-
Medical journals
- Career
Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
Authors: N. Hong Ha 1,2; T. T. Thanh Huyen 1,2
Authors‘ workplace: Department of Maxillofacial – Plastic – Aesthetic Surgery, Viet-Duc University Hospital, Hanoi, Vietnam 1; Department of Craniofacial and Plastic Aesthetic Surgery, University of Medicine and Pharmacy, Vietnam National University, Hanoi, Vietnam 2
Published in: ACTA CHIRURGIAE PLASTICAE, 67, 4, 2025, pp. 228-234
doi: https://doi.org/10.48095/ccachp2025228Introduction
Total external ear amputation is considered a rare injury. In many cases, microsurgical replantation is impossible because of the insufficient size of the blood vessel, and the extensive lesions of the auricular. Buncke and Schulz pioneered clinical studies on animal model regarding replanting an amputated ear in 1966 [1]. Fourteen years later, Pennington and his colleagues successfully performed the first human microsurgical auricular replantation [2]. In February 2012, at Viet Duc Hospital, we performed the first microsurgical auricular replantation in Vietnam. The patient was discharged after 9 days without any complications. At that time, there were only 5–6 rare success cases with no postoperative complications in the literature [3]. Since then, we have succeeded in four cases of total ear amputation. In the literature, there were about 60 successful microsurgical replantations reported [4,5].
Although the number of successful microsurgical replantations is still limited, there is yet no agreement upon a microsurgical auricular replantation strategy, such as patient position during surgery, surgeon position, which arterial and venous branches to choose for anastomoses, the order of anastomoses, and what to do in case venous anastomoses cannot be performed. That is the reason we want to propose our auricular replantation procedure based on our experience of 4 successful cases and a review of the literature on this rare injury.
1. Demographic data. 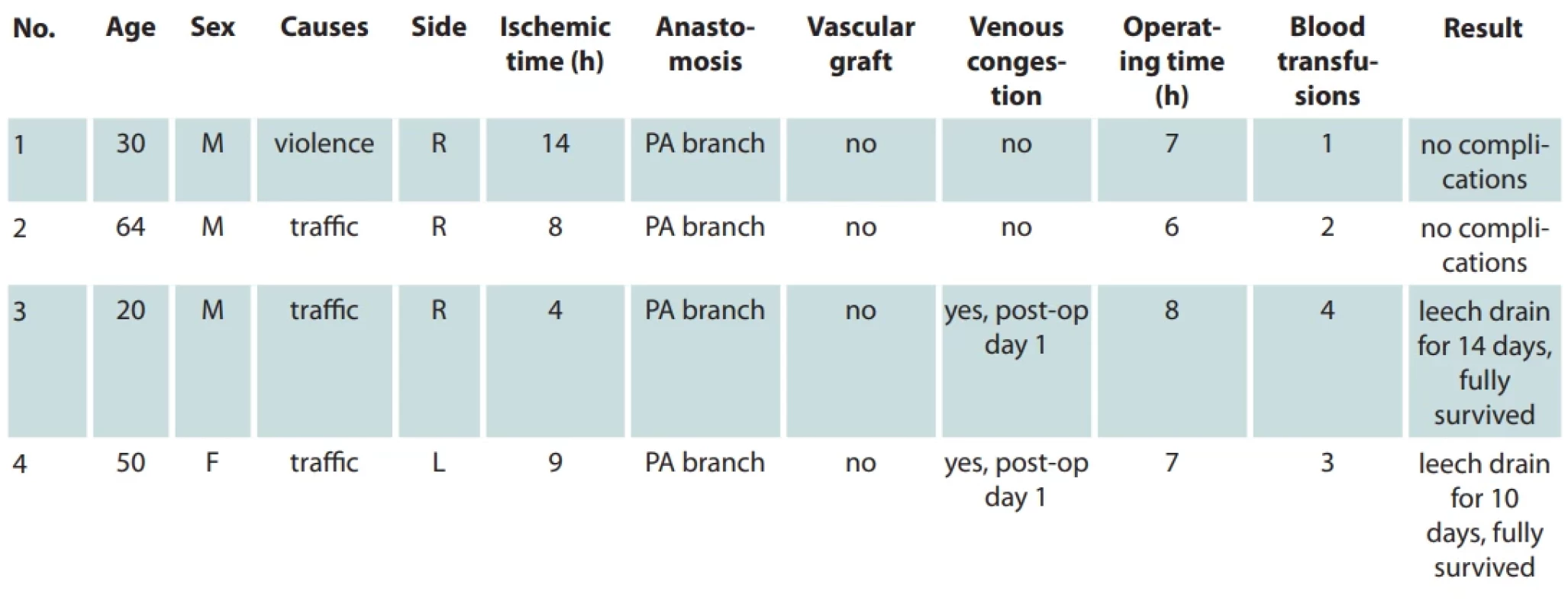
PA – proximal anastomosis Material and methods
We studied microsurgical auricle replantation performed at Vietduc Hospital, Hanoi, Vietnam from February 2012 to July 2022. Data included age, cause, duration of ischemia, patient position, sequence of vascular anastomosis, method of arterial/venous anastomosis/grafting, amount of blood transfused, total surgical time, and results.
Auricle blood supply
The blood supply to the ear is usually the superficial temporal artery (STA) and the posterior auricular artery (both are branches of the external carotid artery). The posterior auricular pedicle is particularly important because it supplies the posterior and anterior two-thirds of the ear. The veins draining the anterior and posterior ears are usually the superficial temporal vein and the posterior auricular vein [6].
Our ear replantation surgical protocol
Place the patient in a supine position, slightly contralaterally tilted, so that the microsurgical lens can look straight down, which facilitates microsurgery (Fig 1D, 2B). Two teams of surgeons: one team work on the amputated ear, and the other team dissects the scalp around the ear under a microscope to locate recipient vessels of sufficient size for direct anastomosis. Since the blood vessels are usually very small, we typically find the artery to anastomose first, and then wait for the backflow to find the location of the vein. After all the vessels that need to be anastomosed are exposed, we anchor the cutaneous layer behind the ear with a few 6.0 nylon stitches, leaving the exposed cartilage separated. This way, the microsurgery team can gain easy access and are more comfortable during anastomosis. After anastomoses are done, the cartilage and cutaneous layer are closed.
1. The fi rst total auricular replantation in Vietnam. (A,B) A 30-year-old male, total amputation of the right ear; (C) microsurgery; (D) after vascular dissection, the cartilages were left separated, providing a clear anterior view. The artery and vein were then anastomosed (diameter 0.4 mm); (E) 100% survival of the ear without any complications after surgery; (F) one week postoperative result. 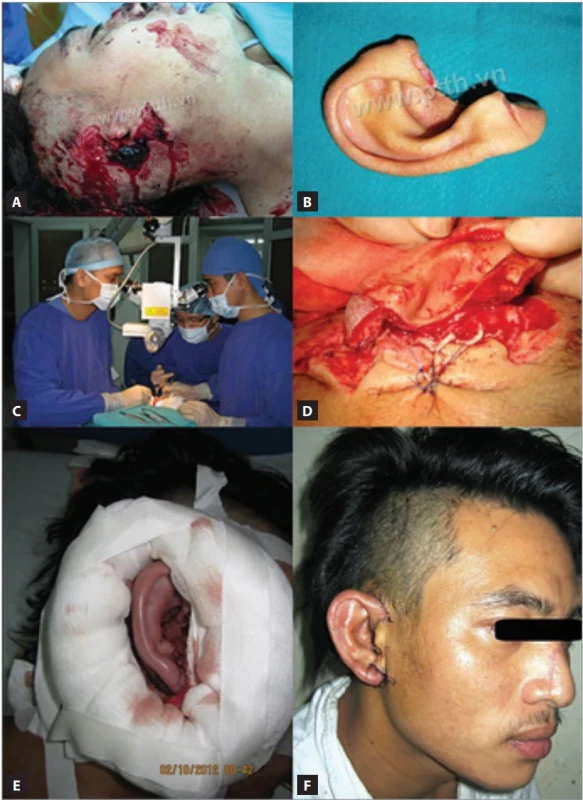
Results
There were four cases of microsurgical auricle replantation performed at Vietduc Hospital, Hanoi, Vietnam from February 2012 to July 2022.
Case 1
A 30-year-old male patient (Fig. 1) had his right ear completely amputated by the traction force incurred by someone else during a violent incident. The patient received first aid at the district hospital, and then he was transferred to our hospital along with the amputated ear 14 hours later.
Emergency microsurgery involved two teams. The first team dissected and marked the distal ends of blood vessels on the amputated ear. An artery was found in the middle of the ear and another artery branch at the apex of the ear (a branch of the posterior auricular artery). The veins were constricted and difficult to find, but there were also two veins in the middle and apex. We marked those vessels with Prolene 6/0.
Second team dissected and marked the artery or vein in the patient’s temporal region. A branch of the posterior auricular artery with a diameter of about 0.5 mm was selected.
The arterial anastomosis was performed using Ethilon 11/0. Arterial blood flow through the anastomosis was good, but there was no backflow from two found veins, only at the wound edge, probably because these veins were too small. We continued to dissect and found another vein in the earlobe area. We continued to dissect along this vein for a distance of 7–8 mm and then move diagonally upwards to anastomose with the vein in the middle of the ear, near the arterial anastomosis.
Total surgery time was about 7 hours. After surgery, the ear showed signs of mild hyperaemia, but there was no venous congestion, and this resolved within 7 days. Postoperative anticoagulation regimen was heparin 10,000 IU/day for 7 days then switched to aspirin 250 mg/day for 3 weeks. After 9 days, the ear color was normal and the patient was discharged from the hospital.
Case 2
A 21-year-old male patient, with a history of heavy smoking, was admitted to the hospital 1 hour after a traffic accident, when his motorbike crashed into a barrier, causing part of his right ear to be amputated. The amputated part of the ear was not properly preserved and was placed directly on ice. The patient was transferred to the operating room 4 hours after the accident. Preoperative examination: the amputated part included most of the upper helix and antihelix of the right ear, measuring about 2.5 × 4 cm. The amputated part was quite crushed overall (Fig. 2).
2. Amputated ear replantation. (A) Part of the right ear was amputated; (B) posterior auricular artery anastomosis; (C) use of leeches to treat venous congestion; (D) long-term results. 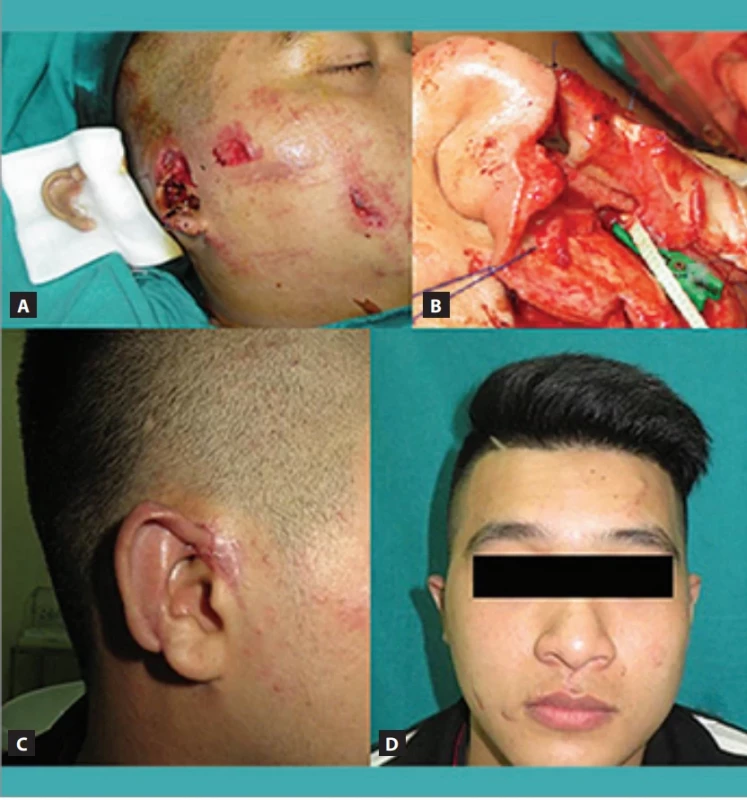
Under the microscope, an artery measuring about 0.4 mm was found but no vein (Fig. 2B). After performing an end-to-end anastomosis, venous reflux appeared at the wound edge, and a vein measuring about 0.3 mm was found right at the earlobe. At the corresponding location at the recipient site, we found a vein of similar size but severely bruised. We performed a microsurgical end-to-end venous anastomosis using interrupted Ethilon 10/0. The anastomosis was patent, the ear was warm and pink, and the capillary refill was in the normal range. The total surgery time was 8 hours. The patient was given systemic heparin during and after surgery. On the second day after surgery, venous congestion appeared. We had to use measures to reduce the congestion, such as aspiration of blood from the earlobe and wiping it with heparin-soaked gauze. On the third day, there was still congestion and edema, so we had to use leeches to drain venous blood. Measures to reduce venous congestion for 14 days were continued with anticoagulants to prevent embolism for 3 weeks. Blood loss was monitored. The total blood transfusion was 4 units. There was no infection and the replanted ear remained viable. Results were evaluated 1 year after surgery; cosmetic and anatomical recovery was achieved, and the patient was completely satisfied with the surgical results.
Discussion
There are many factors to consider when choosing a treatment for an amputated ear. These include: the mechanism of the injury, the size and condition of the ear (proximal stump and severed segment, the duration of ischemia, the age of the patient, and the patient’s general condition and consent. After careful consideration of these factors, the surgeon will decide on a treatment approach.
Three of our patients were injured in a traffic accident, and 1 patient was injured in a violent incident. According to Steffen’s literature review, the cause of auricular amputation is divided equally between traffic accidents and bite wounds (of which 65% are due to human bites, and 35% are due to dogs) [7]. In Vietnam as well as other developing countries, we find that the majority of the causes are due to traffic accidents and violent incidents, not due to bites like in Western countries. Therefore, our amputated parts are often large in size, occupying 2/3 of the ear or more, so the indication for microsurgical replantation is more necessary and reasonable than the indication for a composite graft [7,8]. Our ischemic time is 4–9 hours, while the optimal time for microsurgical replantation of amputated body parts is 6 hours. Histologically, the amputated ear is mainly composed of skin and cartilage tissue, perhaps for that reason the ischemic time may be longer than other body parts. The longest ischemic time for successful replantation was 33 hours [9]. However, we still feel it is necessary to organize training sessions for medical staff on how to preserve, transport and handle emergency cases of amputated body parts [3,10].
To date, in the literature, all authors agree that microsurgical auricular replantation is the priority, because it provides superior cosmetic results compared to non-microsurgical reconstruction [5,8,11–13].
In all of our patients, we found a branch of the posterior auricular artery measuring 0.4–0.5 mm, which is sufficient for anastomosis if the surgeon has good technique. We did not find any branch of the STA suitable for anastomosis. Which vascular pedicle to use to anastomose the amputated ear is also an important issue in the microsurgical anastomosis procedure. From our experience based on anatomical findings, we recommend prioritizing finding only 1–2 branches of the artery at the posterior site of the external ear. From our experience, one well patent artery branch is enough to supply blood to the entire amputated ear. It is better to spend time and effort to find and suture 1–2 more veins. Although, in the literature, more than 50% of reported cases of replanting auricular amputation were only able to anastomose 1 artery and no vein [5].
The position of the patient’s head also determines an important part of the success or failure of the whole surgery. To make anastomosis of the vessels behind the ear, some surgeons recommend a prone position [3,11]. However, we found that this position would be difficult for the surgical team because the microscope must always be tilted. Even the surgeon assistant would have difficulty during anastomosis phase. Therefore, we suggested that after exposing all the vessels that need to be anastomosed, we would anchor the cutaneous layer behind the ear with a few 6.0 nylon stitches, leaving the exposed cartilage separated. Place the patient in a supine position, slightly contralaterally tilted, so that the microsurgical lens can look straight down, which facilitates microsurgery (Fig. 1D, 2B). Throughout the literature, we found no recommendation in the choice of patient position, so there was no opportunity to draw experience from the standard procedure [4,5,7,8,11,12,14].
The indication and technique of microsurgical anastomosis will depend greatly on whether arterial and venous branches are found at both the peripheral and central ends. If no viable blood vessels could be found on the ear, microsurgical anastomosis would not be indicated. If both peripheral and central blood vessels were found but the crushed tissue limits viable vascular length, we will proceed with further dissection or grafting to avoid tension at the anastomosis. If the corresponding central artery cannot be identified, we will graft the peripheral artery with a branch of the posterior auricular artery. The authors recommend using only the posterior auricular artery in emergencies and reserving the STA for the superficial temporal fascia flap, as it may be necessary later for the secondary auricular reconstruction [5,7,8,15,16].
In some special cases, if there is no peripheral artery to anastomose, some authors have utilized the end of a peripheral vein as a blood supply. Then the replanted ear will become a venous flow-through flap (arterialization of the venous system) [17].
After the artery is anastomosed, the venous blood flowing back from the ear will help determine which vein is large enough to perform microsurgical anastomosis. If the vein is too small or cannot be anastomosed, some authors have used an arterial branch of the amputated ear, treating it as a draining vein, and anastomosing it to the recipient vein of the head and face through a reverse vein graft. This method allows some backflow, but the ear graft will swell for a long time after surgery [13].
A popular choice in cases of venous congestion is the use of medical or chemical leeches [18,19]. Out of our 4 patients, in two of them we could not suture the vein, so we had to use leeches to resolve the venous congestion. When medical leeches were not available, some authors suggested injecting high doses of heparin directly under the skin of the replanted ear, then making multiple small incisions on the ear and applying heparin-soaked gauze to drain the blood (chemical leeches). Currently, in the medical literature, there are about 20 cases of successful ear replantation without vein anastomosis [4,5]. However, the amount of blood loss is quite large and a blood transfusion of up to 7 units might be required [20]. In our two cases, venous congestion required leeches ranged from 10 to 14 days, with a total of 3–4 units of blood transfused. The advantages and risks of this technique needed to be discussed between the patient/patient’s family and the surgeon.
In addition to allowing venous backflow, leeches will release anticoagulants (hirudin) that cause increased bleeding. A major difficulty in Vietnam is that we do not have facilities to raise and supply medical leeches, so we had to encourage our family members to find and catch them in rural rivers and lakes in the wild. In the future, medicinal leaches fed with sterile bovine blood might be the solution. We also organized training for a group of professional nurses to store and preserve leeches for long-term use as well as to monitor them closely so that they do not move into the ear canal, nasal cavity, or mouth. To prevent the risk of Aeromonas hydrophila infection when using leeches, we always prescribe post-operative antibiotic treatment (usually quinolone or third generation cephalosporin).
Although the number of clinical cases is small, all authors agree that microsurgical replantation provides the best aesthetic results. When replantation is not possible due to contraindications or microsurgical replantation fails, patients will undergo secondary auricular reconstruction. Since most of the patients with traumatic ear loss were adults, whose costal cartilage is completely ossified, many authors choose the method of one-stage ear reconstruction using an artificial cartilage framework (Fig. 3). That is why it is very important to preserve the STA with all its branches in cases of traumatic ear loss to be used in secondary auricular reconstruction [16,21,22].
3. Single-stage traumatic ear reconstruction with artifi cial framework. (A) 39-year-old male patient, post-traumatic ear amputation; (B) CT angiography shows superfi cial temporal arteries still preserved during the emergency stage; (C) harvest the temporoparietal fascia fl ap with an endoscopic technique with full branch frontal and parietal; (D) immediate reconstructed ear post-operative result, no scar on the scalp; (E,F) 6 months post-operative result. 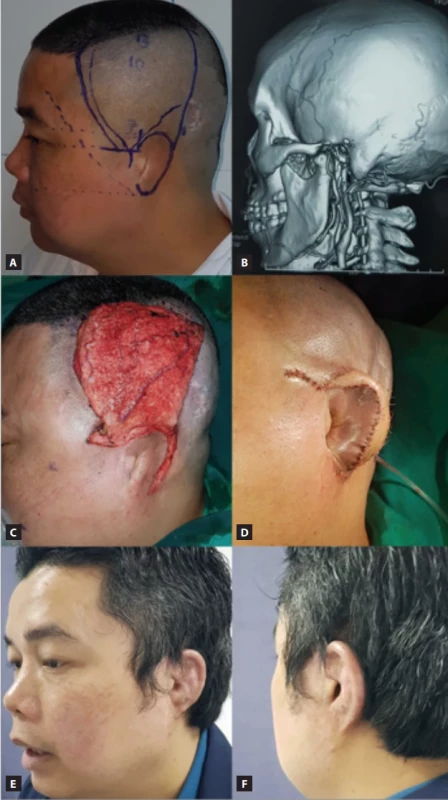
Conclusion
An amputated ear is a rare emergency injury and each case is different. The surgeon will have to apply the appropriate treatment techniques. If possible, microsurgical auricular replantation is the optimal choice because it provides excellent cosmetic results. If this is not the case, second-stage auricular reconstruction, especially the endoscopically assisted technique using an artificial frame, provides convenience and excellent cosmetic results. We recommend not damaging the skin of the mastoid region and the branches of the STA so that there is material for secondary reconstruction.
Disclosure
The authors have no conflicts of interest to disclose. The authors declare that this study has received no financial support. All procedures performed in this study involving human participants were in accordance with ethical standards of the institutional and/or national research committee and with the Helsinki declaration and its later amendments or comparable ethical standards.
Roles of authors
Nguyen Hong Ha – conception and design, data acquisition, analysis and interpretation of data, writing publication, critical revision of publication, supervision, resources; Tran Thi Thanh Huyen – analysis and interpretation of data, writing publication, critical revision of publication, technical, administrative, or material support.
Sources
1. Buncke HJ., Schulz WP. Total ear reimplantation in the rabbit utilising microminiature vascular anastomoses. Br J Plast Surg. 1966, 19 (1): 15–22.
2. Pennington DG., Lai MF., Pelly AD. Successful replantation of a completely avulsed ear by microvascular anastomosis. Plast Reconstr Surg. 1980, 65 (6): 820–823.
3. Jung SW., Lee J., Oh SJ. et al. A review of microvascular ear replantation. J Reconstr Microsurg. 2013, 29 (3): 181–188.
4. Momeni A., Liu X, Januszyk M., et al. Microsurgical ear replantation-is venous repair necessary? A systematic review. Microsurgery. 2016, 36 (4): 345–350.
5. Gailey AD., Farquhar D., Clark JM., et al., Auricular avulsion injuries and reattachment techniques: a systematic review. Laryngoscope Investig Otolaryngol. 2020, 5 (3): 381–389.
6. van Gijn DR., Dunne J. Oxford handbook of head and neck anatomy. Oxford University Press 2022.
7. Steffen A., Katzbach R., Klaiber S. A comparison of ear reattachment methods: a review of 25 years since Pennington. Plast Reconstr Surg. 2006, 118 (6): 1358–1364.
8. Baldini N. A comparison of ear amputations replantation techniques. J Stomatol Oral Maxillofac Surg. 2024, 125 (Suppl 2): 101497.
9. Shelley OP., Villafane O., Watson SB. Successful partial ear replantation after prolonged ischaemia time. Br J Plast Surg. 2000, 53 (1): 76–77.
10. Nguyen HH. The microsurgical replantation of seven complete scalp avulsions: is one artery sufficient? J Plast Reconstr Aesthet Surg. 2012, 65 (12): 1639–1644.
11. Bai H., Tollefson TT. Treatment strategies for auricular avulsions: best practice. JAMA Facial Plast Surg. 2014, 16 (1): 7–8.
12. Dadaci M., Yildirim MEC., Ince B. Experience of replantation and reconstruction in total scalp, partial forehead, and ear avulsions. J Craniofac Surg. 2019, 30 (7): 2268–2270.
13. Pederson WC. Replantation. Plast Reconstr Surg. 2001, 107 (3): 823–841.
14. Shubin H., Jun W., Yunyong H., et al. Replantation of amputated ear with anastomosis of vessel. Zhonghua Zheng Xing Wai Ke Za Zhi. 2015, 31 (5): 337–339.
15. Reinisch JF., van Hövel Tot Westerflier CVA., Gould DJ., et al. Secondary salvage of the unsatisfactory microtia reconstruction. Plast Reconstr Surg. 2020, 145 (5): 1252–1261.
16. Nguyen H., Huyen TTT., Hang NTT. Single-incision endoscopic-assisted temporoparietal fascia harvest for single stage auricular reconstruction. Acta Chir Plast. 2022, 64 (2): 62–68.
17. Trovato MJ., Agarwal JP. Successful replantation of the ear as a venous flap. Ann Plast Surg. 2008, 61 (2): 164–168.
18. Chepeha DB., Nussenbaum B., Bradford CR. et al. Leech therapy for patients with surgically unsalvageable venous obstruction after revascularized free tissue transfer. Arch Otolaryngol Head Neck Surg. 2002, 128 (8): 960–965.
19. Alfeky H., McArthur P., Helmy Y. Salvaging digital replantation and revascularisation: efficiency of heparin solution subcutaneous injection. Surg Res Pract. 2018, 2018 : 1601738.
20. Nath RK., Kraemer BA., Azizzadeh A. Complete ear replantation without venous anastomosis. Microsurgery. 1998, 18 (4): 282–285.
21. Baluch N., Nagata S., Park C., et al. Auricular reconstruction for microtia: a review of available methods. Plast Surg (Oakv). 2014, 22 (1): 39–43.
22. Nguyen HH., Vu DD., Ngo LM., et al. Anatomical variant of the superficial temporal artery in temporoparietal fascia flap for microtia reconstruction. J Plast Reconstr Aesthet Surg. 2024, 91 : 105–110.
Nguyen Hong Ha
Department of Maxillofacial – Plastic – Aesthetic Surgery
Viet-Duc University Hospital
40 Trang Thi, Hanoi, Vietnam
nhadr4@gmail.com
Submitted: 9. 3. 2025
Accepted: 8. 12. 2025
Labels
Plastic surgery Orthopaedics Burns medicine Traumatology
Article was published inActa chirurgiae plasticae

2025 Issue 4-
All articles in this issue
- Will robots replace us?
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
- Intraoperative cone beam computed tomography in craniomaxillofacial traumatology – a case report
- Digital retractile keloid in a context of spontaneous keloids – a case report
- Extensive keloid scar of the left auricle – combined treatment of excision followed by brachytherapy: a case report
- Post-otoplasty keloid scars – treatment strategies and case reports
- Large urethral false passage during a routine catheterization – low threshold for better outcome
- Acta chirurgiae plasticae
- Journal archive
- Current issue
- Online only
- About the journal
Most read in this issue- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career

