-
Medical journals
- Career
THE MANUFACTURING PRECISION OF DENTAL CROWNS BY TWO DIFFERENT METHODS IS COMPARABLE
Authors: Viktória Rajťúková 1; Irenej Poláček 1; Teodor Tóth 1; Jozef Živčák 1; Gabriela Ižáriková 2; Mila Kovačevic 3; Andrej Somoš 4; Radovan Hudák 1
Authors‘ workplace: Department of Biomedical Engineering and Measurement, Faculty of Mechanical Engineering, Technical University of Kosice, Slovakia 1; Department of Appl. Mathematics and Informatics, Faculty of Mechanical Engineering Technical University of Kosice, Slovakia 2; Faculty of Medicine, University of Novi Sad, Serbia 3; Department of Pneumology and Phtiseology, Louis Pasteur University Hospital, Košice, Slovakia 4
Published in: Lékař a technika - Clinician and Technology No. 4, 2016, 46, 102-106
Category: Original research
Overview
Like all production areas the production of dental replacements, either prosthetic or aesthetic, has recently undergone great advancement due to computer-aided design of dental parts and their computer aided manufacturing. CNC milling, which belongs to the group of subtractive production methods, is very well established in dental production. For the last several years, methods of additive manufacturing, such as Selective Laser Melting (SLM), Selective Laser Sintering (SLS) and Direct Metal Laser Sintering (DMLS), have gone mainstream. In general, both additive and subtractive methods have their technological pros and cons; therefore, the aim of this paper is to determine how accurate in terms of tolerance of production of ± 50 μm both technologies are and afterwards to determine which of the technologies is more accurate. Given that nowadays the most commonly used material in the dental area is cobalt-chromium (Co-Cr) alloy, this alloy was chosen for the experiment. Thirty Co-Cr dental crowns were manufactured for analysis according to the referential CAD model, 15 by CNC milling and 15 by SLM. The crowns were subsequently scanned using a dental 3D scanner, and their inner areas were extracted and compared to the nominal CAD model. The percentage agreement of production is on the level of approximately 94% with both devices, and the average value of agreement as well as the standard deviation and range variation are better with additive production.
Keywords:
additive method, subtractive method, cobalt-chromium, reference model, internal surfacesIntroduction
An alternative to the conventional method [1] of producing dental replacements and constructions are CAD/CAM technologies, which have been developing over the past several years and are now already a part of dental laboratories. Both subtractive [2] and additive [3, 4] production are included among CAD/CAM technologies.
The subtractive method represents the technology of machining material utilizing a CNC milling machine. In the presented paper, dental crowns are manufactured by a 5-axis CNC Ceramill motion 2 milling machine (AmannGirrbach, Austria) [5]. The machine is available for the manufacture of dental replacements from various materials (zircon, wax, PEEK) as well as from Co-Cr (Ceramill Sintron). The CNC machines used in the dental field have predefined shapes (pucks, blocks). However, these technologies have certain limits, e.g. a limited capacity of movement of the machines. Complications arise with the production of complicated geometrical shapes and the cutting of small structures.
The SLM technique is a powder-based additive manufacturing method capable of producing a prosthesis layer by layer from a 3D CAD model and which also has the advantage of CAD/CAM technique. The SLM technique has been widely used in aerospace, aviation, automotive and other industries for many years [6], but it has only recently been employed in dentistry [7, 8, 9]. The basic principle of the SLM technique is to produce prostheses layer by layer according to their shapes by selectively fusing metal powder through computer-aided laser control. This offers several advantages over the conventional CAD/CAM technique, and it also saves raw materials and requires fewer tools, thus reducing costs [10].
In the submitted study the Mlab cusing R device (Concept Laser, Germany), which is employed for the production of titanium alloys and Co-Cr alloys, was used. It uses SLM (Selective Laser Melting) tech-nology. The production process is carried out by gradual depositing of powdered layers of the material remanium star CL with a thickness of 25 µm and their subsequent laser melting. In dentistry it is used for the production of crowns, bridges, model castings and the like. On the basis of a standardized production process it is also possible to make prototypes of small sizes with high precision [11].
Current SLM devices provide metallic restorations made of Co-Cr alloys for removable and fixed partial dentures without compromising the alloy or restoration properties at a fraction of the time and cost, showing great potential to replace the aforementioned production techniques in the long term; however, further clinical studies are essential to increase the acceptance of this technology by the worldwide dental community [12].
The innovative manufacturing concept of SLM offers many advantages compared with casting and milling techniques. SLM provides a microstructure different than those from casting and milling, with minimal internal porosity, internal fitting and marginal adaptation [10, 13].
In the literature available, authors present studies focused on long-term effects, internal and marginal fit [14, 15], the possibilities of applying new production methods in the dental area [15, 17], mechanical pro-perties [18, 19] and microstructural examination at production [14, 20]. Other studies have been devoted porosity [14, 21], electrochemical testing [22, 23] and metal-ceramic bond strength [24, 25, 26].
However, only a few studies have dealt with a com-parison of subtractive and additive technologies. In the current paper 15 crowns were manufactured from Co-Cr alloy using both methods (additive and subtractive); after production, the crowns underwent post-processing (heat treatment, support removal and mechanical treatment). They were then individually scanned using a dental scanner. The data obtained were then compared with the reference model in the VGStudio Max 2.2 software (Volume Graphics GmbH, Germany).
Material and method
It is crucial to know the percentage of chrome (Cr) and cobalt (Co) in the alloy to determine the physical and mechanical properties of the Co-Cr alloy as a whole.
The higher amount of Cr in the alloy, the higher is its corrosion resistance. On the other hand, the higher the amount of Co in the alloy, the higher is its strength, hardness and modulus of elasticity [13].
For production using the additive method the metal powder remanium star CL (Dentaurum, Germany) is used. The material remanium star CL is used for the production of dental crowns and bridges by additive technology and satisfies the requirements of the standards EN ISO 969 and DIN EN ISO 22674. The size of its grain is from 10 µm up to 30 µm.
Ceramill Sintron (AmannGirrbach, Austria) is used for the production of crowns and bridges using the subtractive method. In line with the standard DIN EN ISO 22674 : 2007, the alloy does not contain the elements Ni, Be, Ga and Cd. As was mentioned above, this is a metal powder pressed into the shape of a puck.
The practical part of the experiment deals with a description of the subtractive and additive production methods, a comparison of the individual production methods with regard to the achieved precision, and the repeatability of the production of crowns from the
Co-Cr alloy made by the additive method with crowns made by the subtractive method.Design of the CAD model
The basis for both the subtractive and additive methods is the 3D model of a dental replacement, which is prepared by a dental technician. Fig. 1 shows the 3D model of a crown which was used as the reference model for further production.
Fig. 1: Referential model of the crown. 
Method of preparation for the production of crowns
For preparation of the 3D model made using additive production the software CAMbridge was used. The 3D model is correctly positioned in the software; the support material is designed (Fig. 2a) and is placed on the production surface (Fig. 3a). After completing modifications a file of the *.cls format is generated, which is subsequently loaded into the Mlab cusing R device.
Preparation of the 3D model for the subtractive method was done in the Ceramill Match software. The material used is selected in the software and the contour edges are demarcated. The number and thickness of the anchors are entered (Fig. 2b) and placement in the puck is defined (Fig. 3b).
Fig. 2: Method of preparation of referential model in the CAMbridge software (a) and Ceramill Match software (b). 
Fig. 3: Arrangement of the referential model on the building plate (a) and in the puck (b). 
After preparation of the data, the production process – cutting (the subtractive method) and pressing (the additive method) – is initiated. The dental replacements produced are subsequently annealed and modified to their final form.
Scanning of samples – pre - and post - processing
To acquire the digital data of the surface of the manufactured dental crowns the dental 3D scanner Identica (Medit, Seoul, South Korea) was used. The scanner is primarily intended for scanning dental plaster castings, the surface of which is matt and with a constant colouring. During production of the crowns the surface was not matt; for this reason a chalk casing was deposited on all the scanned objects.
The area for setting the tooth – the internal surface – was evaluated; therefore, the acquired scans were cleaned of unwanted noise and at the same time only the selected area was left, as is given in Fig. 4.
Fig. 4: Process of scan modification. 
Results and Discussion
Comparison of samples with the reference model
The acquired scans of the individual crowns in the form of STL files were compared with the reference model in the Volume Graphics VGStudio Max 2.2 software (Volume Graphics GmbH, Germany).
The result of the comparison is the percentage value of agreement of the scan of the real implant with the reference model. This is the most suitable method of evaluation for the purpose of analysis in this study, because it provides data on deviations over the entire monitored surface of the crown, not only in isolated locations, which do not have to capture the maxima or minima.
For evaluation of deviations it is in general necessary to determine the coordinate system of the reference model and a method of aligning the scan to the reference. Because the dimensions are not plotted, the original coordinate system of the reference model was used.
Alignment of the scan with the reference ran in two stages. The first stage is alignment using the Best-fit method and the second using the reference positioning system (RPS). Best-fit is necessary to use for the best possible “rough” alignment of the objects.
The Best-fit method uses the least squares principle, i.e. the deviations between the scan and the model is mathematically segmented. This method is not appropriate in cases when the obtained scan and the 3D model significantly differ at some locations, as the calculation might, in an effort to minimise the deviations, shift the alignment and thus the result must not necessarily correspond to the reality.
This was the first reason for removing the super-fluous surfaces from the acquired scans, because distant surfaces can influence or disable alignment using this method. In Fig. 5 the alignment in the case of a significant deviation between the compared and the reference model is depicted. For the selected tolerance bounds, the green colour represents the surroundings of the centre of the toleration field and other colours of its edge, or the field outside the prescribed tolerance.
Fig. 5: Best-fit alignment and its results with significant size deviations. 
The final alignment was performed using the RPS method, where it is aligned on set points (Fig. 6) covering the assessed surface, aside from the edges and top of the implant, where the origin of local maxima/minima is assumed in consequence of pro-duction or scanning. These extremes can unfavourably influence the result of the alignment.
Fig. 6: Reference points for RPS alignment. 
Analysis of acquired data
A comparison of the scan with the reference model was performed in the Nominal-Actual Comparison module of the VGStudio MAX 2.2 software.
The toleration field for the maximum permitted deviation of production was set at ± 50μm. The value of ± 300 μm was selected as the maximum assessed deviation, i.e. the software evaluated the deviation from the reference model in this range. Fig. 7 shows the nominal model (orange), the actual scan (yellow) and their mutual covering and comparison. The green colour in the comparison represents the toleration field ± 50μm.
Fig. 7: Nominal – actual comparison. 
Tab. 1 represents the percentage agreement of the scan with the reference model with a maximum deviation of 50 μm for crowns made from the Co-Cr alloy by the subtractive and additive method. With respect to the fact that all of the non-relevant parts of the scan were removed, the percentage agreement is not influenced by them and represents the real value of the percentage agreement.
1. Percentage agreement of Co-Cr crowns with the reference model for additive and subtractive production. 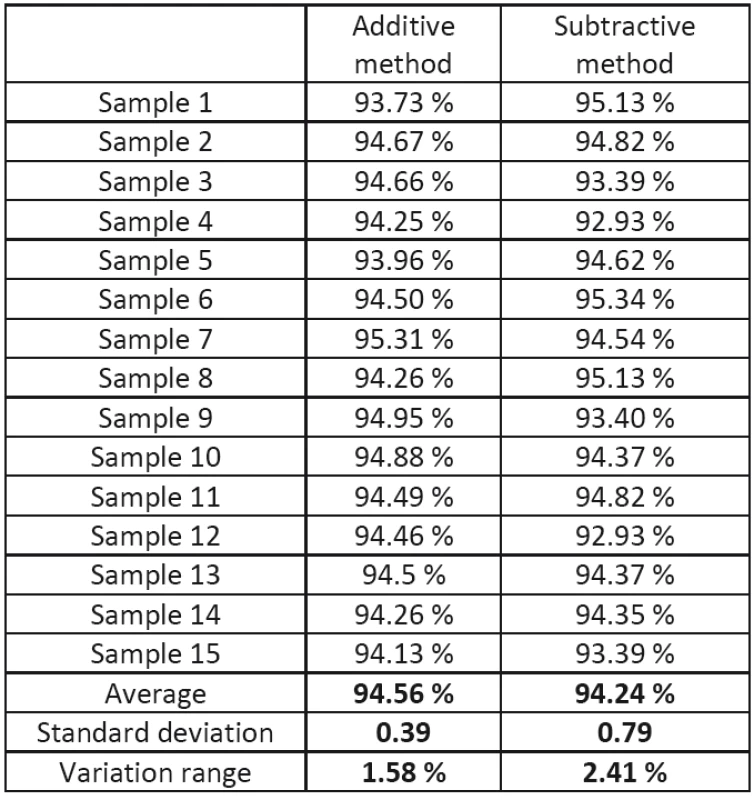
From the results it follows that the average agreement for additive production is higher by 0.32% than with the subtractive method. Equally, the standard deviation and variation range are smaller with additive production.
Statistical processing of acquired data
Statistical processing of the acquired data verified whether there is a significant statistical difference between the samples of crowns made from cobalt-chromium alloy produced by the subtractive and the additive method.
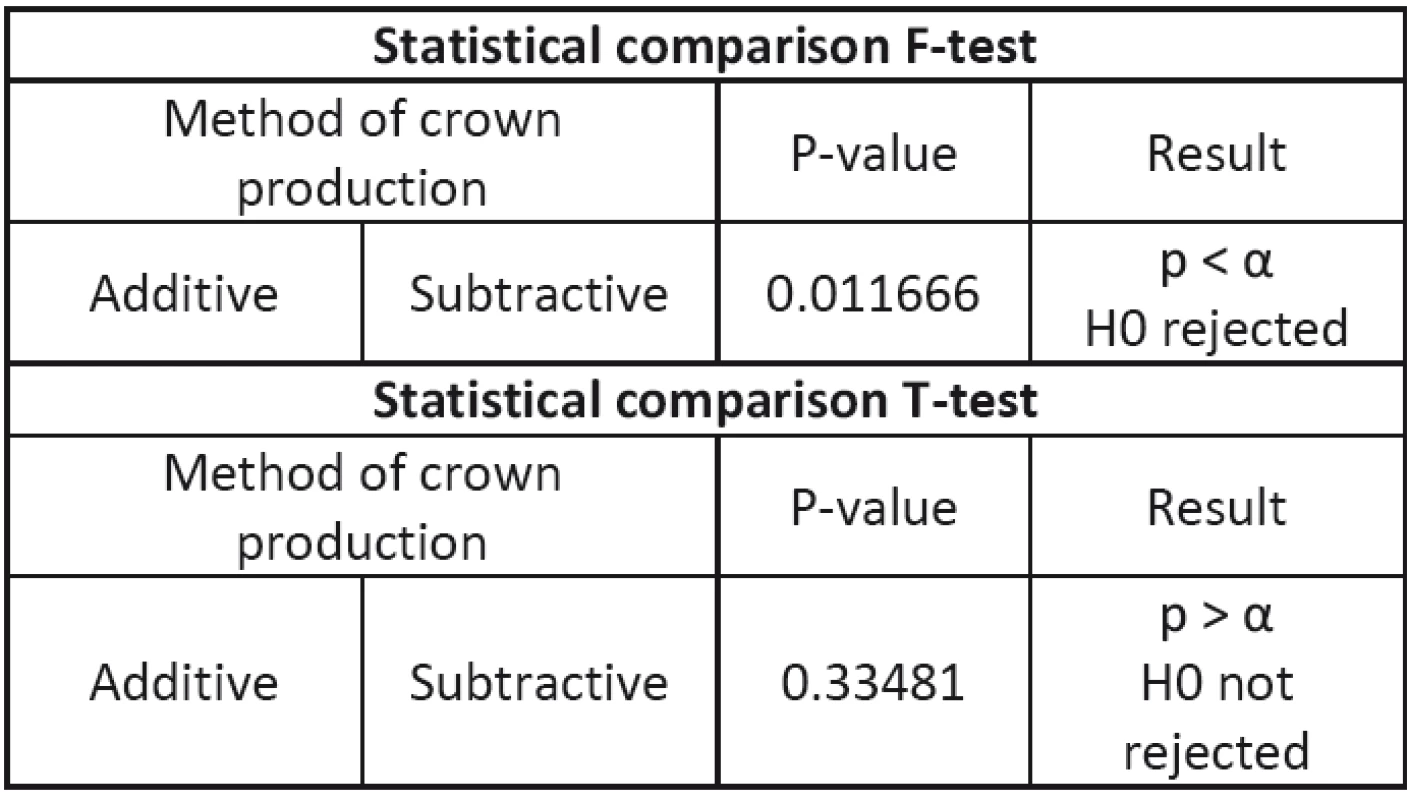
A two-sample F-test of equality of variances was used for variance, where the hypothesis on agreement of the variances of the two files is tested and on the basis of its results the T-test is approached with equality/inequality of the variances. The T-test was used for independent selection; this is a method for evaluating the difference in the average of two groups. The p-value obtained is compared with the value of the level s of significance α, the value of which 0.050.
In Tab. 2 the F-test and the T-test are used for statistical comparison.
Using the T-test it was determined that no sta-tistically significant difference was found between the samples of crowns from the cobalt-chromium alloy produced by the subtractive and additive methods.
Conclusion
From the presented results it follows that production on the Mlab Cusing R (Concept Laser, Germany) and Ceramill motion 2 (AmannGirrbach, Austria) devices is, in relation to the precision of production, comparable on the level of 50 μm. This result is confirmed by statistical processing of the acquired data. The percentage of agreement of production is with both devices on the level of approximately 94%, and the average value of agreement, value of the standard deviation and variation range are better during additive production.
Acknowledgement
The work was supported by research grant No. ITMS 26220220185 of the project: Medical University Science Park in Kosice (MediPark) and “Manu-facturing and testing of custom made bone scaffolds made of hydroxyapatite (HA) using 3D printing tech-nology” (APVV – 14 – 0294) and Experimental and computerised biomechanical testing of implantable me-dical devices and the implementation thereof in the education process (064TUKE-4/2016).
Ing. Viktória Rajťúková, Ph.D.
Department of Biomedical Engineering and Measurement
Faculty of Mechanical Engineering
Technical University in Kosice
Letna 9, 042 00 Kosice
Email: viktoria.rajtukova@tuke.sk
Phone: +421 055 602 2651
Sources
[1] Noort, R: The future of dental devices is digital. Dent Mater 2012; ISSN 0957-4530, 28 : 3–12.
[2] Samet, N., Resheff, B., Gelbard, S., Stern, N.: A CAD/CAM system for the production of metal copings for porcelain-fused-to-metal restorations. J Prosthet Dent, ISSN 0022-3913, 73 (1995), pp. 457–463.
[3] Quante, K., Ludwig, K., Kern, M.: Marginal and internal fit of metal–ceramic crowns fabricated with a new laser melting technology. Dent Mater, 24 (2008), ISSN 0109-5641, pp.
1311–1315.
[4] Traini, T., Mangano, C., Sammons, R.L., Mangano, F., Macchi, A., Piattelli, A.: Direct laser metal sintering as a new approach to fabrication of an isoelastic functionally graded material for manufacture of porous titanium dental implants. Dent Mater, 24 (2008), ISSN: 0957-4530, pp. 1525–1533.
[5] Amann Girbach, [online 11.05.2016] https://www.amanngirrbach.com/en/products/milling-cam/ceramill-motion-2-5x/
[6] Yadroitsev, I., Bertrand, P.H., & Smurov, I. (2007). Parametric, analysis of the selective laser melting process. Applied Surface Science, 253, 8064–8069.
[7] Jenča, A., Jenčová, J., Jenča, A. ml., Jenčová V.: Dentálny implantát a efektivita remodelácie ortognátneho systému. In: Seminar Sučasti technologii v stomatologii: Užgorod: Prat "Vydavnyctvo Zakarpattja", 2012. - S. 49–55.
[8] Mazzoli, A: Selective laser sintering in biomedical engineering. Med Biol Eng Comput 2013; 51 : 245-56.
[9] Kumar, S: Selective laser sintering: a qualitative and objective approach. Jom-J Min Met Mat S 2003; 55 : 43–47.
[10] Xin, X.Z., Chen, J., Xiang, N., Wei, B.: Surface properties and corrosion behavior of Co-Cr alloy fabricated with selective laser melting technique. Cell Biochem Biophys 2013; 67 : 983–90, ISSN: 1085–9195.
[11] Concept laser, dental machines, [online 11.05.2016]. http://www.concept-laser.de/en/industry/dental/machines.html.
[12] Hughes, Kate: A 3D printed future. Inside Dental Technology [online 11.05.2016] http://www.dentalaegis.com/idt/2013/04
[13] Choi, Y.J., Koak, J.Y., Heo, S.J., Kim, S.K., Ahn, J.S., Park, D.S.: Comparison of the mechanical properties and micro-structures of fractured surface for Co-Cr alloy fabricated by conventional cast, 3-D printing laser-sintered and CAD/CAM milled techniques. J Korean Acad Prosthodont. 2014 Apr; 52(2):67–73.
[14] Ucar, Y., Akova, T., Akyil, M.S., et al: Internal fit evaluation ofcrowns prepared using a new dental crown fabrication tech-nique: laser-sintered Co-Cr crowns. J Prosthet Dent 2009; ISSN: 0022-3913, 102 : 253–259.
[15] Örtorp, A., Jönsson, D., Mouhsen, A., Vult von Steyern, P.: The fit of cobalt–chromium three-unit fixed dental prostheses fabricated with four different techniques: A comparative in vitro study, Dental Materials, Volume 27, Issue 4, April 2011, Pages 356–363, ISSN 0109-5641.
[16] Jenča, A., Jenčová, V., Jenčová, J., Jenča A. ml.: Dentálny implantát a jeho osteointegrácia ako náhrada piliera, In: Implantológia a pokročilé implantáty : zborník referátov: Košice, 28.11.2011. - Košice: Univerzita Pavla Jozefa Šafárika v Košiciach, 2011. - ISBN 9788097096410. - S. 172–179.
[17] Koutsoukis, T., Zinelis, S., Eliades, G., Al-Wazzan, K., Rifaiy, M. A. and Al Jabbari, Y. S. (2015): Selective Laser Melting Technique of Co-Cr Dental Alloys: A Review of Structure and Properties and Comparative Analysis with Other Available Techniques. Journal of Prosthodontics, ISSN 2005-7806,
24 : 303–312. doi:10.1111/jopr.12268.
[18] Kruth, J.P., Mercelis, P., Van Vaerenbergh, J., et al: Binding mechanisms in selective laser sintering and selective laser melting. Rapid Prototyping J, ISSN 1355-2546, 2005; 11 : 26–36.
[19] Yamanaka, K., Mori, M., Kuramoto, K., et al: Development of new Co-Cr-W-based biomedical alloys: effects of micro alloying and thermomechanical processing on microstructures and mechanical properties. Mater Des 2014; ISSN 0264-1275, 55 : 987–998.
[20] Takaichi, A., Suyalatu, Nakamoto, T., et al: Microstructures and mechanical properties of Co-29Cr-6Mo alloy fabricated by selective laser melting process for dental applications. J MechBehav Biomed Mater 2013; ISSN 0957-4530, 21 : 67–76.
[21] Munoz, A.I., Mischler, S.: Effect of the environment on wear ranking and corrosion of biomedical CoCrMo alloys. J Mater SciMater Med, ISSN 0957-4530, 2011; 22 : 437–45.
[22] Reclaru, L., Ardelean, L., Rusu, L., et al: Co-Cr material selection in prosthetic restoration: Laser sintering Technology. Solid State Phenomena 2012; ISSN 1662-9779, 188 : 412–415.
[23] Rodrigues, W.C., Broilo, L.R., Schaeffer, L., et al: Powder metallurgical processing of Co-28%Cr-6%Mo for dental implants: physical, mechanical and electrochemical properties. Powder Technol 2011; ISS: 0032-5910, 206 : 233–23.
[24] Kim, K.B., Kim, J.H., Kim, W.C., et al: Evaluation of the marginal and internal gap of metal-ceramic crown fabricated with a selective laser sintering technology: two - and three-dimensional replica techniques. J Adv Prosthodont 2013;5 : 179-186, ISSN 2005-7806.
[25] Roberts, H.W., Berzins, D.W., Moore, B.K., et al: Metal-ceramic alloys in dentistry: a review. J Prosthodont 2009;18:
ISSN 1532-849X 188-19448.
[26] Akova, T., Ucar, Y., Tukay, A., Balkaya, M.C., Brantley, W.A.: Comparison of the bond strength of laser-sintered and cast base metal dental alloys to porcelain, Dent Mater, 24 (2008), pp. 1400–1404.
Labels
Biomedicine
Article was published inThe Clinician and Technology Journal

2016 Issue 4
Most read in this issue- CARDIOPULMONARY EXERCISE TESTING FOR VO2MAX DETERMINING IN SUBJECTS OF DIFFERENT PHYSICAL ACTIVITY
- THE MANUFACTURING PRECISION OF DENTAL CROWNS BY TWO DIFFERENT METHODS IS COMPARABLE
- COMBINATION OF ATOMIC FORCE MICROSCOPY AND COMET ASSAY FOR ANALYSIS OF DNA DAMAGE INDUCED BY PDT
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career