-
Medical journals
- Career
Extensive keloid scar of the left auricle – combined treatment of excision followed by brachytherapy: a case report
Authors: J. Fau 1; P. Vítek 2; K. Procházková 1; P. Kurial 1; T. Votruba 1; P. Vodička 1; V. Mařík 1
Authors‘ workplace: Department of Plastic Surgery, Hospital České Budějovice, Czech Republic 1; Department of Oncology, Hospital České Budějovice, Czech Republic 2
Published in: ACTA CHIRURGIAE PLASTICAE, 67, 4, 2025, pp. 264-267
doi: https://doi.org/10.48095/ccachp2025264Introduction
Keloid scars present a significant challenge in surgical practice. This is a type of scar that arises from disorganized fibroproliferative collagen that extends beyond the edges of the original wound. It results from abnormal production of extracellular matrix [1]. Keloid scars are more prevalent in individuals of African, Hispanic, and Asian descent, suggesting a genetic predisposition associated with pigmentation and other hereditary factors [2].
While for most minor keloid scars we start with intralesional steroid application, which is a relatively quick and conservative treatment with often good results, for extensive findings we have to choose a combined strategy. This case report describes the details of the treatment of a 32-year-old female patient with an extensive keloid on the left earlobe after a piercing, utilizing a combined approach of surgical excision and brachytherapy.
Description of the case
A Vietnamese-origin female patient presents to the plastic surgery outpatient clinic (June 2023) with a mass in her left auricle that has been enlarging for several years. Given the reported history of piercing, it was obvious from the beginning that it was a keloid scar (Fig. 1). Considering the extent of the scar, the patient was indicated for combined therapy, i.e. excision followed by brachytherapy. The operation took place under local anaesthesia during hospitalization. After the initial marking, we performed the excision of the keloid into healthy tissue while leaving the intact cartilage of the helix of the left auricle at the base. After removing the pedunculated keloid, we sent the specimen for histology. An oval defect of 3 × 1,5 cm forms after the excision. Using previous hydrodissection and subsequent preparation, we released the skin cover from both the ventral and dorsal sides of the auricle, inserted a catheter into the dermal layer along the entire length of the wound for postoperative brachytherapy targeting, and sutured the skin over the defect and catheter. The catheter was secured to the skin with a button to prevent loosening during manipulation (Fig. 2). Immediately after the operation, we referred the patient for the first fraction of brachytherapy. The brachytherapy itself, i.e., fractionated irradiation with a high dose rate (HDR) Ir-192 source, was carried out at the oncology department in three fractions: the first session immediately after surgery, the second session six hours later, and the third 24 hours after the second session, i.e. on the following day. After completing the third fraction, we extracted the wire and discharged the patient home and for subsequent outpatient care. Histological findings confirmed our diagnosis of a keloid scar. The effect was already noticeable with calm primary wound healing at suture removal (14 days post-operation). The patient was instructed on the importance of meticulous scar care, which includes maintaining cleanliness of the scar, performing regular pressure massages, utilizing silicone gels or sheets, ensuring adequate hydration, and protecting the scar from sun exposure. One year post-operation, the patient came for an evaluation of the medium-term treatment effect (Fig. 3). Both the patient and the medical team were very satisfied with the result.
1. Keloid of the left earlobe. 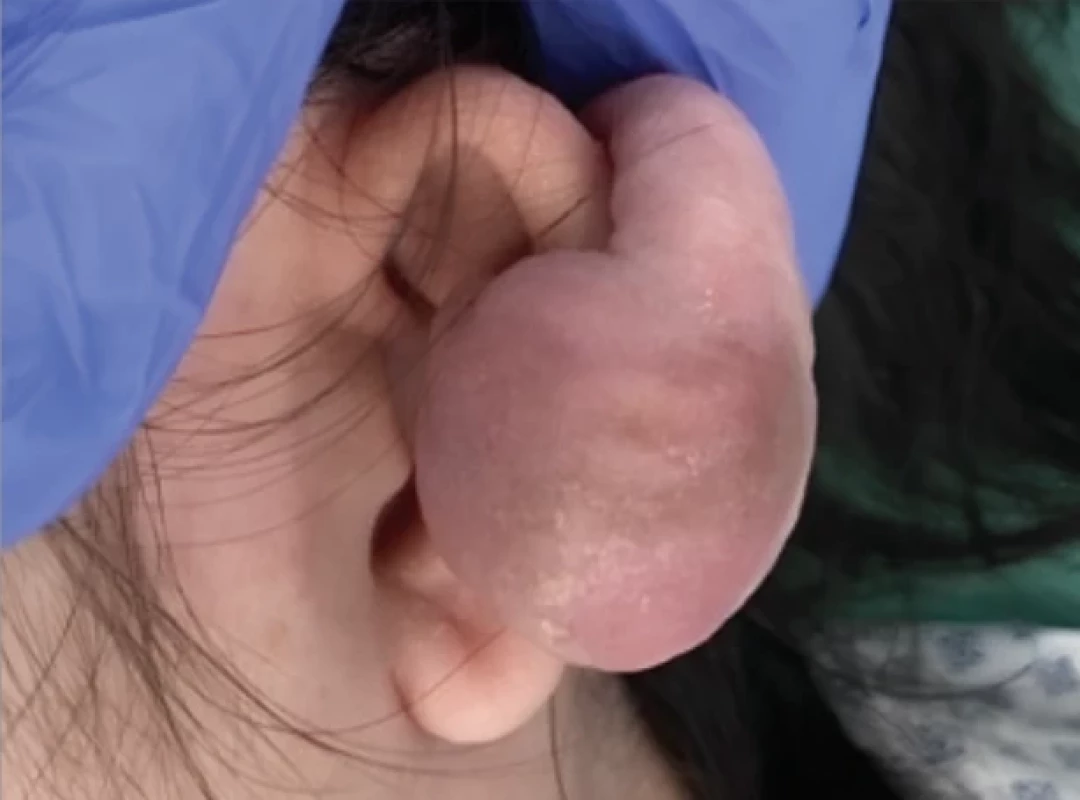
2. Result at the end of the surgery after insertion of a catheter for subsequent brachytherapy. 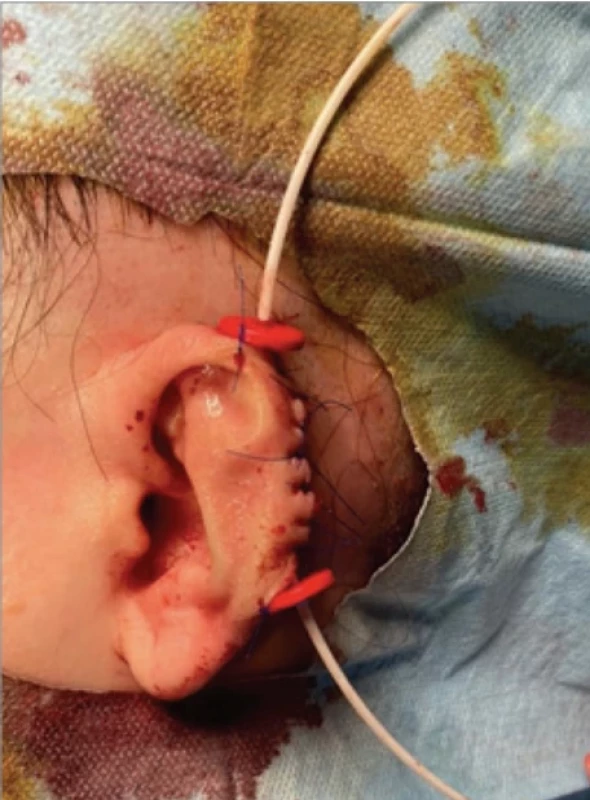
3. One year after the combined procedure. 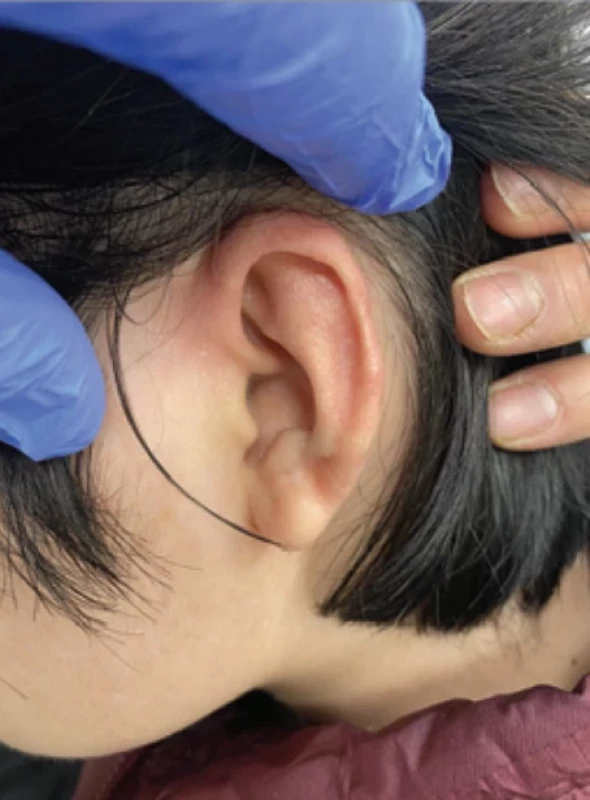
Discussion
Despite all the treatment options (Tab. 1) for this kind of skin lesion (medical and surgical therapies, such as intralesional steroid injection and surgical excision), the percentage of recurrence is still high [1]. Surgical excision remains a cornerstone in the treatment of keloids, particularly for symptomatic lesions or those causing aesthetic concerns. The excision down to the cartilage is critical to ensure complete removal of the keloid tissue while preserving surrounding structures. The recurrence rate of keloids following only surgical treatment can be quite high [3]. To address the high recurrence rates associated with surgical excision, brachytherapy was employed as an adjunctive treatment. This localized form of radiation therapy targets residual keloid cells that may remain post-surgery [4]. According to our oncological department, the recommended timing for brachytherapy is immediately after the surgical excision of the keloid. The isodose (a curve representing points of equal radiation dose) is measured at a 0.5 cm distance from the centre of the applicator and its length does not extend beyond the entry and exit edges of the wound. The dose per fraction ranges from 4 to 6 Gy. In our case, the patient received three fractions of radiation, a strategy aligned with current best practices that aims to enhance long-term efficacy [5]. This approach aims to reduce the high recurrence rate typically associated with keloid excision alone by delivering targeted radiation to the area, thus inhibiting the regrowth of keloid tissue [4]. According to the sources, surgical excision of keloids alone tends to have a recurrence rate of approximately 45–100% [3]. In comparison, post-operative brachytherapy has the recurrence rate of 15% [1]. This multifaceted strategy addresses both the immediate physical concerns of the keloid and aims to significantly reduce the likelihood of recurrence.
The combined method is discussed as an effective strategy particularly beneficial for patients who have a history of recurrent keloids or larger lesions. Additionally, the synergy between surgical excision and subsequent brachytherapy significantly enhances the overall efficacy of the treatment [6]. Meanwhile, the positive outcome observed in this case supports the growing evidence advocating for combined treatment modalities in keloid management. In summary, the presented case highlights the effectiveness of the combination of surgical excision with brachytherapy in the treatment of keloid scars. This approach not only minimizes recurrence but also significantly increases patient satisfaction and quality of life.
The efficacy of ear keloid treatment profoundly influences patients’ psychological well-being and self-assurance. To further diminish the long-term recurrence rate of keloid and achieve optimal aesthetic outcomes, intraoperative meticulous suturing, comprehensive keloid tissue removal, postoperative radiotherapy (including intervention timing, frequency, and total dosage) are essential [7]. For the objective assessment of preoperative and postoperative findings, the Vancouver Scar Scale is employed (Tab. 2). On the other hand, some authors may mention the risk of carcinogenesis with the use of brachytherapy, but the risk of carcinogenesis attributable to treatment with radiotherapy in keloid scars is very low and acceptable for this treatment modality [8]. Further studies and clinical trials will be necessary to refine these strategies and improve outcomes in patients with keloid scars.
1. Effi cacy of medical and surgical treatments on keloid scars. 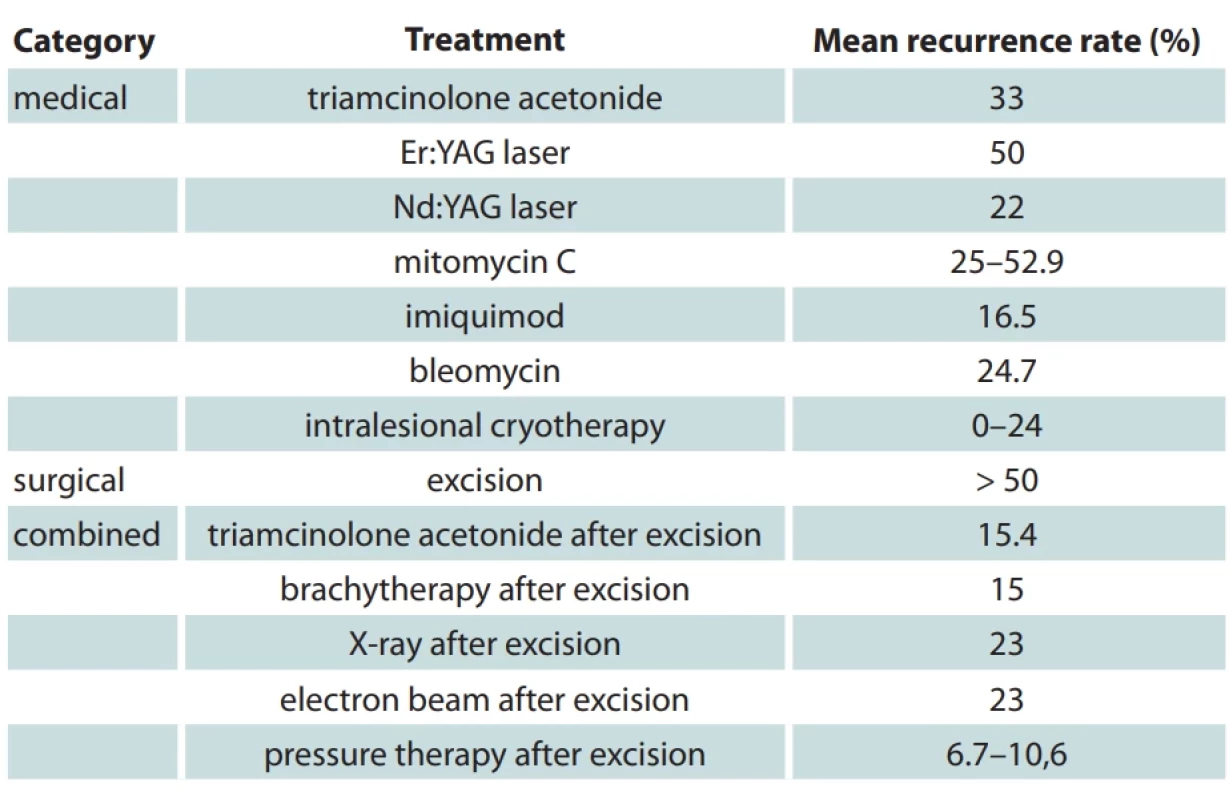
2. The Vancouver Scar Scale with patient assessment. 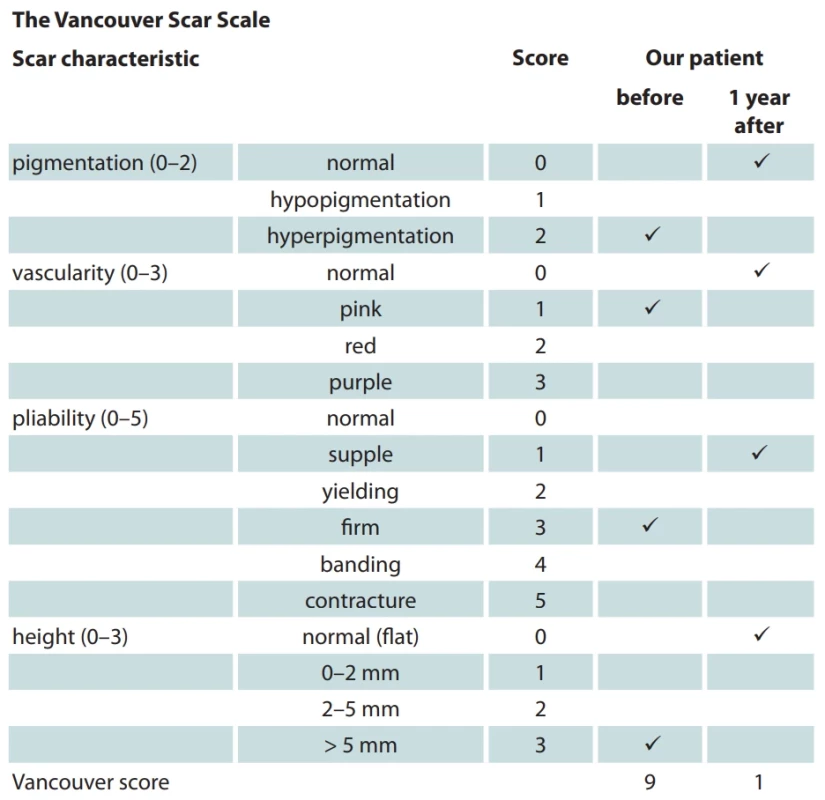
Conclusion
The combined approach of surgical excision followed by immediate postoperative brachytherapy proves to be an effective and reliable method in the treatment of extensive keloid scars, significantly reducing the risk of recurrence compared to surgery alone. In the presented case of a large auricular keloid, this strategy led to excellent medium-term outcomes, with high patient and medical team satisfaction. Emphasis on meticulous surgical technique, timely initiation of radiotherapy, and diligent postoperative scar care is essential for achieving optimal aesthetic and functional results. Although there is a minimal risk associated with radiation therapy, the benefits of this combined modality clearly predominate.
Roles of the authors
Jakub Fau – surgeon, author, article creator; Petr Vítek – article consultant, oncologist; Vladimír Mařík – article consultant, review and editing, advisor, Kristýna Procházková, Pavel Kurial, Tomáš Votruba, Petr Vodička – review and editing
Disclosure
The authors of this case report declare that there are no conflicts of interest regarding the publication of this report. All aspects of the study, including the collection, analysis, and interpretation of data, as well as the preparation of the manuscript, were conducted independently of any commercial or financial relationships that could be construed as a potential conflict of interest.
Note
The photographs presented in this article were taken by the author with the explicit consent of the patient. All necessary precautions were taken to ensure patient confidentiality and anonymity in accordance with ethical guidelines for medical publications.
Sources
1. Ekstein SF., Wyles SP., Moran SL., et al. A review of therapeutic management. Intl J Dermatol. 2021, 60 (6): 661–671.
2. Greene CA., Hampton G., Jaworski J., et al. Multi-ancestry meta-analysis of keloids uncovers novel susceptibility loci in diverse populations. Nat Commun 2025, 16 (1): 7770.
3. Luo PM, Glass Ii DA 2nd. Keloid management: a review of treatment modalities. Ital J Dermatol Venerol. 2025, 160 (1): 29–39.
4. Rockwell WB, Cohen IK, Ehrlich HP. Keloids and hypertrophic scars: a comprehensive review. Plast Reconstr Surg. 1989, 84 (5): 827–837.
5. Bijlard E., Verduijn GM., Harmeling JX., et al. Optimal high-dose-rate brachytherapy fractionation scheme after keloid excision: a retrospective multicenter comparison of recurrence rates and complications. Int J Radiat Oncol Biol Phys. 2018, 100 (3): 679–686.
6. Al-Attar A., Mess S., Thomassen J. Keloid pathogenesis and treatment. Plast Reconstr Surg. 2006, 117 (1): 286–300.
7. Tan Q., Xu J., Xu W., et al. Surgery and superficial x-ray radiotherapy for keloids of the preauricular and contralateral ear lobe: Case report. Clin Case Rep. 2024, 12 (4): e8657.
8. Barragán VV., García AI., García JF., et al. Perioperative interstitial high-dose-rate brachytherapy for keloids scar. J Contemp Brachytherapy. 2022, 14 (1): 29–34.
Jakub Fau, MD
Labels
Plastic surgery Orthopaedics Burns medicine Traumatology
Article was published inActa chirurgiae plasticae

2025 Issue 4-
All articles in this issue
- Will robots replace us?
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
- Intraoperative cone beam computed tomography in craniomaxillofacial traumatology – a case report
- Digital retractile keloid in a context of spontaneous keloids – a case report
- Extensive keloid scar of the left auricle – combined treatment of excision followed by brachytherapy: a case report
- Post-otoplasty keloid scars – treatment strategies and case reports
- Large urethral false passage during a routine catheterization – low threshold for better outcome
- Acta chirurgiae plasticae
- Journal archive
- Current issue
- Online only
- About the journal
Most read in this issue- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career

