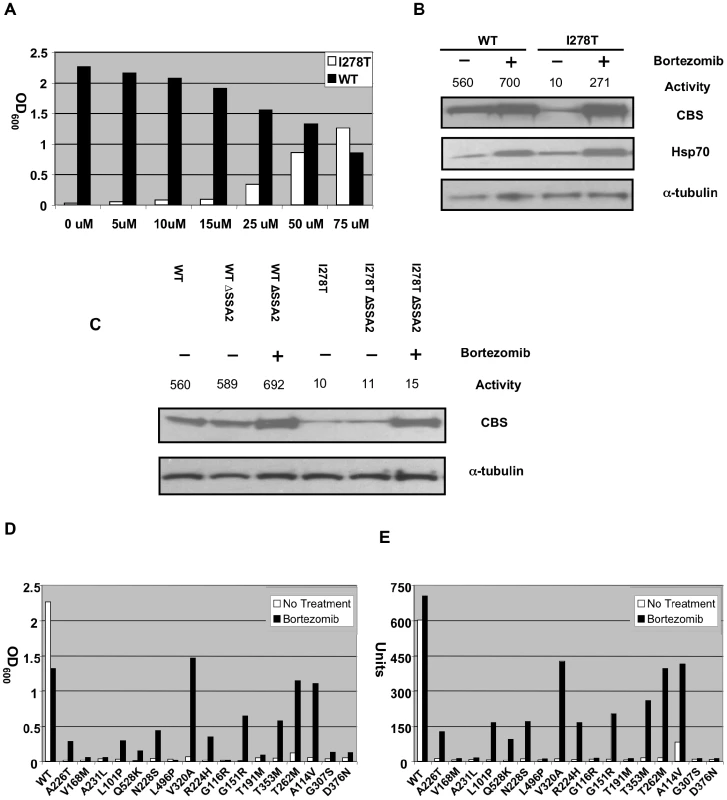
(A) A stationary phase culture of yeast (WY35) transformed with a plasmid expressing either WT (phCBS) or I278T (pI278T) human CBS was diluted 1∶1000 in SC–Cys media with the indicated amount of bortezomib and grown at 30°C for 24 h. Growth was determined by measuring OD at 600 nm. (B) WY35 pI278T and WY35 phCBS cells were grown in SC–Trp+Cys media either with or without 50 µM of bortezomib for 24 hours and extracts were prepared. Levels of CBS, α-tubulin, and Hsp70 and CBS activity were assessed as described in Materials and Methods. CBS units are nmole cystathionine formed/mg protein-hr. (C) Yeast strain WY35 phCBS, WY35 pI278T, LS3 phCBS, LS3 pI278T were grown at 30°C in the absence and presence of bortezomib and extracts were assessed for CBS activity and CBS protein. (D) Stationary phase cultures of yeast strain WY35 expressing the indicated allele of CBS were diluted 1∶1000 in SC–Cys media either with or without 50 µM of bortezomib and growth was monitored by OD600 after 24 h at 30°C. (E) Log phase cultures of WY35 grown in SC+Cys media with or without 50 µM of bortezomib expressing the indicated CBS allele were harvested, lystates prepared, and CBS enzyme activity was measured and expressed in units. Bortezomib treatment also caused a 2.8 to 3.6-fold increase in Hsp70 in WT and I278T expressing strains, respectively (Figure 2B). To determine if this induction was essential for restoration of I278T CBS function, we examined the effect of bortezomib on yeast lacking the Hsp70-encoding gene SSA2 (ssa2Δ; Figure 2C). As expected, steady state levels and the enzyme activity of I278T CBS were lower compared to wt CBS in both SSA2 and ssa2Δ cells in the absence of bortezomib. In the presence of bortezomib, we saw stabilization of I278T protein in ssa2Δ cells, but no increase in enzyme activity. In ssa2Δ cells expressing WT CBS, we did not observe any decrease in enzyme activity, indicating that SSA2 is not required generally for human CBS function. These results show that simply blocking proteolysis of I278T CBS is not sufficient to restore function to the mutant enzyme, and that SSA2 (Hsp70 protein) is required for bortezomib-induced rescue of function.
We also investigated the effect of bortezomib on our panel of other patient-derived CBS mutants. We found that 9/17 of the alleles tested showed significant growth in cysteine-free media and had enzyme activity restored to between 37–68% of wild-type CBS (Figure 2D). It should be noted that some of these mutants (T353M and T262M for example) produce stable but non-functional enzymes, indicating that bortezomib is not simply working by preventing protein degradation (Figure S4)
Restoration of function to mutant forms of p53 and MTHFR
We next determined if chaperone manipulation could be used to restore function to disease causing mutants of p53 and MTHFR. To examine p53 function, we used a yeast strain (yIG397) in which human p53 binds upstream of the ADE2 promoter, activates transcription, and results in correction of the strains adenine auxotrophy [21]. Into this strain we transfected plasmids that expressed either wild-type human p53 or one of three different patient-identified point mutations (R175H, R273H, C277F) and measured p53 function by examining growth in adenine deficient media. As expected, we found that cells expressing wild type human p53 grew well, while cells expressing the mutant alleles had almost undetectable levels of growth (Figure 3A). However, when the media was supplemented with either 4% ethanol, 50 µM Bortezomib, or an hsp26Δ construct was introduced into the strain, each mutant exhibited significant growth rescue with at least one of the treatments.
Fig. 3. Functional rescue of mutant p53 and MTHFR in yeast. 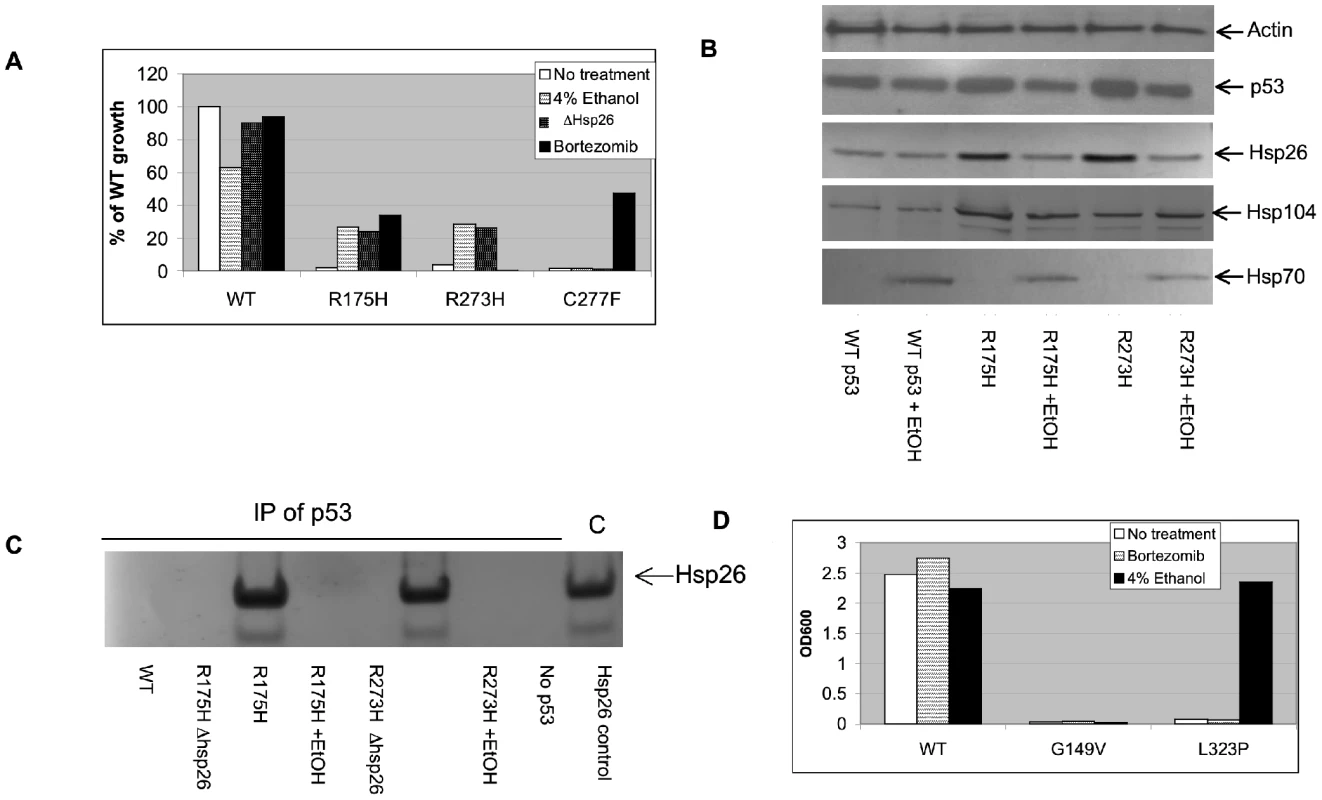
(A) Yeast p53 tester strain yIG397 (HSP26), or LS2 (hsp26Δ) were transformed with an expression plasmid expressing the indicated p53 alleles. Stationary phase cultures of yeast expressing the wild type and indicated mutant were diluted 1∶1000 in SC-ura -ade media grown in 15 ml tubes with aeration at 30°C for 24 hours. Where indicated, 4% ethanol or 50 µM bortezomib were added to the media. (B) Yeast strain yIG397 carrying the indicated p53 alleles was grown in adenine containing media with or without 4% ethanol. Lysates were then probed by Western Blot with the indicated anti-bodies. (C) Yeast strains yIG397 and LS2 expressing the indicated p53 alleles were grown in adenine containing media supplemented with 4% ethanol when indicated. Lysates were prepared and immunoprecipitation was performed with anti-p53 antibody and Hsp26 present in the immune complexes was analyzed by immunoblot. (D) Yeast MTHFR tester strain XSY3-1A (met11Δ) were transformed with expression plasmids expressing the indicated MTHFR allele. We performed more in depth analysis on two of the mutant alleles, R175H and R273H. In the absence of ethanol, steady state levels of both of these mutant proteins are slightly elevated compared to wild type CBS and cause elevations in the steady state levels of Hsp26 and Hsp104 (Figure 3B). The elevation in Hsp104 was unexpected, as we had previously shown that I278T CBS had no effect on Hsp104 levels [14]. When ethanol is added to the cultures, Hsp70 levels are induced and p53 and Hsp26 levels are reduced to wild-type levels, while hsp104 levels remain elevated. The observation that p53 levels go down, while growth increases indicates that, like CBS, ethanol is enhancing the specific activity of p53.
We also examined the dependence of ethanol rescue on having a functionally intact SSA2 and HSP104 (Figure S5). Deletion of either gene resulted in total loss of the ability of ethanol to promote adenine independent growth. Immunoprecipitation experiments demonstrate that, similar to mutant CBS, Hsp26 recognizes mutant p53 but not wild-type p53 and that this interaction is lost upon ethanol treatment. (Figure 3C). Taken together, these results show that p53 mutants behave similar, but not identical, to CBS mutants with regards to rescue by agents that perturb the cellular chaperone environment.
We next determined the frequency by which defective p53 protein could be rescued by either ethanol or bortezomib treatment. We examined rescue using a panel of 22 single missense mutant p53 alleles that were obtained by random mutagenesis of the human p53 (see Materials and Methods). Like CBS, we found that some mutants were rescuable by both ethanol and bortezomib (4/22), some only by bortezomib (8/22), some only by ethanol (4/22), and some that were not rescuable by either treatment (6/22). In total, we found that 16 out of 22 (72%) of the randomly generated mutants were rescuable by at least one of the treatments (Figure S6).
We have also examined the effect of ethanol and bortezomib on mutant alleles of human 5–10-methylene tetrahydrofolate reductase (MTHFR) expressed in yeast. In this assay, expression of a functional human MTHFR enzyme complements the methionine auxotrophy present in a met11Δ mutant [22]. Two missense mutant MTHFR proteins were tested for growth rescue by either addition of ethanol or bortezomib and we found that one, L323P, could be rescued by the addition of ethanol (Figure 3D).
Restoration of CBS function in patient fibroblasts by MG132
We next determined if the restoration of function we observed in S. cerevisiae could also occur in mammalian cells. To test this, we examined the effect of proteasome inhibitors on mammalian cells expressing mutant human CBS protein. We obtained four primary fibroblast lines and one EBV transformed lymphoblastoid line from five patients with CBS deficiency. Four of the five lines were from patients that were homozygous for a particular mutation (I278T, T353M, T262M, G307S), while one line was from a compound heterozygote (A114V/E302K). We then examined both steady state CBS protein and CBS enzyme activity in untreated and in cells treated with the proteasome inhibitor MG132 (Figure 4A). MG132 was used in these experiments because it was found to be a more potent inducer of Hsp70 than bortezomib for these cells (Figure S7). In the absence of drug, three of the five lines (I278T, T253M, and A114V/E302K) had undetectable levels of CBS protein and all five lines had <1% enzyme activity compared to a control primary human fibroblast line. Addition of MG132 resulted in restoration of steady-state CBS to wild-type levels in all five lines and caused a dramatic increase in enzyme activity (over 100-fold increase to 28 to 66% of wt CBS) in three of the five lines (I278T, T353M, and T262M). Interestingly, the increase in enzyme activity in the T262M cells was not associated with increased T262M protein levels, again suggesting that the rescuing effect of proteasome inhibitors is not due to inhibition of mutant protein degradation. Consistent with this idea, we found that MG132 resulted in a two-fold increase in Hsp70 (Figure 4A). With one exception, we note concordance in the behavior of mutants that were rescuable by proteasome inhibition in yeast and in patient fibroblasts. It is possible that the lack of rescue observed in the A114V allele may have to do with the cell line also having the E320K allele as well. In total, these results indicate that exposure of human cells to proteasome inhibitors can rescue enzymatic activity from several missense mutant CBS proteins.
Fig. 4. Functional rescue of mutant CBS by proteosome inhibitors in mammalian cells. 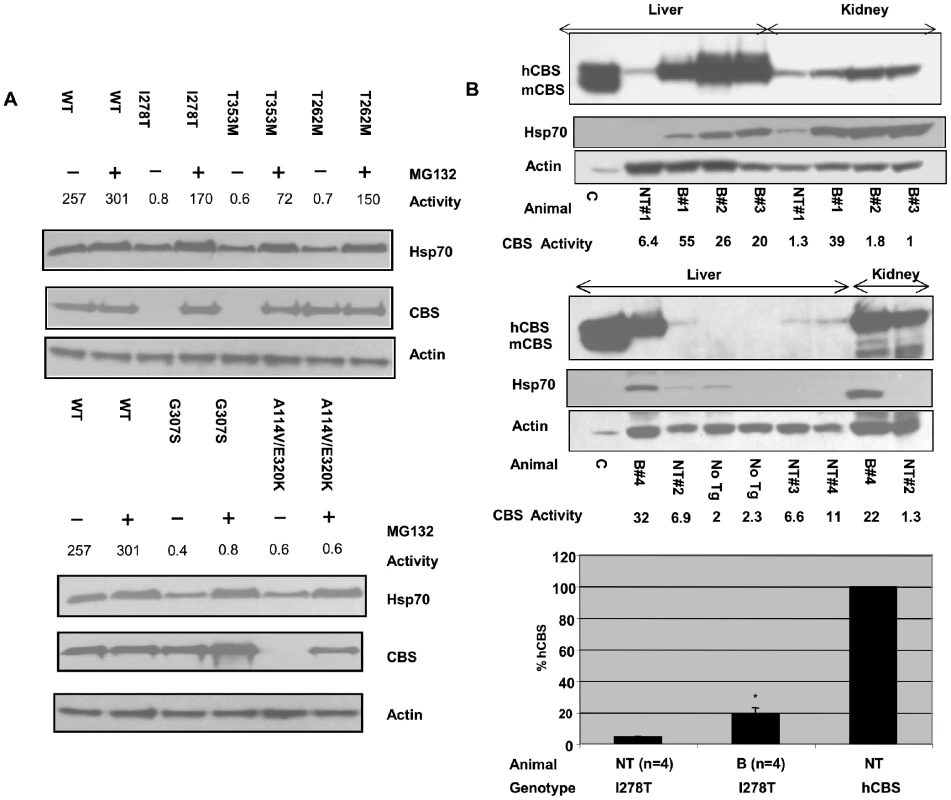
(A) Restoration of CBS enzyme activity in patient fibroblasts. Primary fibroblast cells expressing the indicated CBS allele were grown to 80% confluency at which time MG132 (18 µM) was added. After seven hours protein was harvested and Hsp70, CBS, and actin protein levels were measured by immunoblot. CBS activity was measured and activity is expressed as nmole cystathionine formed/mg protein-hr. Note that the G307S cell line is a transformed lymphoid cell line. (B) Effect of intravenous bortezomib treatment on Tg-I278T Cbs−/− mice. Tg-I278T Cbs−/− mice were kept on zinc water for 10 days to induce transgene expression and then either injected with bortezomib (30 µg) or saline by tail vein injection. After 17 hours mice were sacrificed and tissues harvested. Immunoblot analysis of CBS in liver and kidney extracts from bortezomib treated “B” and non-treated (NT) I278T mice. Actin was used as loading control. CBS activity was measured and activity is expressed as nmole cystathionine formed/mg protein-hr. Mice labeled “No Tg” are Cbs−/− animals lacking human CBS. Lane labeled “C” contains extract from a Tg-I278T Cbs+/− animal. Bar graph shows Liver CBS activity in bortezomib treated (n = 4) and non-treated (n = 4) Tg-I278T Cbs−/−mice was compared with CBS activity in a non-treated mouse containing normal hCBS. Statistical significance was calculated by t test. Results are represented in terms of mean±SE. *P<0.05. Increased CBS activity and lower plasma homocysteine in Tg-I278T Cbs−/− mouse treated with bortezomib
Previously we had developed a mouse model for homocystinuria caused by I278T CBS (Tg-I278T Cbs−/−). This mouse contains a homozygous deletion of the mouse CBS gene, and expresses human I278T CBS under control of a zinc-inducible promoter [23]. In this animal it was demonstrated that human I278T CBS expressed in mouse liver had minimal enzyme activity [24]. To test the effect of bortezomib in vivo, we induced I278T expression by addition of zinc to the drinking water, and after one week injected 30 µg of bortezomib into the tail veins of four Tg-I278T Cbs−/− animals. After 17 hours, serum, liver and kidney were then harvested and analyzed. Examination of steady state CBS protein indicates that bortezomib greatly increased the amount of liver I278T protein and Hsp70 protein compared to a mock-injected control (Figure 4B). In addition, CBS enzyme activity increased on average 4.3-fold in the livers of treated animals compared to untreated controls, to about 18.7% of that found in an animal that expresses wild-type human CBS (Figure 4B). We also observed increased enzyme activity in kidney extracts in two of the four injected animals (Figure 4B). Interestingly, the kidney does not show significantly increased steady-state I278T protein, indicating that the increased enzyme activity is due entirely to increased enzyme specific activity. Bortezomib treatment resulted in a 46% decrease in tHcy in serum, (p<0.05) (Figure S8). Bortezomib also resulted in a 28% decrease in serum methionine, although this was not statistically significant (Figure S8). These results indicate that bortezomib can decrease tHcy in vivo by increasing residual I278T enzyme activity.
Discussion
In the work described here, we have shown that it is possible to restore substantial amount of functional activity to a large percentage of missense mutant alleles of human CBS, p53, and MTHFR expressed in S. cerevisiae by treatments that cause Hsp70 induction. These treatments include addition of ethanol or proteosome inhibitor to the media, or deletion of the small heat shock protein HSP26. At least one of these treatments was able to dramatically increase enzyme or transcriptional activity in 17/18 (94%) mutant CBS proteins, 19/25 mutant p53 proteins (76%), and 1/2 mutant MTHFR proteins (50%). Interestingly, different types of response to the different rescuing treatments were observed. Some mutants were rescued by all three treatments (e.g. I278T CBS), some by two of three treatments (e.g. T262M CBS), while others only responded to a single treatment (e.g. G307S CBS). These differences are probably not due to differential Hsp70 induction, as all three treatments result in similar levels of induction. We speculate that each of these different treatments may have unique effects on other molecular chaperones and that each treatment may produce a unique intracellular folding milieu. With regards to CBS mutants, we found that both pyridoxine responsive mutants (e.g. I278T) and non-responsive mutants (e.g. G307S) could be rescued.
Our findings support the view that most missense mutations primarily affect protein folding, as opposed to altering critical residues involved in specific catalytic or interaction sites. This agrees with biophysical studies of protein folding. As stated by DePristo et al. [25] “The overwhelming conclusion from 20 years of mutation studies on protein stability is that most amino-acid replacements, at all sites in a protein result in large effects on ΔG relative to the observed range of ΔG values themselves.” It is also possible that in multi-domain proteins like CBS, mutations affect protein folding by trapping the protein in a non functional intermediate state due to the existence of a high kinetic barrier [2]. Therefore, a possible explanation for the effectiveness of chaperone manipulation is that chaperone complex either helps mutant proteins overcome rate-limiting kinetic constraints in the folding process or brings the trapped intermediate back to a folding competent state. Interestingly, in CBS, only one mutation, G116R, was not rescuable by any treatment. This mutation is located only three residues away from the lysine (K119) that binds the active site pyridoxal phosphate at the base of an alpha helix [26]. Thus this change may be an example of a mutation that affects a key catalytic-site in the protein.
Our results also show that this is not a yeast-specific phenomenon. We were able to restore function to three of six mutant alleles present in fibroblast cells from CBS deficient patients by treatment with the proteasome inhibitor MG-132. In addition, we showed that a 4.3-fold increase in CBS activity could be achieved with a single injection of bortezomib into mice expressing I278T CBS. Consistent with our findings, Mu et al. showed that MG-132 could increase residual glucocerebrosidase enzyme activity four-fold in cell lines containing the L444P variant associated with Gaucher disease, and that a combination of MG-132 and a chemical chaperone, 2-Acetamido-2-deoxynojirimycin, could increase residual activity five-fold in cells containing the Tay-Sachs disease causing α-hexosaminidase G269S mutation [27]. In addition, the Hsp70-inducing drug arimoclomol was reported to delay disease progression in mice expressing a SOD1 mutant in which glycine is substituted with alanine at position 93 [28].
Taken together, these findings suggest that treatment with proteasome inhibitors and other Hsp70 inducers may be beneficial to individuals with severe genetic diseases caused by missense mutation. One potential concern with drugs that manipulate the molecular chaperone environment is they may have potential adverse effects on the normal proteome, and thus create side effects that would preclude their use as drugs. While this is a possibility, it should be noted that Bortezomib is already an FDA approved drug that is used to treat multiple myeloma. The major noted toxicity is peripheral neuropathy [29]. However, it is unknown if the levels of Bortezomib used to induce changes in the chaperone environment would need to be as high as those used in chemotherapy. Furthermore, there is another proteasome inhibitor in clinical trials (PR-171) that does not exhibit a strong peripheral neuropathy effect [30]. In addition, there are at least two other drugs that are known Hsp70 inducers that have undergone successful phase I trials in humans including 17-allylamino-17-demethoxygeldanamycin and arimoclomol [31],[32]. Therefore, while there may be some risk in this approach, there is no reason a priori to believe that the benefits of restoring function to a mutant protein would not out weigh the potential side effects.
In addition to germline genetic diseases, the work described here may have relevance to the treatment of somatic genetic diseases such as cancer. Mutations in p53 are the most frequent genetic alteration in human cancer, and loss of p53 function is critical for tumorigenesis [33]. Several pharmacologic chaperones that restore function to mutant p53 protein have been identified and these have been shown to effectively induce apoptosis in certain cells that express mutant p53 [34],[35]. Our findings suggest that proteasome inhibitors may also effectively restore function to certain p53 alleles. Although bortezomib has been shown to inhibit cell growth and cause apoptosis in a large number of cancer cell lines, the IC50 concentrations vary widely [36]. No systematic study of the relationship between bortezomib sensitivity and the p53 status of tumor cells has been reported.
In summary, the data reported here shows that the functional effects of a majority of missense mutations in at least three human genes can be reversed by treatments that alter the intracellular molecular chaperone environment. Based on these results, we suggest that drugs that effect the intracellular chaperone environment may be useful in the treatment of a number of genetic diseases caused by missense mutations.
Materials and Methods
Yeast strains, plasmids, growth, and drug treatment
Yeast strains WY35 (α leu2 ura3 ade2 trp1 cys4::LEU2), LS1 (α leu2 ura3 ade2 trp1 cys4::LEU2 hsp26::KanMX) and LS3 (α leu2 ura3 ade2 trp1 cys4::LEU2 ssa2::KanMX) were generated as previously described [14],[37]. Yeast strain yIG397 (MATa ade2-1 leu2-3,112 trp1-1 his-11,15 can1-100, ura3-1 URA3 3XRGC::pCYC1::ADE2) was obtained from Dr. Richard Iggo [21]. Strains LS3 (yIG397+hsp26Δ), LS4 (yIG397+ssa2Δ) and LS5 (yIG397+hsp104Δ) were derived from this strain by transformation with appropriate deletion cassettes as previously described [14]. The MTHFR tester strain, XSY3-1a (MATa ade2-1, can1-100, ura3 leu2 trp1, his3, trp1 met11Δ::TRP1) was created as previously described [22]. Plasmids expressing wild-type or mutant human CBS proteins were created by site-directed mutagenesis and gap-repair as described [38],[39]. The plasmids expressing mutant p53 alleles were constructed using gap repair with pRDI-22 [21]. Additional p53 mutants were generated by amplification with TaqI polymerase, followed by gap-repair and subsequent screening on SC-ade media for non-functional alleles. Ninety-six clones were then isolated and sequenced. Twenty-three of these clones contained a single missense mutation and were used for the studies described here. Bortezomib (Velcade™, Millennium Pharmaceuticals, Inc) was obtained from the Fox Chase Cancer Center outpatient clinic. Synthetic complete media lacking cysteine (SC–Cys) and (SC–Cys+G418) were made as previously described [14]. SC+Cys media were made by adding glutathione to the indicated SC media at a final concentration of 30 µg/ml. All other chemicals were purchased from Sigma. For yeast cell growth assays, saturated cultures were diluted to an OD600 of 0.05 and treated with bortezomib in standard 15-ml borosilicate tubes containing 3 ml of media. Cells were then grown at 30°C with rotating aeration. After 24 hours OD600 was determined using a Milton Roy Spectronic 601 spectrophotometer (Ivyland, PA).
Cell lines and drug treatment
Cell lines used in this study were: WS1 (WT) [40], F5889 (I278T/I278T) [41], 382 (T262M/T262M ) [42], 2242 (A114V/E302K) [43], 3161 (T353M/T353M, JPK unpublished), 3079 (G307S/G307S) [44]. Fibroblasts and EBV transformed lymphoid cells were grown in MEM or RPMI medium supplemented with 15% FBS along with appropriate antibiotics, respectively, in 5% CO2 at 37°C. MG132 was purchased from Peptide International (product number, IZL-3175v). MG132 or bortezomib was added to cells when they reached 80% confluency and after seven hours of exposure, the MG132 containing media was discarded, cells were rinsed with PBS, and then harvested for protein extraction.
Extract preparation and immunoblot analysis
Saturated yeast were diluted to an OD600 of 0.05 and cells were harvested when OD was between 0.7 and 0.9 (mid-log phase). Yeast extracts were prepared by mechanical lysis as described previously [45]. Total mammalian protein extracts were prepared using the mammalian protein extraction reagent obtained from Pierce, Rockford, IL (product # 78501). Protein concentration was determined by the Coomassie Blue protein assay reagent (Pierce) using bovine serum albumin as a standard. For immunoblot analysis, yeast extracts containing 20 µg or mammalian cell containing 50 µg of total protein were run on precast Tris-acetate gels (Bio-Rad) at 15 mA and transferred to polyvinylidene difluoride membrane as previously described [14]. Immunopurified mouse anti-CBS was purchased from ABNOVA (catalogue # H00000875-A01) and was used at 1/10,000 dilution. Anti-p53 is a mouse monoclonal anti-body obtained by Calbiochem (cat. #OP43) and was used at a 1/1000 dilution. Yeast Hsp70 monoclonal mouse serum was from AbCAM (catalogue # ab5439) and used at a dilution of 1/5000. Human Hsp70 monoclonal antibody (product # SPA-810D) was used at 1/1000 dilution. Α-Tubulin antibody used here is the same as described previously [14]. For rabbit antiserum, a horseradish peroxidase-conjugated anti-rabbit secondary anti-body was used at a 1/30,000 dilution (Jackson ImmunoResearch, West Grove, PA). Signal was detected by chemiluminescence using SuperSignal West Pico chemiluminescent substrate (Amersham Biosciences) and Chemigenius station (Syngene); signal was quantitated by Alpha Innotech software. Immunopreciptiations were performed as previously described [14].
Mouse studies
All animal studies were reviewed and approved by the Fox Chase Cancer Center Institutional Animal Care and Use Committee. Tg-hCBS Cbs−/− and Tg-I278T Cbs−/− mice were generated as previously described [23],[46]. All mice were from C57BL6 strain background and were fed the rodent chow (Teklad 2018SX; Harlan Teklad, Madison, WI, USA) ad libitum. Adult mice (9–12 months old) were injected with 30 µl of bortezomib (1 mg/ml) via tail vein injection. After 17 hour, mice were sacrificed and liver, kidney and serum were extracted. Liver and kidney homogenates were prepared as previously described [46]. Western blotting was done under denaturing conditions as previously described [47].
CBS activity and metabolite measurement
CBS activity was measured in 30 mg of crude dialyzed protein extracts of liver and kidney, using a Biochrom 30 amino acid analyzer (Biochrom, Cambridge, UK) as described previously [47]. One unit of activity is one µM of cystathionine formed per hour per milligram of protein. The same instrument was employed to measure total homocysteine (tHcy) and methionine in serum as described [8].
Supporting Information
Zdroje
1. StensonPD
BallEV
MortM
PhillipsAD
ShielJA
2003 Human Gene Mutation Database (HGMD): 2003 update. Hum Mutat 21 577 581
2. BrossP
CorydonTJ
AndresenBS
JorgensenMM
BolundL
1999 Protein misfolding and degradation in genetic diseases. Hum Mutat 14 186 198
3. KrugerWD
WangL
JheeKH
SinghRH
ElsasLJ,2nd
2003 Cystathionine beta-synthase deficiency in Georgia (USA): correlation of clinical and biochemical phenotype with genotype. Hum Mutat 22 434 441
4. MuddSH
SkovbyF
LevyHL
PettigrewKD
WilckenB
1985 The natural history of homocystinuria due to cystathionine beta-synthase deficiency. Am J Hum Genet 37 1 31
5. WilckenDE
WilckenB
1997 The natural history of vascular disease in homocystinuria and the effects of treatment. Journal of Inherited Metabolic Disease 20 295 300
6. YapS
NaughtenER
WilckenB
WilckenDE
BoersGH
2000 Vascular complications of severe hyperhomocysteinemia in patients with homocystinuria due to cystathionine beta-synthase deficiency: effects of homocysteine-lowering therapy. Semin Thromb Hemost 26 335 340
7. YapS
BoersGH
WilckenB
WilckenDE
BrentonDP
2001 Vascular outcome in patients with homocystinuria due to cystathionine beta-synthase deficiency treated chronically: a multicenter observational study. Arterioscler Thromb Vasc Biol 21 2080 2085
8. GuptaS
KühnischJ
MustafaA
LhotakS
SchlachtermanA
2009 Mouse models of cystathionine β-synthase deficiency reveal significant threshold effects of hyperhomocysteinemia. FASEB J 23 883 893
9. VarleyJM
2003 Germline TP53 mutations and Li-Fraumeni syndrome. Hum Mutat 21 313 320
10. GonzalezKD
NoltnerKA
BuzinCH
GuD
Wen-FongCY
2009 Beyond Li Fraumeni Syndrome: Clinical Characteristics of Families With p53 Germline Mutations. J Clin Oncol 27 1250 1256
11. EsrigD
SpruckCH3rd
NicholsPW
ChaiwunB
StevenK
1993 p53 nuclear protein accumulation correlates with mutations in the p53 gene, tumor grade, and stage in bladder cancer. Amer J Path 143 1389 1397
12. Cooper EVBDN
StensonPD
PhillipsAD
HowellsK
MortME
2009 The human gene mutation database at the institute of medical genetics at Cardiff.
13. GoyetteP
FrosstP
RosenblattDS
RozenR
1995 Seven novel mutations in the methylenetetrahydrofolate reductase gene and genotype/phenotype correlations in severe methylenetetrahydrofolate reductase deficiency. Amer J Hum Genet 56 1052 1059
14. SinghLR
KrugerWD
2009 Functional rescue of mutant human cystathionine β-synthase by manipulation of Hsp26 and Hsp70 levels in Saccharomyces cerevisiae. J Biol Chem 284 4238 4245
15. YoungJC
AgasheVR
SiegersK
HartlFU
2004 Pathways of chaperone-mediated protein folding in the cytosol. Nat Rev Mol Cell Biol 5 781 791
16. HartlFU
Hayer-HartlM
2002 Molecular chaperones in the cytosol: from nascent chain to folded protein. Science 295 1852 1858
17. KrausJP
JanosikM
KozichV
MandellR
ShihV
1999 Cystathionine beta-synthase mutations in homocystinuria. Hum Mutat 13 362 375
18. LeeDH
GoldbergAL
1998 Proteasome inhibitors cause induction of heat shock proteins and trehalose, which together confer thermotolerance in Saccharomyces cerevisiae. Mol Cell Biol 18 30 38
19. KimD
LiGC
1999 Proteasome inhibitors lactacystin and MG132 inhibit the dephosphorylation of HSF1 after heat shock and suppress thermal induction of heat shock gene expression. Biochem Biophys Res Com 264 352 358
20. OrlowskiRZ
KuhnDJ
2008 Proteasome inhibitors in cancer therapy: lessons from the first decade. Clin Cancer Res 14 1649 1657
21. FlamanJM
FrebourgT
MoreauV
CharbonnierF
MartinC
1995 A simple p53 functional assay for screening cell lines, blood, and tumors. Proc Natl Acad Sci U S A 92 3963 3967
22. ShanX
WangL
HoffmasterR
KrugerWD
1999 Functional characterization of human methylenetetrahydrofolate reductase in Saccharomyces cerevisiae. J Biol Chem 274 32613 32618
23. WangL
ChenX
TangB
HuaX
Klein-SzantoA
2005 Expression of mutant human cystathionine beta-synthase rescues neonatal lethality but not homocystinuria in a mouse model. Hum Mol Genet 14 2201 2208
24. ChenX
WangL
FazlievaR
KrugerWD
2006 Contrasting behaviors of mutant cystathionine beta-synthase enzymes associated with pyridoxine response. Hum Mutat 27 474 482
25. DePristoMA
WeinreichDM
HartlDL
2005 Missense meanderings in sequence space: a biophysical view of protein evolution. Nat Rev Genet 6 678 687
26. MeierM
JanosikM
KeryV
KrausJP
BurkhardP
2001 Structure of human cystathionine beta-synthase: a unique pyridoxal 5′-phosphate-dependent heme protein. Embo J 20 3910 3916
27. MuTW
FowlerDM
KellyJW
2008 Partial restoration of mutant enzyme homeostasis in three distinct lysosomal storage disease cell lines by altering calcium homeostasis. PLoS Biol 6 e26 doi:10.1371/journal.pbio.0060026
28. KieranD
KalmarB
DickJR
Riddoch-ContrerasJ
BurnstockG
2004 Treatment with arimoclomol, a coinducer of heat shock proteins, delays disease progression in ALS mice. Nature Med 10 402 405
29. GilardiniA
MarmiroliP
CavalettiG
2008 Proteasome inhibition: a promising strategy for treating cancer, but what about neurotoxicity? Curr Med Chem 15 3025 3035
30. JagannathS
VijR
StewartK
SomloA
JackubowiakA
2009 Final resutls of PX-171-003-A0, part 1 of an open-label, single-arm, phase II study of carfilzomib (CFZ) in patients with relapsed and refractory multiple myeloma. 2009 ASCO Annual Meeting Orlando Fl J. Clin Oncol 15S (abstr 8504)
31. SolitDB
IvySP
KopilC
SikorskiR
MorrisMJ
2007 Phase I trial of 17-allylamino-17-demethoxygeldanamycin in patients with advanced cancer. Clin Cancer Res 13 1775 1782
32. CudkowiczME
ShefnerJM
SimpsonE
GrassoD
YuH
2008 Arimoclomol at dosages up to 300 mg/day is well tolerated and safe in amyotrophic lateral sclerosis. Muscle and Nerve 38 837 844
33. SoussiT
WimanKG
2007 Shaping genetic alterations in human cancer: the p53 mutation paradigm. Cancer Cell 12 303 312
34. BykovVJ
IssaevaN
ShilovA
HultcrantzM
PugachevaE
2002 Restoration of the tumor suppressor function to mutant p53 by a low-molecular-weight compound. Nat Med 8 282 288
35. BykovVJ
SelivanovaG
WimanKG
2003 Small molecules that reactivate mutant p53. European Journal of Cancer 39 1828 1834
36. AdamsJ
PalombellaVJ
SausvilleEA
JohnsonJ
DestreeA
1999 Proteasome inhibitors: a novel class of potent and effective antitumor agents. Cancer Research 59 2615 2622
37. KrugerWD
1994 A yeast system for expression of human cystathionine beta-synthase: structual and functional conservation of the human and yeast genes. Proc Natl Acad Sci USA 91 6614 6618
38. KrugerWD
CoxDR
1995 A yeast assay for functional detection of mutations in the human cystathionine beta-synthase gene. Hum Mol Genet 4 1155 1161
39. ShanX
KrugerWD
1998 Correction of disease-causing CBS mutations in yeast. Nat Genet 19 91 93
40. TangB
LiYN
KrugerWD
2000 Defects in methylthioadenosine phosphorylase are associated with but not responsible for methionine-dependent tumor cell growth. Cancer Res 60 5543 5547
41. TangB
KadariyaY
MurphyME
KrugerWD
2006 The methionine salvage pathway compound 4-methylthio-2-oxobutanate causes apoptosis independent of down-regulation of ornithine decarboxylase. Biochem Pharmacol 72 806 815
42. MoatSJ
BaoL
FowlerB
BonhamJR
WalterJH
2004 The molecular basis of cystathionine beta-synthase (CBS) deficiency in UK and US patients with homocystinuria. Hum Mutat 23 206
43. de FranchisR
KrausE
KozichV
SebastioG
KrausJP
1999 Four novel mutations in the cystathionine beta-synthase gene: effect of a second linked mutation on the severity of the homocystinuric phenotype. Hum Mutat 13 453 457
44. HuFL
GuZ
KozichV
KrausJP
RameshV
1993 Molecular basis of cystathionine beta-synthase deficiency in pyridoxine responsive and nonresponsive homocystinuria. Hum Mol Genet 2 1857 1860
45. ShanX
DunbrackRLJr
ChristopherSA
KrugerWD
2001 Mutations in the regulatory domain of cystathionine beta synthase can functionally suppress patient-derived mutations in cis. Hum Mol Genet 10 635 643
46. WangL
JheeKH
HuaX
DiBelloPM
JacobsenDW
2004 Modulation of cystathionine beta-synthase level regulates total serum homocysteine in mice. Circ Res 94 1318 1324
47. GuptaS
WangL
HuaX
KrijtJ
KozichV
2008 Cystathionine β-synthase p.S466L mutation causes hyperhomocysteinemia in mice. Hum Mutat 29 1048 1054
Štítky
Genetika Reprodukční medicína
Článek Maternal Ethanol Consumption Alters the Epigenotype and the Phenotype of Offspring in a Mouse ModelČlánek Genetic Dissection of Differential Signaling Threshold Requirements for the Wnt/β-Catenin PathwayČlánek Distinct Type of Transmission Barrier Revealed by Study of Multiple Prion Determinants of Rnq1
Článek vyšel v časopisePLOS Genetics
Nejčtenější tento týden
2010 Číslo 1- Je „freeze-all“ pro všechny? Odborníci na fertilitu diskutovali na virtuálním summitu
- Kazuistika – Perspektivy využití precizované medicíny v rámci personalizované specifické terapie onkologických pacientů
- Nobelova cena za chemii pro genetické nůžky: Objev, který změní naši budoucnost?
- Technologie na bázi RNA v klinické praxi: od přebarvených petúnií k terapii vzácných a dosud jen obtížně léčitelných chorob u lidí
- „Nepředstavovali jsme si, že náš výzkum povede přímo ke vzniku nových léků, dokonce ještě za našeho života“
-
Všechny články tohoto čísla
- Irradiation-Induced Genome Fragmentation Triggers Transposition of a Single Resident Insertion Sequence
- A Major Role of the RecFOR Pathway in DNA Double-Strand-Break Repair through ESDSA in
- Kidney Development in the Absence of and Requires
- Modeling of Environmental Effects in Genome-Wide Association Studies Identifies and as Novel Loci Influencing Serum Cholesterol Levels
- Inverse Correlation between Promoter Strength and Excision Activity in Class 1 Integrons
- Activation of Mutant Enzyme Function by Proteasome Inhibitors and Treatments that Induce Hsp70
- Postnatal Survival of Mice with Maternal Duplication of Distal Chromosome 7 Induced by a / Imprinting Control Region Lacking Insulator Function
- The Werner Syndrome Protein Functions Upstream of ATR and ATM in Response to DNA Replication Inhibition and Double-Strand DNA Breaks
- Maternal Ethanol Consumption Alters the Epigenotype and the Phenotype of Offspring in a Mouse Model
- Understanding Gene Sequence Variation in the Context of Transcription Regulation in Yeast
- miR-30 Regulates Mitochondrial Fission through Targeting p53 and the Dynamin-Related Protein-1 Pathway
- Elevated Levels of the Polo Kinase Cdc5 Override the Mec1/ATR Checkpoint in Budding Yeast by Acting at Different Steps of the Signaling Pathway
- Alternative Epigenetic Chromatin States of Polycomb Target Genes
- Co-Orientation of Replication and Transcription Preserves Genome Integrity
- A Comprehensive Map of Insulator Elements for the Genome
- Environmental and Genetic Determinants of Colony Morphology in Yeast
- U87MG Decoded: The Genomic Sequence of a Cytogenetically Aberrant Human Cancer Cell Line
- The MCM-Binding Protein ETG1 Aids Sister Chromatid Cohesion Required for Postreplicative Homologous Recombination Repair
- Genetic Dissection of Differential Signaling Threshold Requirements for the Wnt/β-Catenin Pathway
- Differential Localization and Independent Acquisition of the H3K9me2 and H3K9me3 Chromatin Modifications in the Adult Germ Line
- Genetic Crossovers Are Predicted Accurately by the Computed Human Recombination Map
- Collaborative Action of Brca1 and CtIP in Elimination of Covalent Modifications from Double-Strand Breaks to Facilitate Subsequent Break Repair
- Distinct Type of Transmission Barrier Revealed by Study of Multiple Prion Determinants of Rnq1
- Genome-Wide Association Study Identifies as a Novel Susceptibility Gene for Osteoporosis
- and Regulate Reproductive Habit in Rice
- Nonsense-Mediated Decay Enables Intron Gain in
- Altered Gene Expression and DNA Damage in Peripheral Blood Cells from Friedreich's Ataxia Patients: Cellular Model of Pathology
- The Systemic Imprint of Growth and Its Uses in Ecological (Meta)Genomics
- The Gift of Observation: An Interview with Mary Lyon
- Genotype and Gene Expression Associations with Immune Function in
- The Elongator Complex Regulates Neuronal α-tubulin Acetylation
- Rising from the Ashes: DNA Repair in
- Mis-Spliced Transcripts of Nicotinic Acetylcholine Receptor α6 Are Associated with Field Evolved Spinosad Resistance in (L.)
- BRIT1/MCPH1 Is Essential for Mitotic and Meiotic Recombination DNA Repair and Maintaining Genomic Stability in Mice
- Non-Coding Changes Cause Sex-Specific Wing Size Differences between Closely Related Species of
- Evidence for Pervasive Adaptive Protein Evolution in Wild Mice
- Evolutionary Mirages: Selection on Binding Site Composition Creates the Illusion of Conserved Grammars in Enhancers
- VEZF1 Elements Mediate Protection from DNA Methylation
- PLOS Genetics
- Archiv čísel
- Aktuální číslo
- Informace o časopisu
Nejčtenější v tomto čísle- A Major Role of the RecFOR Pathway in DNA Double-Strand-Break Repair through ESDSA in
- Kidney Development in the Absence of and Requires
- The Werner Syndrome Protein Functions Upstream of ATR and ATM in Response to DNA Replication Inhibition and Double-Strand DNA Breaks
- Alternative Epigenetic Chromatin States of Polycomb Target Genes
Kurzy
Zvyšte si kvalifikaci online z pohodlí domova
Revma Focus: Spondyloartritidy
nový kurz
Autoři: prof. MUDr. Vladimír Palička, CSc., Dr.h.c., doc. MUDr. Václav Vyskočil, Ph.D., MUDr. Petr Kasalický, CSc., MUDr. Jan Rosa, Ing. Pavel Havlík, Ing. Jan Adam, Hana Hejnová, DiS., Jana Křenková
Autoři: MDDr. Eleonóra Ivančová, PhD., MHA
Autoři: prof. MUDr. Eva Kubala Havrdová, DrSc.
Všechny kurzyPřihlášení#ADS_BOTTOM_SCRIPTS#Zapomenuté hesloZadejte e-mailovou adresu, se kterou jste vytvářel(a) účet, budou Vám na ni zaslány informace k nastavení nového hesla.
- Vzdělávání



