-
Medical journals
- Career
Post-otoplasty keloid scars – treatment strategies and case reports
Authors: J. Stehlík 1; L. Streit 1,2; O. Košková 1,2
Authors‘ workplace: Department of Burns and Plastic Surgery, University Hospital Brno, Czech Republic 1; Faculty of Medicine, Masaryk University Brno, Czech Republic 2
Published in: ACTA CHIRURGIAE PLASTICAE, 67, 4, 2025, pp. 268-272
doi: https://doi.org/10.48095/ccachp2025268Introduction
Wound healing is a complex physiological process culminating in scar formation, which restores tissue integrity but may lead to pathological outcomes such as hypertrophic scars or keloids. Keloids are benign fibroproliferative lesions characterized by excessive collagen deposition, extending beyond the original wound margins [1]. Unlike hypertrophic scars, keloids do not regress spontaneously and often enlarge over time, causing aesthetic, functional, and psychosocial issues [2]. Clinically, keloids present as firm, raised, glossy lesions, frequently accompanied by pruritus, pain, or pressure sensations [3].
Keloids have a reported prevalence of 4–16% in the general population, with higher rates (up to 20%) in individuals with darker skin phototypes (Fitzpatrick IV–VI), particularly those of African, Caribbean, South Asian, or Hispanic descent [4]. Genetic predisposition plays a significant role, with familial clustering suggesting autosomal dominant inheritance with incomplete penetrance [5]. Identified genetic markers, such as those on chromosomes 2q23 and 7p11, further support this predisposition [6]. Keloids are most common between ages 11 and 30, when skin healing is most active, with a slight female predominance [7].
Auricular keloids, particularly those following otoplasty, represent a distinct clinical subset due to their anatomical location and therapeutic challenges [8]. Otoplasty, a procedure to correct prominent ears, is often performed in younger patients, a group already at higher risk for keloid formation due to active wound healing. Auricular keloids in this region are particularly prone to recurrence due to mechanical tension and anatomical constraints. A study by Mohammadi et al. demonstrated that surgical excision followed by postoperative intralesional triamcinolone acetonide injections achieved a 100% success rate without recurrence over a mean follow-up of 16 months, suggesting this combined approach as an effective treatment protocol for auricular keloids [9]. The posterior auricle, a common site for keloid development post-otoplasty, is poorly ventilated and subject to mechanical tension, exacerbating fibrotic responses [1]. Additional risk factors include darker skin phototypes, genetic predisposition, and a history of keloid formation [4]. These keloids frequently recur after treatment, necessitating repeated interventions and causing significant aesthetic and psychological distress [7]. While not separately classified in ICD-10 or ICD-11, auricular keloids require specialized management strategies to address their unique characteristics [8].
Case reports
Patient 1
A 14-year-old male patient, with a light skin phototype (Fitzpatrick II) and no family history of keloids, underwent bilateral otoplasty in 2017 at another institution to correct prominent ears. In 2019, he developed keloids on the posterior auricle, which were surgically excised. Recurrence occurred in 2022, likely due to non-compliance with the recommended postoperative treatment protocol after the initial excision and necessitated further surgical intervention. Postoperatively, our institutional protocol was implemented, consisting daily silicone gel and patch application, pressure massages, low-level laser therapy (LLLT) – 15–20 sessions, 3 times weekly) – and at the first signs of hypertrophic scar maturation, triamcinolone acetonide ointment was introduced (applied daily at night for one month, with therapy repeated after a three-week interval). One year post-surgery, the patient exhibited improved scar remodeling with no further recurrence, although long-term monitoring remains ongoing (Fig. 1).
1. Patient 1 – extensive keloid formation preoperatively (left) and a maturing scar one year post-surgery with strict adherence to the treatment protocol (right). 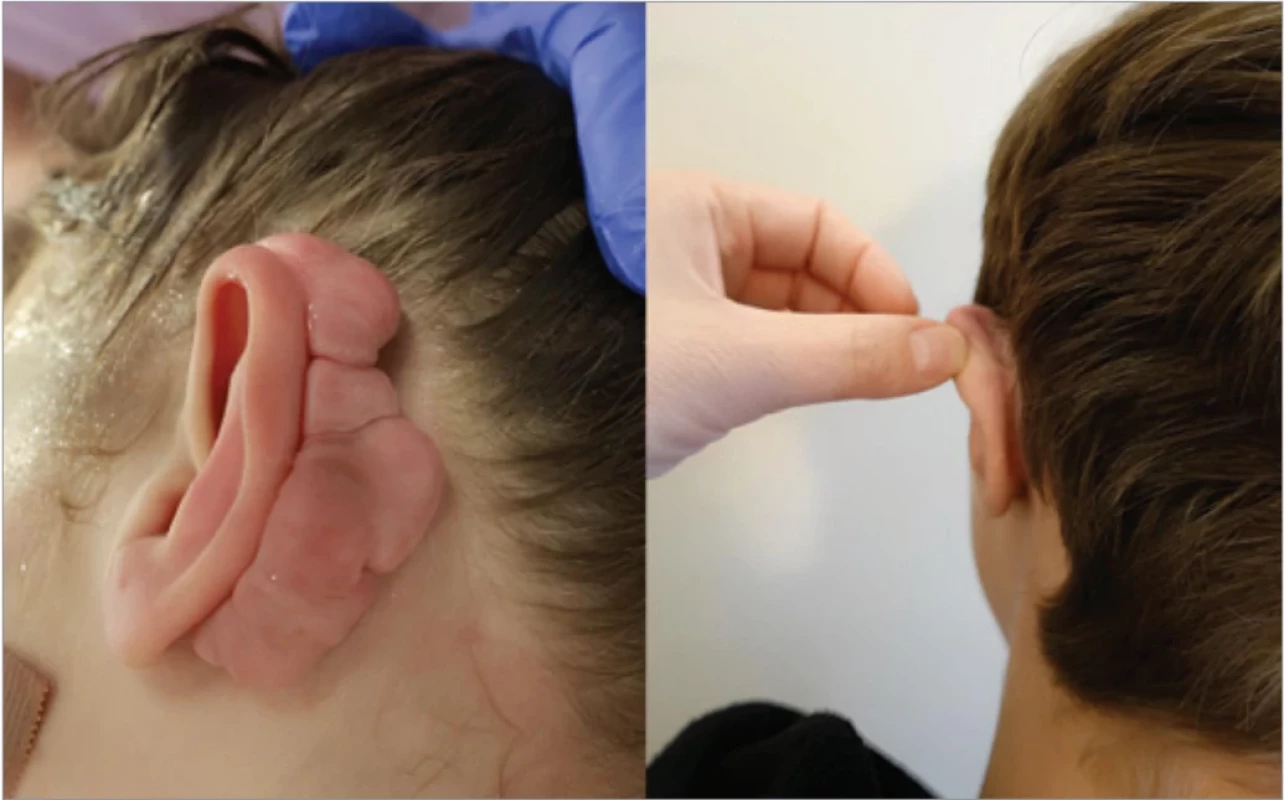
Patient 2
A 13-year-old male patient, with a light skin phototype (Fitzpatrick II) and no family history of keloids, underwent otoplasty in 2020 at another institution. Keloid formation was noted in 2022, leading to surgical excision. In 2024, recurrent keloids required another excision (Fig. 2), likely due to limited access to follow-up care and adjuvant therapies during the COVID-19 pandemic. Post-excision management followed our institutional protocol: daily application of silicone gel and patches, pressure massages, and LLLT – 15–20 sessions, three times weekly. At the first signs of hypertrophic scar maturation, triamcinolone acetonide ointment was introduced (applied nightly for 1 month). Three months after surgery, keloid scar maturation began to be observed; therefore, intralesional injections of methylprednisolone acetate were administered (every 3 weeks, for a total of 4 sessions). One year postoperatively, no signs of keloid recurrence were observed. The patient exhibited no scar hypertrophy and improved aesthetic outcomes, with ongoing follow-up to monitor for any recurrence (Fig. 3).
2. Patient 2 – preoperative keloid formation observed on both ears. 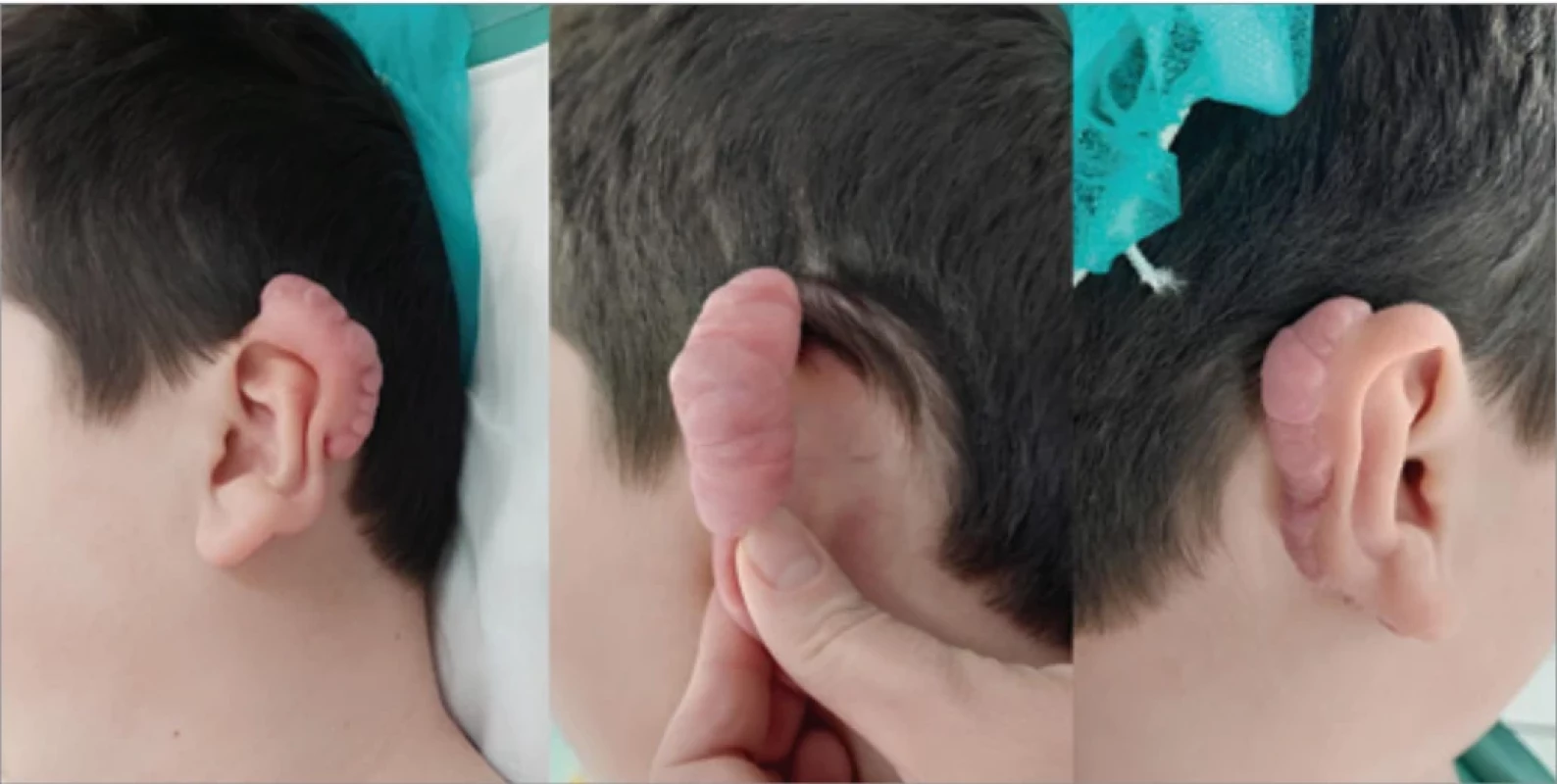
3. Patient 2 –outcome of scar maturation one year following keloid excision with consistent adherence to the treatment protocol (repeated intralesional corticosteroid administration, low-level laser therapy, regular application of silicone products, and pressure massage). 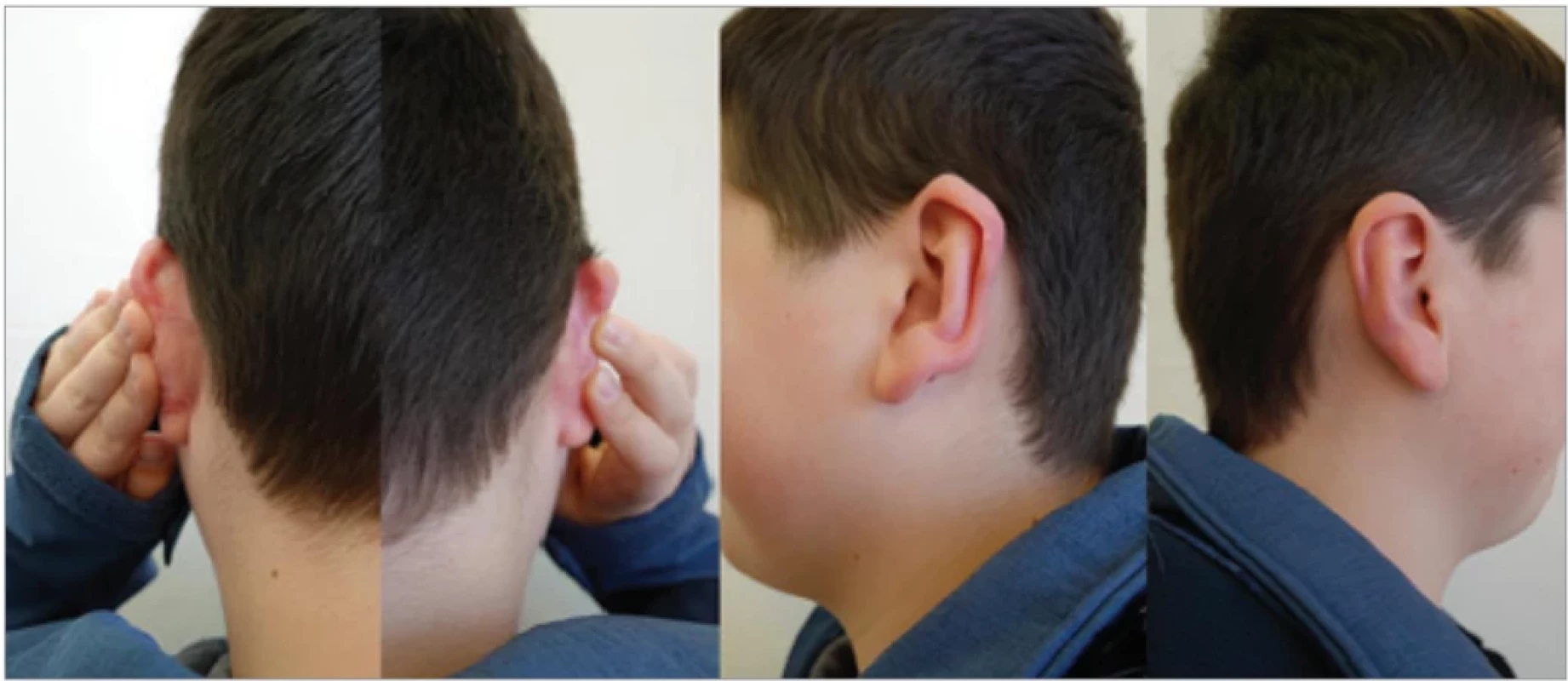
Discussion
The management of auricular keloids post-otoplasty remains challenging due to their high recurrence rate (up to 80% after surgical excision alone) and the aesthetic significance of the ear [1]. No universal treatment protocol exists, but evidence supports a multimodal approach combining surgical and non-surgical modalities to minimize recurrence and optimize outcomes [2]. Silicone-based therapy, LLLT and pressure massages are a cornerstone of prevention and therapy of hypertrophic and keloid scars [10,11]. Compression therapy, especially when combined with silicone sheets, has also demonstrated reduced recurrence rates following keloid excision [12]. Silicone-based therapies (gels and patches) create a hydrated, occlusive environment that softens scars and reduces tension [10]. The LLLT (e. g., 805 nm LED devices used several times weekly) has shown promise in scar modulation, particularly in early hypertrophic and keloid scars, while pressure massages improve scar pliability [3,11]. At the first signs of scar hypertrophy or keloid formation, topical or intralesional corticosteroid administration such as methylprednisolone acetate plays an important therapeutic role by reducing collagen synthesis and fibroblast proliferation [13]. The choice of steroid type, dosage, and injection technique remains variable in clinical practice, but international expert consensus highlights the need for standardized protocols for intralesional corticosteroid treatment of keloids [14]. The synergistic effect of triamcinolone acetonide and 5-fluorouracil in pathological scars is also well-documented, and physical enhancement techniques such as microneedling or microincision significantly improve their dermal penetration [15]. Advanced laser modalities, including pulsed dye laser (PDL) and fractional CO₂ laser, can improve texture, reduce erythema, and lead to partial volume reduction in keloid and hypertrophic scars. Clinical studies show that PDL in particular offers promising outcomes with minimal side effects. For established keloids, laser therapy (CO2 or PDL) is integrated with corticosteroids to enhance efficacy, with recent systematic reviews showing that CO₂ laser-assisted delivery of triamcinolone acetonide improves outcomes in scar texture, pigmentation, and volume reduction compared to monotherapy [16,17].
Adjunctive treatments such as radiotherapy and intralesional cytostatic agents have also been explored for keloid management. Postoperative superficial radiotherapy, particularly electron beam or brachytherapy, may reduce recurrence rates when administered within 24–72 hours after surgical excision, by suppressing fibroblast proliferation and extracellular matrix deposition. This approach is primarily used in adult patients and typically reserved for extensive or refractory keloid formations, given the potential risks and limited data on its safety and efficacy in pediatric populations [18]. Similarly, intralesional 5-fluorouracil (5-FU), either alone or in combination with corticosteroids, has shown promising results in reducing keloid size and symptoms by interfering with DNA synthesis in rapidly dividing cells. This treatment is primarily used in adult patients, particularly for extensive hypertrophic or keloid scars, where conventional therapies have limited efficacy [19]. These modalities are generally reserved for refractory or recurrent cases due to potential side effects. Future research should focus on optimizing laser therapy parameters and exploring novel adjuvants, such as 5-fluorouracil, to further reduce recurrence rates [2]. Genetic profiling may also guide personalized prevention strategies, enhancing outcomes in predisposed individuals [6].
At our institution, we emphasize early intervention to prevent keloid progression, particularly in high-risk patients (e. g., younger age, darker phototypes, or positive family history) [4]. Our protocol, illustrated in Scheme 1 and implemented at our institution since 2022, is initiated immediately after wound healing and is tailored to the stage of keloid development. As part of the surgical protocol for the treatment of recurrent keloids, the authors recommend using only non-absorbable suture material, which is removed at the end of the second postoperative week. A key element of the surgical technique is the careful mobilization of the wound edges to achieve a tension-free closure, thereby minimizing mechanical stress on the scar and reducing the risk of recurrence. According to the authors’ clinical experience, early initiation of the protocol using LLLT and topical corticosteroid ointments at the first signs of hypertrophic scar formation in at-risk teenage patients helps reduce the progression to potential keloid development. In contrast, in patients with a known history of keloids in this high-risk age group, it is advisable to initiate intralesional corticosteroid injections at the earliest signs of hypertrophic scarring. None of the presented patients experienced any side effects related to the non-systemic administration of corticosteroids.
This approach has shown promising results in reducing recurrence and improving aesthetic outcomes, as demonstrated in the presented cases. The presented cases highlight the efficacy of a structured, multimodal approach in managing auricular keloids post-otoplasty. Early intervention, particularly in high-risk patients, is critical to prevent progression to fully developed keloids [4].
Scheme 1. Keloid scar treatment protocol at our institution. 
LLLT – low-level laser therapy Conclusion
Although rare, keloid formation following otoplasty must be considered a potential complication, particularly in predisposed individuals. Early recognition and intervention are essential, with treatment ideally initiated during the early stages of scar maturation. In cases where the keloid causes auricular deformity, surgical excision is indicated. However, surgical excision alone carries a high risk of recurrence. Based on our clinical experience, the implementation of a strict multimodal postoperative protocol including silicone therapy, pressure massage, low-level laser therapy, and topical or intralesional corticosteroids significantly reduces the likelihood of recurrence and improves both functional and aesthetic outcomes.
Roles of the authors: Jan Stehlík contributed to the conceptualization of the study, data curation, writing of the original draft, and review and editing of the manuscript. Libor Streit was involved in writing the original draft. Olga Košková participated in the conceptualization of the study, data curation, project administration, writing of the original draft, and review and editing of the manuscript.
Disclosure: The authors have no conflicts of interest to disclose. The study was in accordance with the Helsinki declaration. The legal guardians of the patients provided informed consent for publication.
Funding: This research was supported by Specific University Research provided by MŠMT MUNI/A/1822/2025 and supported by MH CZ – DRO (FNBr, 65269705).
Sources
1. Ogawa R. Keloid and hypertrophic scars are the result of chronic inflammation in the reticular dermis. Int J Mol Sci. 2017, 18 (3): 606.
2. Berman B., Maderal A., Raphael B. Keloids and hypertrophic scars: pathophysiology, classification, and treatment. Dermatol Surg. 2017, 43 (Suppl 1): S3–S18.
3. Andrews JP., Marttala J., Macarak E., et al. Keloids: the paradigm of skin fibrosis – pathomechanisms and treatment. Matrix Biol. 2016, 51 : 37–46.
4. Bayat A., Arscott G., Ollier WE., et al. Keloid disease: clinical relevance of single versus multiple site scars. Br J Plast Surg. 2005, 58 (1): 28–37.
5. Marneros AG., Norris JE., Olsen BR., et al. Clinical genetics of familial keloids. Arch Dermatol. 2001, 137 (11): 1429–1434.
6. Nakashima M., Chung S., Takahashi A., et al. A genome-wide association study identifies four susceptibility loci for keloid in the Japanese population. Nat Genet. 2010, 42 (9): 768–771.
7. Chike-Obi CJ., Cole PD., Brissett AE. Keloids: pathogenesis, clinical features, and management. Semin Plast Surg. 2009, 23 (3): 178–184.
8. Park SY., Lee GH., Park JM., et al. Clinical characteristics of auricular keloids treated with surgical excision. Korean J Audiol. 2012, 16 (3): 134–137.
9. Mohammadi AA., Kardeh S., Motazedian GR., et al. Management of ear keloids using surgical excision combined with postoperative steroid injections. World J Plast Surg. 2019, 8 (3): 338–344.
10. Gold MH., McGuire M., Mustoe TA., et al. Updated international clinical recommendations on scar management: part 2 – algorithms for scar prevention and treatment. Dermatol Surg. 2014, 40 (8): 825–831.
11. Barolet D., Boucher A. Prophylactic low-level light therapy for the treatment of hypertrophic scars and keloids: a case series. Lasers Surg Med. 2010, 42 (6): 597–601.
12. Tahir SM., Ihebom D., Simman R. Compression therapy for keloid scars: a systematic review and meta-analysis. Plast Reconstr Surg Glob Open. 2024, 12 (6): e5864.
13. Mustoe TA., Cooter RD., Gold MH., et al. International clinical recommendations on scar management. Plast Reconstr Surg. 2002, 110 (2): 560–571.
14. Yin Q., Wolkerstorfer A., Lapid O., et al. KECORT study: an international e-delphi study on the treatment of KEloids using intralesional CORTicosteroids in clinical practice. Am J Clin Dermatol. 2024, 25 (6): 1009–1017.
15. Vettorato E., Volonté P., Musazzi UM., et al. Skin microincision technique to enhance drug penetration for the treatment of keloid and hypertrophic scars. Int J Pharm. 2025, 671 : 125259.
16. Bouzari N., Davis SC., Nouri K. Laser treatment of keloids and hypertrophic scars. Int J Dermatol. 2007, 46 (1): 80–88.
17. Branyiczky MK., Metko D., Hsu JTS., et al. Combination of carbon dioxide laser and triamcinolone acetonide for keloid and hypertrophic scar treatment: a systematic review. J Am Acad Dermatol. 2025, 93 (3): 821–825.
18. Ogawa R., Yoshitatsu S., Yoshida K., et al. Is radiation therapy for keloids acceptable? The risk of radiation-induced carcinogenesis. Plast Reconstr Surg. 2009, 124 (4): 1196–1201.
19. Manuskiatti W., Fitzpatrick RE. Treatment response of keloidal and hypertrophic sternotomy scars: comparison among intralesional corticosteroid, 5-fluorouracil, and 585-nm flashlamp-pumped pulsed-dye laser treatments. Arch Dermatol. 2002, 138 (9): 1149–1155.
Olga Košková, MD, PhD
Department of Burns and Plastic Surgery
University Hospital Brno
Jihlavská 200
625 00 Brno
Czech Republic
koskova.olga@gmail.com, koskova.olga@fnbrno.cz
Submitted: 9. 7. 2025
Accepted: 22. 11. 2025
Labels
Plastic surgery Orthopaedics Burns medicine Traumatology
Article was published inActa chirurgiae plasticae

2025 Issue 4-
All articles in this issue
- Will robots replace us?
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
- Intraoperative cone beam computed tomography in craniomaxillofacial traumatology – a case report
- Digital retractile keloid in a context of spontaneous keloids – a case report
- Extensive keloid scar of the left auricle – combined treatment of excision followed by brachytherapy: a case report
- Post-otoplasty keloid scars – treatment strategies and case reports
- Large urethral false passage during a routine catheterization – low threshold for better outcome
- Acta chirurgiae plasticae
- Journal archive
- Current issue
- Online only
- About the journal
Most read in this issue- Treatment and outcomes of rectus diastasis in post-bariatric patients and postpartum women – a systematic review
- Anterior approach to posterior auricular artery in microvascular anastomosis – a new concept in replanting amputated ears – experience from four successful cases and literature review
- Association between the maxillofacial injury severity score to helmet types, neutrophil lymphocyte ratio and length of stay
- Taylor’s flap reconstruction following abdominoperineal resection for advanced hidradenitis suppurativa – a case series and literature review
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career

