-
Medical journals
- Career
Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
Authors: S. Uderzo; E. Esposito; F. Vampa; M. Sapienza; M. Faenza; E. Grella; G. Nicoletti
Authors‘ workplace: Plastic Surgery Department, Primo Policlinico, Università degli Studi della Campania “Luigi Vanvitelli”, Napoli, Italy
Published in: ACTA CHIRURGIAE PLASTICAE, 67, 4, 2025, pp. 235-244
doi: https://doi.org/10.48095/ccachp2025235Introduction
Rectus diastasis (RD) is a clinical condition with a high prevalence worldwide. The definition currently accepted by most authors describes RD as a widening of the linea alba beyond 2 cm, accompanied by thinning of this structure [1–3].
This condition results in a protruding abdomen, which leads to both aesthetic concerns and significant functional disability for the patient, affecting the entire abdominal wall. This disability primarily predisposes patients to the development of hernias, lower back pain, and reduced trunk muscle strength [4–6].
The two main patient groups affected are post-bariatric patients and postpartum women.
The diagnosis of diastasis recti is mostly clinically made using the “finger width” method, which manually assesses the distance between the medial margins of the two rectus muscles. Alternatively, more in-depth diagnostic methods such as ultrasound or CT can be used [1].
In the early stages, treatment of the condition takes place through non-surgical approaches such as physiotherapy or training programs aimed at strengthening the abdominal wall; in the more advanced stages, invasive open or laparoscopic surgical methods are used.
Most existing studies consider a wall defect > 5 cm as the appropriate indication for a surgical approach [6]. However, currently, there is no unanimity on a tailor-made approach for each type of patient suffering from the diastasis of rectal muscles.
The aim of this study is to perform an updated review of the last 20 years in the treatment of the diastasis of rectal muscles in conjunction with an abdominoplasty, to evaluate any existing differences in the surgical treatment of postpartum and post-bariatric diastasis recti and, finally, to evaluate any existing differences in the management of female and male patients.
Evaluation of the topic
Methods
The research was conducted on PubMed, Google Scholar and Cochrane library according to the 2009 Prisma statement, using the following words:
((((“Rectus Abdominis/surgery”[Mesh]) OR (Rectus muscle)) OR (Abdominal muscle)) OR (Abdominal wall*)) AND (((“Diastasis, Muscle/surgery”[Mesh]) OR (Abdominal diastasis)) OR (abdominal separation)).
The bibliographies of all articles were consulted to search for any other eligible articles not included in the algorithm’s search results. The articles were selected by two independent physicians according to the following inclusion criteria: comprehensive English-language articles published from 2004 to 2024 regarding surgical techniques for the treatment of diastasis recti, conducted on patients over 18 years of age. In the event of disagreement on the selection of an article according to the eligibility criteria, two other reviewers were consulted.
Non-English articles, animal studies and letters to editors were excluded. In addition, articles dealing with conservative techniques for the treatment and prevention of diastasis recti, articles dealing with hernia repair techniques that do not have a midline defect and articles dealing with “complex” reconstruction of the abdominal wall were excluded. Finally, articles that talk about the repair of the defect through laparoscopic surgical techniques have been excluded. The data extracted from the articles concern the title, year and name of the author, number of patients included, and number of articles included, type of diastasis (post-pregnancy or post-bariatric), technique used, materials used, recurrence rate and complications.
Efforts were made to minimize potential biases. Data analysis for each individual article was conducted through a comprehensive review of the text and extraction of relevant information from the presented tables. When the patient category, falling within one of the two study-specific groups, was not explicitly stated, this was documented accordingly in the study tables. Additionally, the results of the selected articles were reported both in the tables and summarized in a few lines within the text.
2,352 articles emerged from the research. After skimming according to the PRISMA statement and after eliminating duplicates, 37 articles were selected (Scheme 1). Five articles have been selected from the bibliography of the research articles as they are considered related to the purpose of the review.
Of the selected articles, 15 are reviews. Tab. 1 shows the data extrapolated from the reviews as type of surgical technique and suture / suture material / suture size used in the correction of diastasis recti: nine reviews analyze studies with open technique, seven reviews analyze characteristics of suture material and type of plication (single layer or multilayer), three reviews analyze the differences between men and women, and one is an analysis conducted on cadavers.
Tab. 2 shows, on the other hand, the data extrapolated from all the other types of studies (case report, retrospective, control case and guidelines) comparing the type and number of patients, the type of incision and the technique used in an open approach, the suture materials and the suturing technique and, finally, if mentioned, episodes of recurrence and/or complications.
1. Analysis of the reviews. 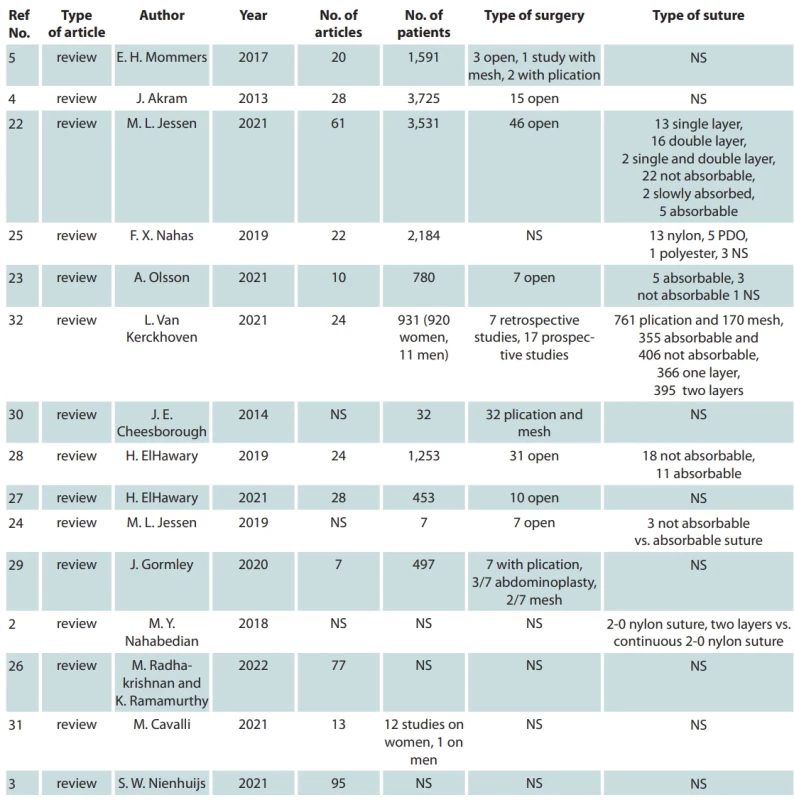
NS – not stated, PDO – polydioxanone 2. Analysis of articles. 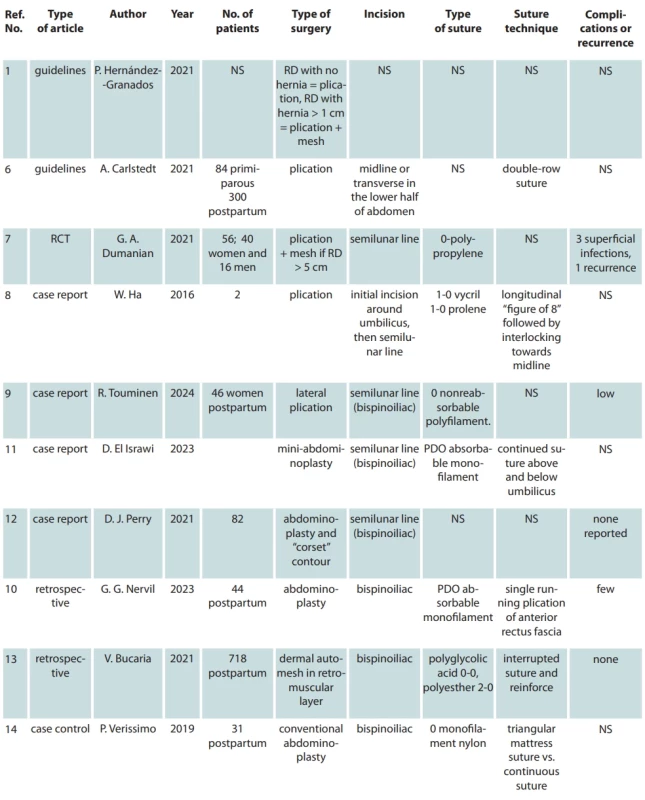
NS – not stated, PDO – polydioxanone, RCT – randomized control trial, RD – rectus diastasis Tab. 2 – continuing. Analysis of articles. 
prolekare.web.text.media.image_type_Other.en NS – not stated, PDO – polydioxanone, RCT – randomized control trial, RD – rectus diastasis Two of these articles are guidelines that recommend a double-layer plication if the RD is < 1 cm, while if the defect is > 1 cm they also recommend the application of mesh [1,6].
Dumanian and Moradian talk about the use of mesh in moderate and severe diastasis in both men and women, demonstrating that the best suture is transfascial and close to the semilunar line [7].
In their case report on two Korean women, Ha et al. show a multiple longitudinal plication approach of the abdominal wall with absorbable thread [8].
Tuominen et al. describe the experience with hydrodissection and epidural anesthesia for lateral plication modification of abdominoplasty to restore abdominal wall firmness [9].
El Israwi and Watfa explain a modified mini-abdominoplasty [11], while Perry and Driscall reinforce the plication with an autograft taken from the removed adipose-skin flap calling the technique “corset contour” [12].
Nervil et al. argue as using a single running plication of the anterior rectus fascia with a slowly absorbable suture gives a fair cosmetic result, excellent effect on symptoms, few complications and high levels of patient satisfaction [10].
Bucaria and Boccuzzi offer an alternative to mesh with a dermal graft which is easy to handle, has demonstrated comparable tensile strength to alloplastic mesh and is available in abdominoplasty or mini abdominoplasty from the excised skin [13].
Veríssimo et al. show how the use of triangular mattress sutures significantly reduces the length of the aponeurosis of the rectus muscle [14].
Gama et al. state at the end of his randomised study that the repair of single-layer straights with non-absorbable thread is much faster and with efficiency comparable to the classic technique [15].
Nahas et al. bring a correction of the technique by plicating the posterior sheaths of the rectus after their advancement in patients who have recurrence because they have a congenital mutation of the muscle insertion [16].
In their case-control study, Mestak et al. conclude by saying that the rectus sheath plication using absorbable sutures in patients with the diastasis of rectal muscles is a reliable method that maintains the long-term stability of the abdominal wall. The same conclusion is reached by Nahas et al. in their retrospective study [17,18].
In their case report, Gallus et al. demonstrate how plication surgery is not only aesthetic but also functional, so much so that postpartum women with RD can be enrolled in the US Navy [19].
Rosen and Hartman conclude his retrospective study by stating that long-acting absorbable barbed or smooth sutures appear to be equally effective in maintaining rectus diastasis repair [20].
Finally, with their retrospective study on the treatment of RD in conjunction with hernia, Köhler et al. say that patients with rectus diastasis and absorbable sutures have a tenfold higher risk for recurrence compared to those without rectus diastasis and nonabsorbable sutures [21].
Definition of outcomes
The first outcome of the study concerns the evaluation of the different existing open techniques for the treatment of diastasis recti and the comparison of these in terms of material used, complications and recurrence rate.
The second outcome aims to analyze whether there are differences in terms of anatomical characteristics of diastasis in post-bariatric and postpartum patients and any differences in surgical treatment.
Diastasis recti is a common condition in post-bariatric patients and post-pregnancy patients. Surgical management takes over when a conservative approach is not possible. There are several classifications available in the literature, but there is not unequivocally recognized one.
Diastasis recti can be classified by patient characteristics: T1 (post-pregnancy) and T2 (for adiposity); by size of the defect in D1 (between 2 and 3 cm), D2 (between 3 and 5 cm) and D3 (> 5 cm); finally for the concomitant presence of hernia (H1) or absence (H0) [1]. A further classification is the Nahas classification which identifies four types of diastasis aesthetics: type A, post-pregnancy DRAM (diastasis of rectus abdominus muscle); type B, DRAM and lateral and infraumbilical aponeurosis laxity; type C, congenital lateral insertion of the rectus abdominis muscles; and type D, DRAM combined with a poor waist circumference [4,5]. Other classifications are the Beer and the Rath [2,4].
Mostly, RD is acquired with central/visceral obesity and pregnancy being the two main etiological factors of its incidence [22]. The congenital forms caused by autosomal dominant transmissions are due to syndromes that involve alterations in the quality of collagen present in the body, associating, in these cases, with joint aneurysms and laxity, as in Ehler-Danlos syndrome [3]. A not uncommon malformation of the insertion of the rectus on the lateral costal margin has also been reported, causing post-treatment relapsing diastasis, which requires plication of the posterior sheaths of the rectus after their advancement, to obtain a definitive resolution of the diastasis [16].
The use of surgery makes it possible to eliminate the distance between the rectus muscles and restore the continuity of the abdominal wall. Rectus plication is the most widely used surgical technique and is often performed at the same time as a tummy tuck, to improve the aesthetic result of the abdomen and improve the patient’s quality of life.
Surgical technique
When a conservative approach is not possible, the surgical technique represents a valid alternative in improving the symptoms associated with diastasis recti such as lower back pain, urinary incontinence and quality of life [23,24]. The surgical technique available for DR is rectus plication and if there is a concomitant hernia, a combined diastasis and hernia repair technique is used. Plication of the anterior wall of the rectus is the main technique currently used. It consists of pinching the anterior abdominal wall and in most cases is conducted vertically and allows the attenuated linea alba to be delineated [2]. Some studies suggest horizontal, curved, fusiform or H-shaped techniques in the external oblique aponeurosis during plication [25]. In patients with significant anterior rectus sheath laxity, lateral plication on both sides can also be performed to further improve and firm the abdominal contour [2]. In the case of concomitant hernias, for defects < 1 cm the direct plication is sufficient for the correction of the defect, for higher values the use of a mesh is necessary [1].
The plication of the rectus can take place in the open technique, laparoscopic or a combination of the above. The open approach, defined as “according to Pitanguy”, is the most widely used in plastic surgery and consists of a transverse suprapubic incision that joins the two iliac spines. The lifting of the abdominal flap with an upper base allows the visualization of the linea alba and the rectus muscles. Other types of incisions are also possible, such as supraumbilical incisions, used when there are coexisting conditions such as nephrectomy or hernia [7,24,26]. There is also the left suprapubic incision extended 2–3 cm upwards and the median incision extending from the xiphoid process to the pubic area, which is useful when choosing to perform an inverted T abdominoplasty [24,26]. The open technique compared to the laparoscopic technique offers better visualization of the linea alba and the possibility of removing excess skin. However, it is still associated with a higher rate of complications, greater postoperative pain, and larger scarring [27].
A study reports a differentiation of techniques based on sex, preferring the Pitanguy technique in females and the vertical one in males [7].
Plication can be conducted with interrupted suture, interrupted mattress suture or continuous suture [22]. The interrupted suture technique has always been the most common and one of the first to be developed, but it is associated with longer operative times than the continuous one. In addition, plication can be performed with or without mesh reinforcement depending on whether there is a concomitant hernia.
Triangular mattress techniques have been developed to contain the epigastric bulge that was seen in some patients treated with detached sutures.
Plication can be conducted in a single layer or in several layers with a combination or not of detached or continuous suture. The times in the mentioned technique are up to 50% shorter than in the multi-layer technique without having any consequences in tension and resistance over time [15]. Although there are no differences in terms of recurrence in the use of the single-layer or double-layer technique, it appears that the double-layer technique is associated with a lower number of complications [28].
The suture can be absorbable, slowly absorbable or non-absorbable. Some studies comparing the use of notched monofilament with absorbable non-serrated monofilament show a higher recurrence rate in the former case, probably related to the muscle tearing effect that occurs in the passage of the thread into the muscle during plication [25]. This material can also cause more frequent post-operative complications such as seroma and hematoma [20]. Hassan et al. also report a case of diastasis recti conducted with a paper clip, considering it fast in execution and effective in holding [28].
The most used suture as absorbable suture is polyglactin 910 and polydioxanone while the most frequent non-absorbable sutures are polyamide, polypropylene, and polyester [25].
Case-control studies show that even an absorbable suture such as ethicon polydioxanone 2-0 can give stable results in the long term [17].
There are no differences in terms of recurrence between a non-absorbable and a absorbable suture material [24,28]; however, the literature shows that often a non-absorbable suture can generate a greater inflammatory effect, greater palpability in the postoperative period and is associated with a greater persistence of postoperative pain along the midline [25]. In addition, an absorbable thread can facilitate the recurrence of periumbilical and epigastric hernias along with other factors such as obesity and wound infections [21].
The choice of wire size must consider the fact that the knot is tightened the greater the diameter of the wire itself. Therefore, sutures that are too thin tend to tear the aponeurosis and this is the main cause of recurrence of diastasis recti. Thus, choosing a suture thread size ranging from 0 to 2-0 tends to be the most appropriate choice. However, it should be considered that sutures that are too large can lead to the development of granulomas, so these characteristics should be considered when choosing the thread size. There is no evidence to support the use of antibiotic-soaked threads in reducing infection rates in the correction of diastasis recti [25].
Finally, from the current literature, it is not clear whether the plication of the rectus is able to increase abdominal strength as existing studies do not consider the different severity of the diastasis. It can be agreed that rectus plication contributes in terms of improving abdominal function but not muscle strength. It would seem that in the case of a hernia, mesh reinforcement contributes to both trunk reinforcement and abdominal wall functionality [29].
Some authors have questioned the duration of plication alone, suggesting as an alternative a reinforcement with mesh in the submuscular plane.
This technique would seem to be safer in patients who have had a 100% recurrence of musculoaponeurotic laxity at one year after surgery, especially multiparous women with severe abdominal wall laxity [30].
Vertical abdominoplasty allows for greater waist shrinkage and more adequate removal of excess fat from the epigastric region, as well as the creation of a new navel [30]. Therefore, the choice of the type of surgical technique should consider the type of myoaponeurotic deformity according to the Nahas classification [4].
Moreover, Perry and Driscoll suggest an alternative surgical technique called “autodermic corset” performed through the aid of an autograft taken from the abdominal panniculus normally removed and inserted under tension between the semilunar lines as a corset, to reduce the recurrence of RD and abdominal hernias [12].
Complications
The surgical complications related to the plication of the rectus, whether performed with the laparoscopic technique or with the open technique, are many: infections, sensory disturbances, flap necrosis, seroma formation, local wound complications and recurrence [2,4,22]. Common complications include seroma, wound dehiscence, and minor bleeding episodes [27,29]. There is no evidence of difference in terms of complications or recurrences from the comparison of the use of various techniques [22,28]. In addition, significant diastasis recti can contribute to the loss of abdominal function and not allow an adequate Valsalva maneuver [30].
The aspect that most worries patients is post-operative pain. Studies in the literature comparing postoperative pain in the various techniques show that there are minimal differences. However, it must be considered that the analysis of pain in the various studies currently present takes place in a non-standardized way. On the contrary, however, it is possible to conclude that in most cases the use of mild analgesics is sufficient to contain post-operative pain [22].
Finally, it must be borne in mind never to perform too stringent plications in order not to compromise the patient’s ventilation [25].
From the current literature there is no difference in terms of postoperative complications between the above-mentioned techniques, therefore it is not possible at present to identify a superiority of one technique over another [5,22,28].
Etiological differences
There are not enough studies to highlight the differences between men and women, but it is commonly believed that the pathophysiology underlying the process is different in the two sexes.
In post-pregnancy DRAM, collagen remodeling induced by the hormone relaxin during pregnancy seems to play a predominant role by directly stimulating matrix metalloproteases [3,5]. The viscoelastic properties of collagen allow the linea alba to increase its length when subjected to prolonged mechanical stress, as occurs in the case of a constant increase in intra-abdominal pressure. The progressive growth of the fetus inside the uterus together with hormonal changes (increased secretion of relaxin, progesterone and estrogen) in the connective tissue, creates a physiological enlargement between the rectus, which can cause diastasis during pregnancy [31].
The midline conjunction weakens as the components of the extracellular matrix change due to the altered progesterone-estradiol balance and corticosterone release [3].
In most cases, this phenomenon regresses spontaneously after pregnancy, restoring, albeit partially, the continuity of the abdominal wall. Small or highly trained women, as well as those with twin pregnancies, are more at risk [3]. In these, an incidence of diastasis emerged in 66% of cases during the third trimester of gestation and in 33% during the postpartum period [22]. Current data report that one in three women still experience the presence of this midline separation one year after childbirth [3,23,31].
Currently, a statistically significant incidence relative to the age of pregnant women does not seem to emerge, although a slight prevalence in young women has been emphasized in several reviews [31]. Therefore, based on these considerations, surgery in postpartum women should be considered from six to twelve months after delivery, as in some patients it tends to resolve spontaneously [24]. According to other studies, the waiting time before surgery is 2 years [6]. Therefore, pregnancy is confirmed as a risk factor for the development of diastasis and increases with the number of pregnancies. Caesarean section is a risk factor only in the case of a second pregnancy [31].
The increase in intraabdominal pressure caused by increased weight and BMI explains how diastasis recti is a prevalent condition even in obese people. The increase in visceral fat, characteristically male, in fact, leads to an accumulation of adipose tissue in the mesentery and in the greater omentum, associated with a marked loss of muscle thus generating pressure on the rectus muscles, which together with the reduction of collagen in the linea alba above the navel in severely obese patients, causes a separation, explaining the onset of this condition in patients with high BMI [31]. Male diastasis rectus develops more frequently because of increased intra-abdominal fat volume, especially in the supraumbilical region, and occurs from the fifth to the sixth decade of life [30].
Finally, diabetes mellitus appears to be an additional risk factor associated with generalized sarcopenia [31].
Recent cadaveric studies have also shown a structural difference in the linea alba between male and female individuals, showing a predisposition to diastasis in the former. In nulliparous females, compared to males, a greater amount of transverse collagen fibers was found, both in the upper (hypogastric) and in the middle (infra-umbilical) portion, while no differences were found in the lower segment. This disparity translates into a different aponeurotic thickness between the two sexes, both at rest and in the curl-up position [31]. In women, the fiber levels of the linea alba are twice that of a man [3].
In humans, the genetic component seems to have a greater weight [5]. Some authors believe that the male abdominal wall is more rigid, explaining the higher percentage of cases of diastasis and concomitant hernia in this sex [30].
Conclusions
Considering the current literature and the quality of the studies present, there is insufficient evidence to support the choice of one surgical technique over another (plication vs mesh) nor the recurrence rate in the case of absorbable or non-absorbable sutures. There is a greater recurrence for the use of absorbable sutures, but further studies are needed.
Therefore, the choice of the type of surgical approach and the type of suture to be used remains a decision of the surgeon based on his preferences and skills. The choice of technique also considers the patient’s characteristics such as the presence of excess skin or the presence of a concomitant hernia.
The current literature considers the surgical approach a safe and adequate choice for the treatment of diastasis recti especially when combined with excess abdominal skin or in the presence of a concomitant hernia. The conservative approach should only be considered if there is no serious functional impediment or when the patient decides not to undergo surgery. Furthermore, our review did not bring to light different surgical indications depending on the etiology or sex of the patient. It is now common opinion that the basic pathophysiology differs in different conditions. Therefore, subsequent studies should highlight these differences and seek the best surgical approach for each underlying condition.
Limits
The limitations of this study relate to the linguistic bias for the exclusion of non-English articles that may have been relevant to the purpose of the review. In addition, many studies do not report adequate information about the technique used or the characteristics of the suture threads. In addition, many studies do not specify patient characteristics such as gender, BMI, and pregnancies. Moreover, not every study is public, so it has not been possible to include some papers in this review. Finally, the quality of prospective studies is often very low and with a limited number of patients.
Roles of authors
All authors have been actively involved in the planning, preparation, analysis and interpretation of the findings, enactment and processing of the article with the same contribution.
Disclosure
Registration and protocol: not registered and not prepared
Funding: none
Conflicts of interest: none declared
Ethical approval: not required
Sources
1. Hernández-Granados P., Henriksen NA., Berrevoet F., et al. European Hernia Society guidelines on management of rectus diastasis. Br J Surg. 2021, 108 (10): 1189–1191.
2. Nahabedian MY. Management strategies for diastasis recti. Semin Plast Surg. 2018, 32 (3): 147–154.
3. Nienhuijs SW., Berkvens EHM., de Vries Reilingh TS., et al. The male rectus diastasis: a different concept? Hernia. 2021, 25 (4): 951–956.
4. Akram J., Matzen SH. Rectus abdominis diastasis. J Plast Surg Hand Surg. 2014, 48 (3): 163–169.
5. Mommers EHH., Ponten JEH., Al Omar AK., et al. The general surgeon’s perspective of rectus diastasis. A systematic review of treatment options. Surg Endosc. 2017, 31 (12): 4934–4949.
6. Carlstedt A., Bringman S., Egberth M., et al. Management of diastasis of the rectus abdominis muscles: recommendations for swedish national guidelines. Scand J Surg. 2021, 110 (3): 452–459.
7. Dumanian GA., Moradian S. Mesh abdominoplasty for rectus diastasis in women and men. Hernia. 2021, 25 (4): 863–870.
8. Ha W., Song SY., Yoon CS., et al. Severe irreversible diastasis recti abdominis and abdominal hernia in postpartum women: rare case report. Int Surg. 2016.
9. Tuominen R., Peltoniemi H., Jahkola T., et al. An abdominoplasty modification for postpregnancy abdomen with rectus diastasis and midline hernia: the technique and results. Plast Reconstr Surg. 2024, 153 (6): 1111e–1115e.
10. Nervil GG., Paulsen JF., Kalstrup J., et al. Simple plication alleviates physical symptoms in patients with post-gestational rectus diastasis. Hernia. 2023, 27 (4): 957–968.
11. El Israwi D., Watfa W. Rectus muscle plication in mini-abdominoplasty with umbilicus preservation. Plast Reconstr Surg Glob Open. 2023, 11 (5): e4998.
12. Perry DJ., Driscoll DN. Corset autodermis external obliqueplasty reinforcement of rectus diastasis and umbilical hernia repairs during abdominoplasty. Plast Reconstr Surg. 2021, 147 (4): 860–863.
13. Bucaria V., Boccuzzi A. Autologous dermal mesh in severe postpregnancy recti muscles diastasis. Aesthetic Plast Surg. 2021, 45 (1): 198–211.
14. Veríssimo P., Nahas FX., Barbosa MV., et al. Is it possible to repair diastasis recti and shorten the aponeurosis at the same time? Aesthetic Plast Surg. 2014, 38 (2): 379–386.
15. Gama LJM., Barbosa MVJ., Czapkowski A., et al. Single-layer plication for repair of diastasis recti: the most rapid and efficient technique. Aesthet Surg J. 2017, 37 (6): 698–705.
16. Nahas FX., Ferreira LM., de Arimatéia Mendes J. An efficient way to correct recurrent rectus diastasis. Aesthetic Plast Surg. 2004, 28 (4): 189–196.
17. Mestak O., Kullac R., Mestak J., et al. Evaluation of the long-term stability of sheath plication using absorbable sutures in 51 patients with diastasis of the recti muscles: an ultrasonographic study. Plast Reconstr Surg. 2012, 130 (5): 714e–719e.
18. Nahas FX., Ferreira LM., Augusto SM., et al. Long-term follow-up of correction of rectus diastasis. Plast Reconstr Surg. 2005, 115 (6): 1736–1741.
19. Gallus KM., Golberg KF., Field R. Functional improvement following diastasis rectus abdominus repair in an active duty navy female. Mil Med. 2016, 181 (8): e952–e954.
20. Rosen A., Hartman T. Repair of the midline fascial defect in abdominoplasty with long-acting barbed and smooth absorbable sutures. Aesthet Surg J. 2011, 31 (6): 668–673.
21. Köhler G., Luketina RR., Emmanuel K. Sutured repair of primary small umbilical and epigastric hernias: concomitant rectus diastasis is a significant risk factor for recurrence. World J Surg. 2015, 39 (1): 121–126.
22. Jessen ML., Öberg S., Rosenberg J. Surgical techniques for repair of abdominal rectus diastasis: a scoping review. J Plast Surg Hand Surg. 2021, 55 (4): 195–201.
23. Olsson A., Kiwanuka O., Sandblom G., et al. Evaluation of functional outcomes following rectus diastasis repair-an up-to-date literature review. Hernia. 2021, 25 (4): 905–914.
24. Jessen ML., Öberg S., Rosenberg J. Treatment options for abdominal rectus diastasis. Front Surg. 2019, 6 : 65.
25. Nahas FX., Faustino LD., Ferreira LM. Abdominal wall plication and correction of deformities of the myoaponeurotic layer: focusing on materials and techniques used for synthesis. Aesthet Surg J. 2019, 39 (Suppl 2): S78–S84.
26. Radhakrishnan M., Ramamurthy K. Efficacy and challenges in the treatment of diastasis recti abdominis – a scoping review on the current trends and future perspectives. Diagnostics (Basel). 2022, 12 (9): 2044.
27. ElHawary H., Barone N., Zammit D., et al. Closing the gap: evidence-based surgical treatment of rectus diastasis associated with abdominal wall hernias. Hernia. 2021, 25 (4): 827–853.
28. ElHawary H., Abdelhamid K., Meng F., et al. A comprehensive, evidence-based literature review of the surgical treatment of rectus diastasis. Plast Reconstr Surg. 2020, 146 (5): 1151–1164.
29. Gormley J., Copeland A., Augustine H., et al. Impact of rectus diastasis repair on abdominal strength and function: a systematic review. Cureus. 2020, 12 (12): e12358.
30. Cheesborough JE., Dumanian GA. Simultaneous prosthetic mesh abdominal wall reconstruction with abdominoplasty for ventral hernia and severe rectus diastasis repairs. Plast Reconstr Surg. 2015, 135 (1): 268–276.
31. Cavalli M., Aiolfi A., Bruni PG., et al. Prevalence and risk factors for diastasis recti abdominis: a review and proposal of a new anatomical variation. Hernia. 2021, 25 (4): 883–890.
32. Van Kerckhoven L., Nevens T., Van De Winkel N., et al. Treatment of rectus diastasis: should the midline always be reinforced with mesh? A systematic review. J Plast Reconstr Aesthet Surg. 2021, 74 (8): 1870–1880.
33. Borud LJ., Grunwaldt L., Janz B., et al. Components separation combined with abdominal wall plication for repair of large abdominal wall hernias following bariatric surgery. Plast Reconstr Surg. 2007, 119 (6): 1792–1798.
34. Uzair S., Babar Z., Sutton PA. Tissue regeneration mesh reinforcement during abdominoplasty for severe myoaponeurotic laxity after pregnancy. BMJ Case Rep. 2013, 2013: bcr2013010306.
35. Jagric T., Hazabent M. The “scarless ab-lift”: a novel method for the treatment of skin laxity with rectus muscle diastasis. Aesthetic Plast Surg. 2025, 49 (5): 1649–1651.
36. Emanuelsson P., Gunnarsson U., Dahlstrand U., et al. Operative correction of abdominal rectus diastasis (ARD) reduces pain and improves abdominal wall muscle strength: a randomized, prospective trial comparing retromuscular mesh repair to double-row, self-retaining sutures. Surgery. 2016, 160 (5): 1367–1375.
Stefano Uderzo
VIa Casetti 82 bis, 28865 Crevoladossola (VB), Italy
stefanouderzo@gmail.com
Submitted: 22. 3. 2025
Accepted: 23. 11. 2025
Labels
Plastic surgery Orthopaedics Burns medicine Traumatology
Article was published inActa chirurgiae plasticae

2025 Issue 4-
All articles in this issue
- Will robots replace us?
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
- Intraoperative cone beam computed tomography in craniomaxillofacial traumatology – a case report
- Digital retractile keloid in a context of spontaneous keloids – a case report
- Extensive keloid scar of the left auricle – combined treatment of excision followed by brachytherapy: a case report
- Post-otoplasty keloid scars – treatment strategies and case reports
- Large urethral false passage during a routine catheterization – low threshold for better outcome
- Acta chirurgiae plasticae
- Journal archive
- Current issue
- Online only
- About the journal
Most read in this issue- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career


