-
Medical journals
- Career
Digital retractile keloid in a context of spontaneous keloids – a case report
Authors: G. Belmaati Cherkaoui 1; M. Tajir 2; A. Daoudi 3; A. A. Oufkir 1
Authors‘ workplace: Department of Plastic and Reconstructive surgery, Mohammed VI Hospital University, and Research Laboratory in Medical Sciences, Faculty of Medicine and Pharmacy of Oujda, Mohammed I University, Oujda, Morocco 1; Department of Genetics, Mohamed IV Hospital University, Oujda, Morocco 2; Department of Traumatology, Mohamed IV Hospital University, Oujda, Morocco 3
Published in: ACTA CHIRURGIAE PLASTICAE, 67, 4, 2025, pp. 260-263
doi: https://doi.org/10.48095/ccachp2025260Introduction
The term spontaneous keloids, which defines keloid disease, refers to an extremely rare phenomenon in which keloid lesions develop without any identifiable triggering factor such as trauma or surgery. Clinically and pathophysiologically, they are identical to secondary keloids [1], although their existence is debated by some authors [2,3]. It is generally accepted that these lesions are triggered by microtrauma or minimal skin inflammation in genetically predisposed individuals. They have also been reported in association with several genetic syndromes, including Bethlem myopathy, Rubinstein–Taybi syndrome, Dubowitz syndrome, Noonan syndrome, Goeminne syndrome, X-linked recessive polyfibromatosis, and FLNA mutation–related syndrome [4].
Palmoplantar involvement is exceptional and can lead to significant functional impairment, with a substantial impact on quality of life [5]. Treatment remains a major challenge for plastic surgeons because of frequent and unpredictable recurrences. We report here a case of palmoplantar retractile keloid occurring in the context of spontaneous keloids.
Case description
A 32-year-old woman, a secondary school teacher, born from a first-degree consanguineous marriage and with a history of glaucoma treated for the past three years, presented for management of a post-traumatic left IV–V syndactyly (wound sutured 12 years earlier) associated with a complete flexion contracture. The left hallux was also retracted and fixed to the sole, resulting in major functional impairment. Since childhood, the patient had developed hypertrophic scars extending beyond the wound margins after minor trauma or even spontaneously, for which a biopsy had confirmed keloid scars. Clinical examination revealed partial scarring syndactyly of the fourth and fifth digits of the left hand was noted. A keloid mass filled the fourth web space and extended to the pulp of the little finger. The keloid largely involved both the ulnar and radial margins of the fourth and fifth fingers, resulting in stage IV digital retraction of the little finger and stage III of the ring finger according to Tubiana’s classification (Fig. 1A).
A keloid-related retraction of the hallux was also observed, fixed in plantar flexion at approximately 100° (Fig. 1B).
1. Keloid on the palmar surface of the left hand causing digital retraction (A); plantar keloid causing fl exion of the hallux (B). 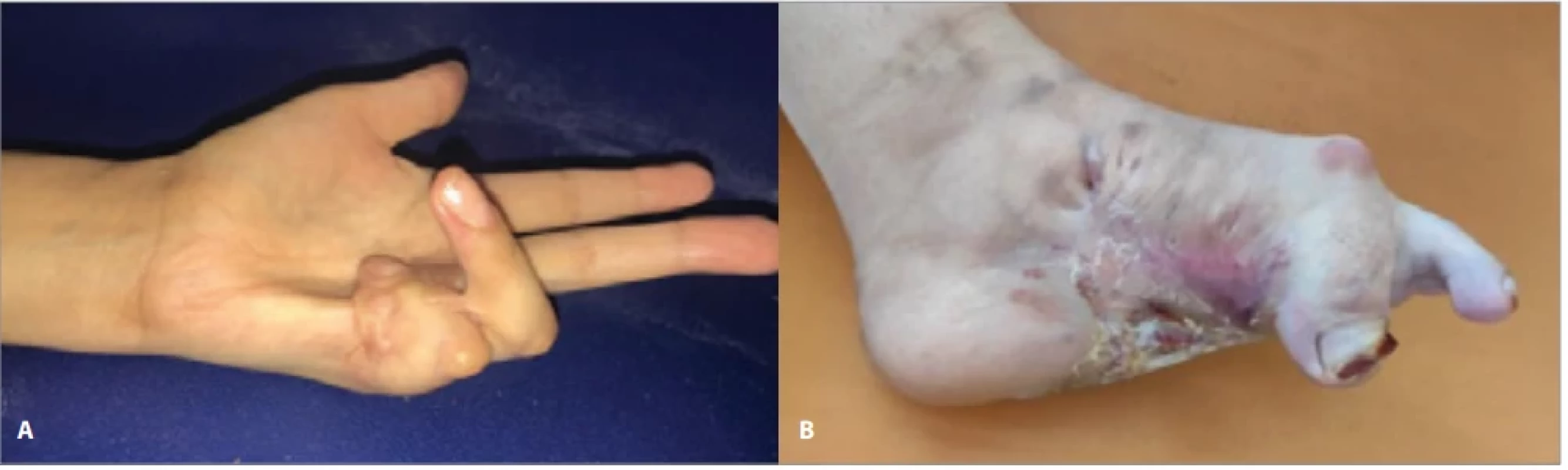
The remainder of the examination revealed keloid scars of various sizes scattered over the body, predominantly on the lower limbs (Fig. 2). Additional findings included facial dysmorphia characterized by ptosis, right-sided exophthalmos, dental malposition, and gingival hypertrophy, as well as dorsal kyphosis. The patient’s general condition was good, with no associated visceral malformations.
2. Keloidal scars of varying size scattered over the body. 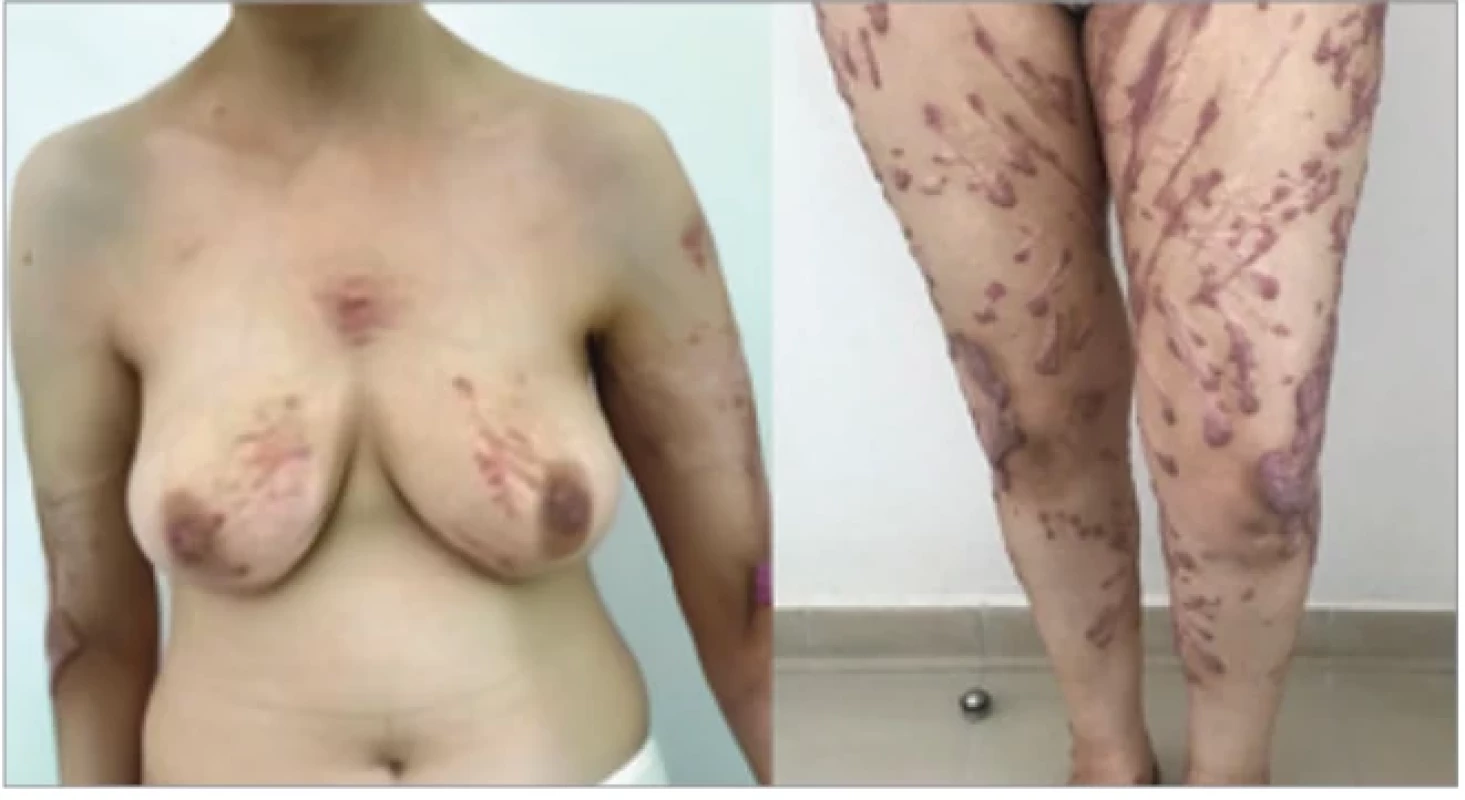
Due to limitations in available molecular diagnostic resources, we were unable to identify the underlying genetic syndrome. The patient’s genetic material was therefore sent to a specialized reference center, where no pathogenic variant was detected on exome sequencing.
The treatment combined the release of the retractile keloid plaque, easy manual arthrolysis to restore full extension (as there was neither joint stiffness nor tendon retraction), immediate coverage of the defect with a thin split-thickness skin graft, and immobilization with Kirschner wires fixing the metacarpophalangeal joints at 90° flexion and the proximal interphalangeal joints in neutral extension.
At the level of the sole, arthrodesis of the hallux metatarsophalangeal joint was performed after release and excision of the keloid plaque. The defect was covered using a transposition flap combined with a thin split-thickness skin graft (Fig. 3). Histopathological examination of the surgical specimen confirmed the keloid nature of the lesions.
3. Plantar keloid release with hallux arthrodesis. 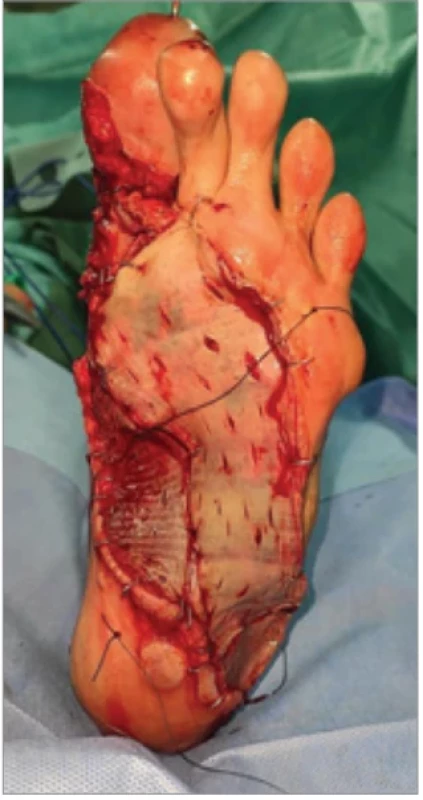
One year after surgery, digital retraction recurred with keloid formation at the edges of the skin graft (stage III of Tubiana for both fingers). At the level of the sole, there was neither keloid recurrence nor retraction. Intralesional corticosteroid injections (betamethasone) administered every 3 weeks for a total of 6 sessions, was attempted in the hand, with poor clinical improvement (Fig. 4). Postoperative outcomes for the foot remained satisfactory (Fig. 5).
At a two-year follow-up, no retraction or keloid recurrence was observed, including on the plantar surface of the foot
4. Immediate and late postoperative result (6 months after surgery). 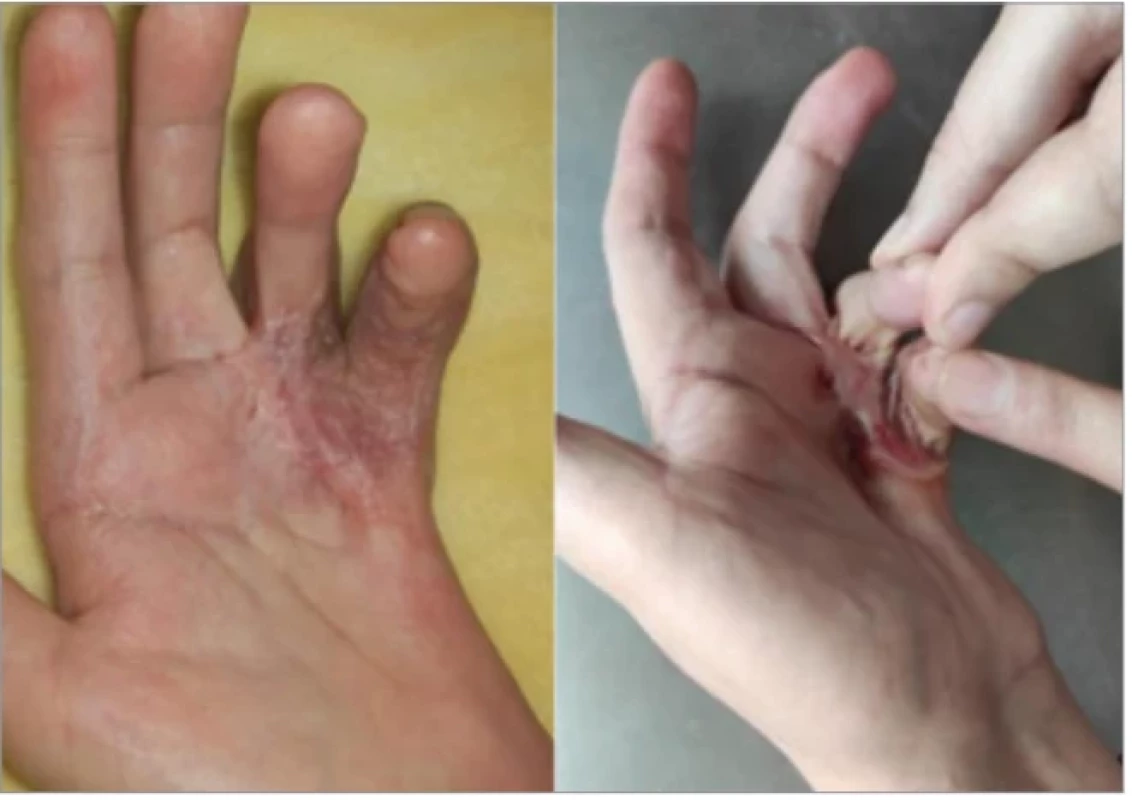
5. Late postoperative result (2 months after surgery). 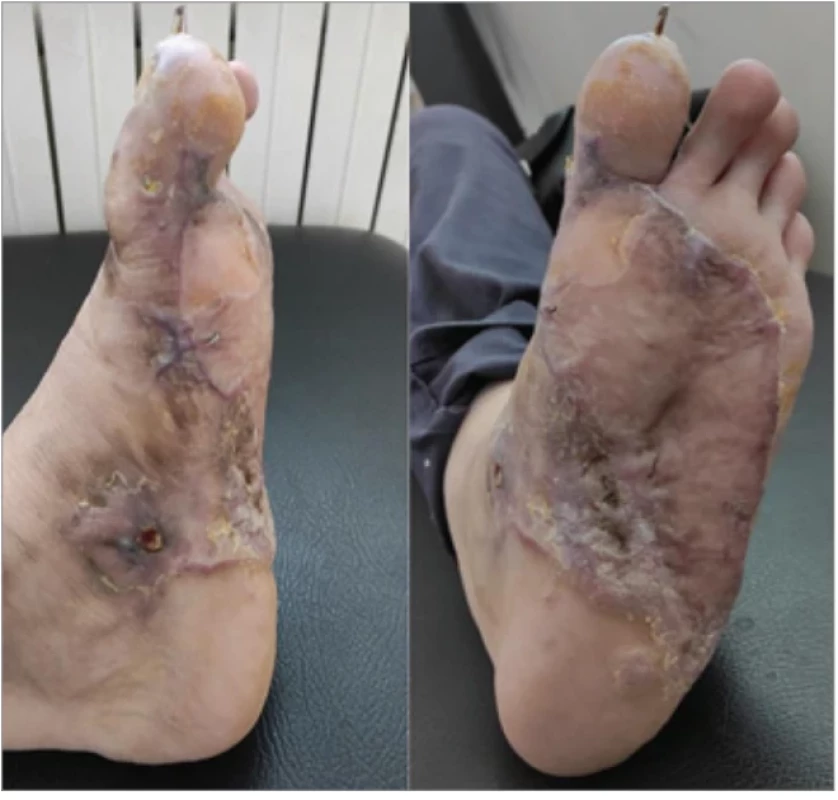
Discussion
Spontaneous keloids are rare lesions, developed without skin trauma [6], reported mainly in association with several genetic syndromes. They are located preferentially on the chest, shoulders and upper back, as secondary keloids [1,7].
Palmar localization of secondary keloids is rare but often disabling. Small series have been described in the Anglo--Saxon literature [8]. In our patient, the keloid was located on the palmar surface of the fourth and fifth fingers, resulting in a partial IV–V scar syndactyly.
In all genetic syndromes associated with spontaneous keloids, hand involvement has not been reported. In polyfibromatosis syndrome, palmar (Dupuytren’s disease), plantar (Ledderhose disease), and penile (Peyronie’s disease) fibromatoses are associated with an erosive arthropathy, but without keloid formation. X-linked recessive polyfibromatosis is known to combine spontaneous keloid scarring with Dupuytren’s contracture [9].
The specific features of this case include:
- the unusual palmar localization of the keloids;
- the rapid progression of the lesions;
- the absence of identifiable genetic abnormalities despite the association of spontaneous keloids with facial dysmorphy;
- the preservation of soft-tissue and joint mobility beneath the hand keloids;
- the rapid recurrence and therapeutic challenges.
- In addition to the sometimes-debilitating aesthetic and psychological impact of this pathology [10], functional impairment is particularly significant at the palmar level, often necessitating surgical intervention.
The curative management of keloids remains disappointing. There is no consensus, and all therapeutic protocols have shown limited success, with persistently high recurrence rates – an issue that explains the wide variety of treatments currently employed. Surgery alone is associated with recurrence rates ranging from 45% to 100% [10].
Combination therapies including surgery aim to reduce these rates. Some authors [11] have advocated triple therapy – combining surgery, intralesional corticosteroid injections, and radiotherapy – with encouraging outcomes. The most effective preventive approach to date is pressure therapy using silicone gel sheeting, which has been reported to reduce recurrence in up to 80% of cases [10].
In this case, surgery combined with intensive physiotherapy and corticosteroid infiltration resulted only in transient improvement in the hand, and the functional benefit of this combination therapy remained limited. In contrast, at the level of the sole, no recurrence of either the retraction – prevented by the metatarsophalangeal arthrodesis – or the keloid was observed.
Conclusion
Digital retractile keloid occurring in the context of spontaneous keloids represents an extremely rare association that, to our knowledge, has not been previously reported in the literature. Its pathophysiology is likely not substantially different from that of secondary keloids. Further investigation into the underlying molecular mechanisms is needed to support the development of more effective therapeutic strategies.
Roles of the authors
G. Belmaati Cherkaoui – clinical management of the patient, drafting of the manuscript; M. Tajir – clinical management of the patient, A. Daoudi – clinical management of the patient, A. A. Oufkir – supervision, critical revision, final approval of the manuscript
Declaration of interest
The authors declare that they have no conflicts of interest in relation to this article.
Consent statement
Written informed consent was obtained from the patient.
Funding acknowledgement
This research received no specific grant from any funding agency in the public
Ethics
The ethical authorization has not been requested because it is a case report and the consent of the patient concerned is made.
Sources
1. Pitche P. What is true in „spontaneous“ keloids? Ann Dermatol Venereol. 2006, 133 (Pt 1): 501.
2. McCabe J., Blades Z., McGrath EE. A spontaneous skin lesion. CMAJ. 2008, 179 (12): 1297–1299.
3. Mandal A., Imran D., Rao GS. Spontaneous keloids in siblings. Ir Med J. 2004, 97 (8): 250–251.
4. Abdulhadi Jfri., Alajmi A. Spontaneous keloids: a literature review. Dermatology. 2018, 234 (3–4): 127–130.
5. Bock O., Schmid-Ott G., Malewski P., et al. Quality of life of patients with keloid and hypertrophic scarring. Arch Dermatol Res. 2006, 297 (10): 433–438.
6. Kerfant N., Gasnier P., Boloorchi A., et al. Spontaneous keloids: about a rare case. Ann Chir Plast Esthet. 2011, 56 (4): 339–341.
7. van de Kar AL., Houge G., Shaw AC., et al. Keloids in Rubinstein-Taybi syndrome: a clinical study. Br J Dermatol. 2014; 171 (3): 615–621.
8. Britto JA., Elliot D. Aggressive keloid scarring of the Caucasian wrist and palm. Br J Plast Surg. 2001, 54 (5): 461–462.
9. Ly L., Winship I. X-linked recessive polyfibromatosis manifesting with spontaneous keloid scars and Dupuytren’s contracture. Australas J Dermatol. 2012, 53 (2): 148–150.
10. Chike-Obi CJ., Cole PD., Brissett AE. Keloids: pathogenesis, clinical features, and management. Semin Plast Surg. 2009, 23 (3): 178–184.
11. Osswald SS., Elston DM., Vogel PS. Giant right plantar keloid treated with excision and tissue engineered allograft. J Am Acad Dermatol. 2003, 48 (1): 131–134.
Ghita Belmaati Cherkaoui
Department of Plastic and Reconstructive surgery
Mohammed VI Hospital University
Oujda
Morocco
ghita.cherkaouibelmaati@gmail.com
Submitted: 23. 4. 2025
Accepted: 22. 11. 2025
Labels
Plastic surgery Orthopaedics Burns medicine Traumatology
Article was published inActa chirurgiae plasticae

2025 Issue 4-
All articles in this issue
- Will robots replace us?
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
- Intraoperative cone beam computed tomography in craniomaxillofacial traumatology – a case report
- Digital retractile keloid in a context of spontaneous keloids – a case report
- Extensive keloid scar of the left auricle – combined treatment of excision followed by brachytherapy: a case report
- Post-otoplasty keloid scars – treatment strategies and case reports
- Large urethral false passage during a routine catheterization – low threshold for better outcome
- Acta chirurgiae plasticae
- Journal archive
- Current issue
- Online only
- About the journal
Most read in this issue- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career

