-
Medical journals
- Career
Supracondylar Fractures of Distal Humerus in Children – Results of Operative Treatment
Authors: Jan Fuit; Petr Menšík
Authors‘ workplace: Krajská nemocnice T. Bati, a. s. Zlín, Traumatologické oddělení
Published in: Úraz chir. 27., 2020, č.2
Overview
Objective: To assess the treatment of supracondylar fractures of the distal humerus in children, which were treated in Tomas Bata Hospital, Zlin. To evaluate the results in the context of contemporary studies.
Introduction: Study presents the supracondylar fracture.
Method: Retrospective study of a group of 228 patients with this type of fracture, treated between the years 2014-2018 in Traumatology department of Tomas Bata Hospital, Zlin.
Results: In this group, 4 children underwent closed reduction and splinting in general anesthesia, 95 were operated on, from which 94,5 % urgently (less than 6 hours after first contact with the patient). The prefered method was closed reduction and percutaneous pinning by crossed Ki wires (CRCPP). In 12 cases (12,6 % of the operations) it was necessary to perform an open reduction, mostly from the limited posterior access. In the group of operatively treated children, there have been noticed 20 cases of some neural injury, mostly n. ulnaris (12), both n. ulnaris and medianus (4), n. medianus only (3). There were 2 cases of pale-pulsless hand after the reduction, which led to the revision of the neurovascular structures from the anterior access. None of the children displayed permanent consequences envolving their everyday lives. In minority of cases (14) at the end of the follow-up, persisted slight deficiency of the flexion, or slight hyperextension of the elbow, or the combination of both. We have recorded 2 cases of the cubitus varus deformity. In this cohort, there was no incidence of the compartment syndrome nor the Volkmann contracture of the extremity.
Conclusion: Supracondylar fracture is a frequent injury with relatively high risk of complications. Some questions of the optimal treatment have still not been answered and need further research.
Keywords:
Supracondylar fracture – urgent surgery – percutaneous pinnig – cubitus varus
Introduction
Elbow injuries are the reason for about 1–3 % of all acute visits of paediatric and adolescent patients [2]. This number is likely to continue to grow, given that since 2010 we have seen an increase in children‘s sports activity in the Czech Republic and the popularity of riskier outdoor sports has been increasing. [12]. Fractures in the region of the elbow joint represent about 5–10 % of all children‘s fractures. The most common of these are the supracondylar fractures - 55–70 % [7,19].
There are numerous classification schemes, the most globally used of which is the Gartland classification (1959), traditionally defining 3 types of fractures. Type I – non-dislocated fractures or fractures with minimal dislocation up to 2mm, respectively. Type 2 – fractures dislocated with fragments in contact with intact dorsal periosteum of the humerus, which was subsequently divided by Wilkins (1984) into type IIA – without rotatory dislocation - and type IIB – with a proportion of rotatory dislocation, type III – grossly dislocated fractures without contact of fragments, unstable in extension, in which dorsal periosteum is usually partially preserved [9, 13]. Type IV of Gartland classification is newly distinguished, which includes fractures significantly unstable, with a tendency to dislocation into both flexion and extension, difficult to reduce. Usually, this type is only detected during handling at the operating room and it is assumed to have a total disrupture of the humeral periosteum [13].
In our conditions it is necessary to mention the classification according to Havránek, which emphasizes the variability of fractures and different treatment procedures. It defines six types of fractures. Type 0 – nondislocated fractures, Type 1 – extension fractures, Type 2 – flexion fractures, Type 3 – indifferent fractures with significant ad latus dislocation in the frontal plane, without a clear share of flexion/extension component. These are highly unstable, difficult to treat fractures, Type 4 high fractures, which are characterized by relatively easy reduction, but pronounced instability, and finally Type 5 involving atypical fractures (with break-out of the medial or lateral column, separate fragment of epicondyle and intercondylar „T"-shaped fractures [10].
The etiology of supracondylar fractures copies the physical activity of children, with falls from a height in the home environment – from bed, chair, etc. predominating in young children under 4 years of age. In preschool children, frequent fractures are caused by falling from structures of children‘s playgrounds – climbing frames, swings, slides, and with increasing age also sports injuries – falls from the bike, trampolines, roller skates, gymnastic tools [2, 3]. In fractures of the extension type, the most common mechanism of injury is a fall on the extended forearm. Here, physiological elbow hyperextension plays its role in children and the ulnar olecranon acts as a lever, which together with the collateral ligaments of the elbow concentrates the resulting forces on the ventral humeral cortical thickening and its disruption occurs. In fractures of the flexion type, the most common mechanism is direct – a fall on the flexed elbow [3, 16].
When diagnosing a supracondylar fracture, in addition to taking the necessary case history, physical examination of the limb is critically important. The classical physical examination procedure should be modified in a young patient [3]. The most important part of examination is the observation. It is necessary to notice the posture of the limb, swelling, haematoma, deformities of the elbow, skin bruises, ecchymosis, or drawn-in skin symptom. The presence of a skin wound can predict the diagnosis of an open fracture, the colour of the periphery of the limb and the mobility of the fingers indicates circulatory and neurological situation. During palpation examination, we follow the rule of starting from non-painful components (examination of peripheral pulsation of a. radialis, capillary return on the fingers, indicative neurological examination) to more painful steps (palpation of the elbow itself), which is reserved for the end of the examination [2]. Simple X-ray scans in two projections are sufficient to determine the diagnosis of the supracondylar fracture, although precise classification often requires an x-ray amplifier assessment in the operating room [10, 19]. Nondislocated fractures can cause differential diagnostic embarrassment, and sometimes it is difficult to distinguish a supracondylar fracture from other types of fractures. Alternatively, due to the relative variability of the ossification zones of the elbow, from a physiological finding. In such cases, it is advantageous to perform comparative X-ray scan of the second elbow. When assessing dislocation of the fracture, we evaluate the alteration of the natural parameters of the child‘s elbow. The physiological antecurvation of the humeral head is a natural ventral angulation between the humerus axis and capitulum humeri axis. This tilt averages from 25 to 40° [10]. Dislocations in the sagittal plane results in the change of this angle, which can be verified by assessing the anterior humeral line (AHL). It is a straight line resulting from the extension of the anterior humeral cortical thickening in the side projection. In children over 4 years of age, it intersects the middle third of capitulum humeri; in children under 4 years of age, it usually intersects the middle of the anterior third of capitulum [11]. If the anterior humeral line does not intersect the capitulum humeri, it is a dislocated supracondylar fracture. In the AP projection, the measurement of Bauman‘s angle is used to assess the dislocation in the frontal plane. It is a residual angle formed by the lines of the growth zone of capitulum humeri and the line that is perpendicular to the long axis of the humerus. Normal Baumann‘s angle is between 9° and 26°; where the angle is less than 9°, we are talking about a cubitus varus-type dislocation of the cubitus [3]. We do not use Baumann‘s angle very much at our site because it depends to much on the accuracy of the X-ray projection, and therefore it is unreliable. In order to assess the axis of the elbow in the frontal plane, the „carrying angle“ between the axes of humeral diaphysis and ulnar diaphysis is of practical importance. Its physiological range is from 5 15° of the valgus [3]. This angle also depends on the X-ray projection and it is expressed in the supination of the forearm only [10].
Treatment of supracondylar fractures is determined by the type of dislocation of the fracture. Stable nondislocated fractures or fractures with minimal dislocation of Gartland type-I, without neurovascular injury, should be treated conservatively by plaster fixation in the flexion of the elbow at the angle of 60-90° for a total of 3 weeks [10, 16, 19, 21]. Then the warm-up is to begin, with the full range of movements and return to all activities restored between week 5–9 from the removal of fixation. In the treatment of fractures of Gartland type-II there is no consensus among the authors between conservative treatment of reduction and plaster fixation and percutaneous osteosynthesis with Ki wires. Particularly in the stable fractures of Gartland-type II, some publications recommend to proceed rather conservatively [4, 15]. In contrast, other authors point out that fractures of the extension type treated by plain reduction need to be plastered at an angle greater than 90 degrees of the flexion, which may result in altering the vascular conditions on the forearm and the risk of developing a compartment syndrome. [10, 21]. Another argument for surgical treatment is the possibility of losing the reduction. Percutaneous osteosynthesis eliminates the need for regular X-ray checks, but requires procedure at the operating room. Dislocated Gartland type-IIB to IV fractures, fractures of the flexion type, and unstable fractures are indicated for reduction and percutaneous osteosynthesis with Ki wires. [3, 10, 21].
The treatment of a dislocated supracondylar fracture is perceived as an urgent procedure at many sites. However, there are foreign works that describe excellent results in a set of patients treated with deferred treatment. Abdullah et al. (2008) already presented the results of 31 children with a Gartland type-III fracture operated by the open reduction method and percutaneous pinning method, where the average time between injury and surgery was 6 days. No higher risk of perioperative complications was observed, none of the patients had a movement limitation at the end of treatment. A recent meta analysis conducted by Farrow (2019) processed data from 12 major clinical studies comparing urgent procedures versus deferred procedures in supracondylar fractures without blood perfusion deficit. There was no significant difference in the number of conversions to open procedure, infection complications, iatrogenic nerve injury, or higher incidence of reosteosyntheses [8]. Prabhakar (2019) also published a study of 309 children with a Gartland type-III fracture and did not find any difference in the duration of the procedure and the duration of peroperative sciascopy in procedures postponed for 15 hours as compared to urgent ones [16]. These studies confirm the theory that the quality of procedure performed at the site with enough experience is of greater importance than the actual urgency of procedure itself.
The method of choice for fixation is percutaneous fixation with Ki-wires introduced from retrograde approach through the fragment of fracture into the metathesis of the humerus; the optimal number of wires is 2–4 depending on the character (comminution) and the degree of instability of the fracture. In our conditions, the cross introduction of wires across the radial and ulnar epicondyle of humerus [10, 21]. In the world literature, the introduction of wires from the radial epicondyle of the humerus is more often promoted in order to eliminate the risk of injury to n. ulnaris. Biomechanical studies of recent years [6, 14, 18] show even greater stability of such performed osteosynthesis and they recommend Ki-wire introduced from ulnar approach only in case of comminution of the medial column.
Associated injuries and complications of the treatment
Localization of the fracture in close proximity to important neurovascular structures and growth zones of the distal humerus predisposes to formation of associated injuries. According to a large multicentric study of Skaggs and Flynn, who collected data from 64 large clinical studies, peripheral nerve lesions occur in 7 % of all fractures, in type-III fractures in up to 20 %; in the case of percutaneous fixation through the ulnar epicondyle of the humerus, the probability of iatrogenic lesion of n. ulnaris is reported in literature to be around 0.03 [14, 21], in 10–20 % of type-III dislocated fractures certain degree of vascular lesion is reported [21]. An injury to a. brachialis can clinically manifest as a pale acral part of the limb with non-palpable pulsation on the peripheral arteries (pale pulseless); this finding requires an urgent solution. Alternatively, a vascular lesion may occur on a. brachialis with non-palpable pulsation on the periphery, but with a good capillary return (pink pulseless). An explanation of this symptom consists in sufficient vascular supply through collateral circulation. To this day there has been no clear consensus in respect of the management of vascular injury in a supracondylar fracture. Delniotis (2018) published an extensive study involving 608 fractures with impaired pulsation and offered a summary of the optimal solution. In the case of a pulseless limb (pale or pink), he recommends an urgent reduction of the fracture; return of pulsation to a. radialis subsequently occurs in 57.4 % of the cases. If there is no immediate capillary return, he recommends an open revision from the front approach. In case of sufficient blood supply to the periphery, there is a possibility of close monitoring for at least 48 hours under oxymeter monitoring and with Dopplerimetric control, this dogma being referred to as „watchful expectancy“ [6]. It includes the possibility of an urgent revision by a vascular surgeon, should the return worsen. Other complications are less common, and they include an ipsilateral fracture of the forearm (1 %), an open supracondylar fracture (1 %), and a compartment syndrome (1 %), which, if not addressed in time by fasciotomy, results in the dreaded Volkmann contracture of the hand (0,5 %) [19].
A specific complication of supracondylar fracture is represented by the cubitus varus-type of elbow deformity, which according to contemporary works occurs in 0–10 % of cases, previously in up to 60 % of cases [3, 10, 21]. In Anglo-Saxon literature, this disorder is referred to as the so-called „gunstock” deformity due to the shape of elbow resembling the outline of a gun. It is mostly caused by inadequate reduction, more rarely by secondary collapse of the medial column, or by a slowdown in the growth of the trochlear part of the humeral physis or, conversely, by acceleration of growth on the lateral side of the physis [10]. Varous elbows with angulation over 20° often cause the restriction of extension, chronic pains, development of elbow instability, cracking/skipping in the tricipital region, and are to be addressed by corrective osteotomy [3].
According to Havránek, the limitation of movement in terms of deficiency in flexion, extension or hyperextension in the elbow, as appropriate, occurs quite often (up to 10 % of the injured persons). In the extensive study of Skaggs and Flynn, they are rated as rare [19].
Methodology
The aim of the thesis is to evaluate 5-year results of treatment of supracondylar fractures in Tomas Bata Hospital, Zlin. Patients with this injury were retrospectively retrieved according to the hospital‘s medical documentation and data on their treatment were evaluated, i.e. age, sex, date of injury, mechanism of injury, method of treatment, time of start of surgery from admission to the hospital, including type of surgery, total duration of treatment, occurrence of complications, particularly neurological and vascular complications, growth disorders, movement limitations, and other consequences of the trauma. Duration of monitoring of the patients having received the operational treatment was at least 1 year from the surgery. No further monitoring was carried out in conservatively treated patients. To verify the data in the documentation, parents of all operated children were contacted by telephone and a short questionnaire covering the above details was conducted. The disputed cases and lasting consequences were evaluated by the current clinical or x-ray control, as appropriate, at the Traumatology Outpatient Clinic. 5 probands (5.3 %) have not been retrieved properly.
Results
At our site, we treated a total of 228 paediatric patients with supracondylar humerus fracture from 2014 to 2018. Their average age was 6.38 year. The incidence of fractures during the year was of a seasonal character and increased in the summer months (Chart 1). The most supracondylar fractures occurred in September (17 %). The safest month in terms of this injury was December. In the specified set of children, 127 were treated conservatively with plaster fixation of the limb for a total of 3 weeks with regular checks. 4 patients were treated by reduction and plaster fixation under general anesthesia/analgosedation, 95 by reductions and osteosynthesis with retrogradely introduced Ki-wires and plaster fixation, supplemented by a suspension, where appropriate. Two patients were operated at another hospital due to the wishes of their parents. At out site, the operation of a supracondylar fracture is perceived as an urgent procedure. The majority of patients, i.e. 90 (94,7 %), was operated within 6 hours from arrival to the outpatient department. The average time from the first contact with the patient to the beginning of surgery was 2.9 hours. The preferred method was closed reduction and crossed percutaneous Ki-wire fixation (CRCPP) using 2–4 Ki-wires depending on the stability and degree of comminution of the fracture (Fig. 1, 2, 3).
1. Distribution of supracondylar fracture during the year 
1. Dislocated type III fracture 
2. The same fracture - perioperative scan 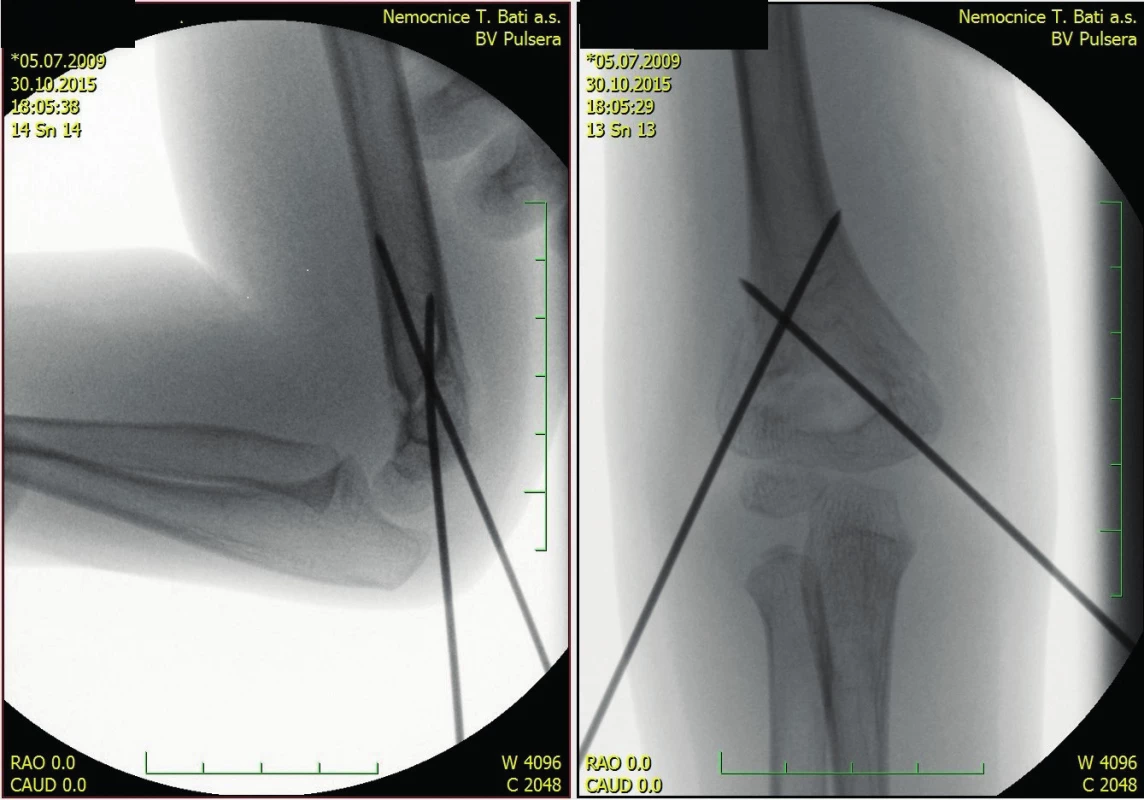
3. Supracondylar fracture fixed in correct position, scan at 3 weeks 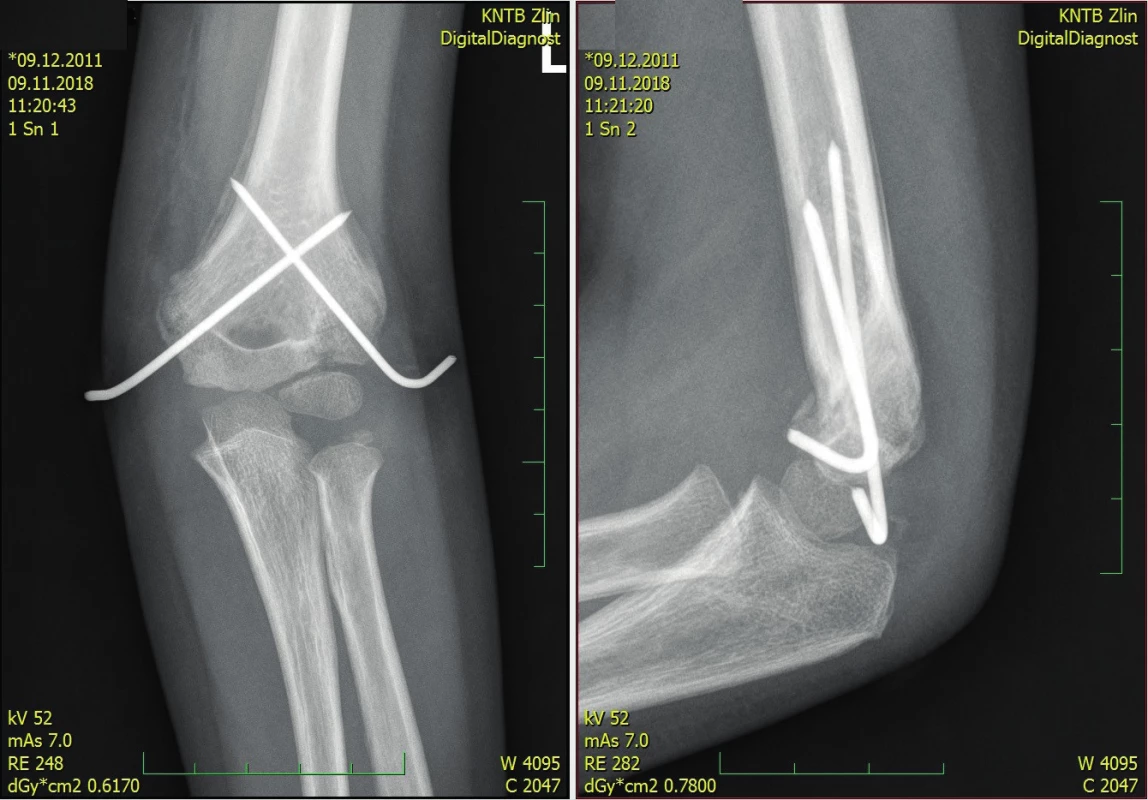
In 12 children (12.6 % of the operated ones) open reduction had to be used, of which in 2 cases due to impaired limb circulation after a closed reduction of the fracture. In the remaining cases, the reason was the impossibility to perform a closed reduction (irreducible fracture). The reasons listed in the operational protocol included inserted periosteum (4), a significantly comminuted fracture with a significant dislocation (2), in the remaining cases the protocol lists reasons like 'significant instability' (2), or the reason was not given (2). A relatively higher percentage of open procedures is due, among other things, to the preferences of some surgeons who tend more easily to conversion to open procedure. At our site, this is typically carried out from a limited rear approach (10 cases) or, with suspected vascular injuries, from the anterior approach (2 cases). In the group of children treated with surgery, 20 cases (21.5 %) of neurological complications were reported, in this mostly the injuries of n. ulnaris - 12 times (60 %), or n. ulnaris as well as n. medianus - 4 times (20 %), or n. medianus separately - 3 times (15 %); severe paresis of nervus radialis occurred in 1 case (5 %). With regard to the retrospective evaluation of the data according to the records in the medical documentation, it was sometimes difficult to assess whether the nerve injury was related to the injury itself or it only occurred in the postoperative period. However, the available data showed the development of paresis of n. ulnaris immediately after surgery in 3 patients (3.15 % of the operated patients), which may indicate an iatrogenic lesion of n ulnaris resulting from the introduction of Ki wire from the ulnar epicondyle of the humerus. All these wounds healed conservatively without consequences. 1 patient developed, after a few weeks from the surgery, a severe paresis of n. ulnaris due to the tension from the scar with the need for neurosurgical procedure – nerve deliberation. In the postoperative period, we also noted the following complications: failure of osteosynthesis and loss of reduction in 3 cases (3.15 %) - solved by re-osteosynthesis, 1 case of infectious complication, which forced timely extraction of the metal and ATB therapy, and subsequently there was healing without consequences. In 14 children (14.7 % of all operated children) there was a slight limitation of movement even after more than 1 year, despite professional rehabilitation, which did not affect quality of life: most frequently it was elbow hyperextension, restriction of elbow flexion, which did not exceed 5–10°, or a combination of both phenomena. A higher incidence of movement disorders was observed in open procedures (in 4 out of 12 cases). Furthermore, growth deviations in the sense of cubitus varus (gunstock deformity) were evaluated, with only 2 girls showing a fully expressed deformity with a varous carrying angle (Fig. 4, 5).
4. Cubitus varus on the left 3 years after the injury compared to the healthy side 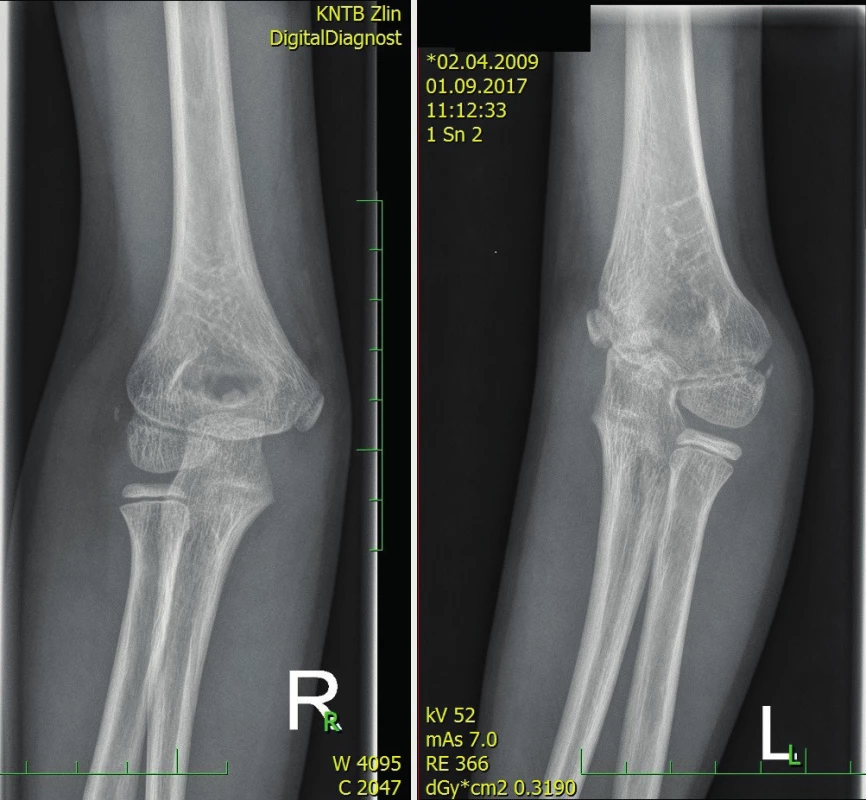
5. Same patient at 10 years of age 
None of them experiences any difficulties after 4 and 5 years after the injury, respectively, or any limitation of their normal daily activities; on the contrary, they are engaged actively in sports. Aseptic necrosis of the humeral trochlea was detected in one girl after a two-year interval; it was solved conservatively with elimination of extensive load on the limb. There was no case of compartment syndrome or Volkmann contracture throughout the set.
Discussion
By comparing the experience of our site with the results of current works, we can conclude that the data regarding the age structure and the injury mechanism are comparable to other works. As for the concomitant nerve injury, our results vary somewhat. Štichauer published a comprehensive set of 459 patients operated due to supracondylar fracture in 2017, with 14.9 % incidence of peripheral nerve injury, with a predominance of n. medianus (r. interosseus anterior) occurring as an isolated injury in 58 %, while the injury of n. ulnaris was observed in 23.7 % [20]. Our ratio is rather the opposite, which can be most likely explained by underdiagnosing of the paresis of r. interosseus anterior, which is manifested only by the paresis of m. flexor pollicis longus and m. flexor digiti II. superficialis and can therefore easily escape attention. According to Skaggs and Flynn [19], the injury of n. radialis amounts for as much as 41.2 % of nerve lesions, but in our population it occurred in 1 case only. We admit the risks of injury of n. ulnaris iatrogenically upon Ki-wire cross fixation, but their percentage was acceptable in our patients (3.15 %) and comparable to foreign publications [3,14]. All such pareses were managed conservatively with the contribution of the specialist rehabilitation. In case of persistent movement disorder in terms of elbow hyperextension, restriction of flexing in the elbow, or combination of both due to a change in the physiological antecurvation of the humerus, i.e. healing in a slightly non-anatomical position, we are in relative accord with the publication of Havránek (2013) as to the frequency of such disorder (2013). Varous angulation of the elbow occurred rarely, i.e. only in 2 girls from a set of 95 operated ones, and did not achieve such a degree as to cause any problems or cause corrective osteotomy of the humerus.
Works around the world usually do not deal with rehabilitation after a supracondylar fracture; some works present the view that the physical activity of children alone is sufficient to restore the range of movements [17]. At our site, professional rehabilitation is the rule and we have good experience with it. Often a non-dominant limb is injured, which leads to the neglected exercising of the limb and therefore it is necessary to motivate the child to exercise.
Conclusion
Supracondylar fractures in children are a fairly common injury encountered by every department of trauma surgery. Their proper treatment will still pose a challenge due to possible perioperative risks and subsequent complications. An operational solution should be a privilege of a site with enough experience. Some questions about therapeutic procedures have not yet been answered and provide space for further examination. In the global view, there is ambiguity in the operational versus conservative treatment of Gartland type-II fractures, advantages and disadvantages of fixation with crossed Ki-wires versus lateral approach, and the management of lateral and management of blood supply disorders in the sense of pink-pulseless limb. More attention would also be given to the evaluation of the effect of rehabilitation.
Sources
1. ABDULLAH, E., MELIH, G. Delayed surgical treatment of supracondylar humerus fractures in children using a medial approach. J Child Orthop. 2008, 2, 21–27. doi: 10.1007/s11832-007-0072-y
2. ABZUG, JM et al. Pediatric Elbow Fractures, Springer International Publishing AG. 2018, pp 19-60. https://doi.org/10.1007/978-3-319-68004-0_4
3. ABZUG, JM, KOZIN, SH. Fractures of the Pediatric Elbow I. Supracondylar Humerus, Lateral Condyle, Transphyseal Distal Humerus and Capitellum Fractures. In Herman MJ, Horn BD (eds): Contemporary Surgical Management of Fractures & Complications. Vol. 3 Pediatrics. Jaypee, 2014. Chapter 3, pp 35–69.
4. ARIYAWATKUL, T. et al. The necessity of fixation in Gartland type 2 supracondylar fracture of the distal humerus in children (modified Gartland type 2A and 2B). J Pediatr Orthop B. 2016, 25,159–164.
5. DELNIOTIS, I., DELNIOTIS, A. et al. Management of the Pediatric Pulseless Supracondylar Humeral Fracture: A Systematic Review and Comparison study of „watchful expectancy strategy" versus surgical exploration of the brachial artery. Annals of Vascular Surgery. 2018, doi:10.1016/j.avsg.2018.05.045.
6. CHEN, TL. Stiffness of various pin configurations for pediatric supracondylar humeral fracture: a systematic review on biomechanical studies. J Pediatr Orthop B. 2015, 24, 389–399. doi: 10.1097/BPB.0000000000000196.
7. EMERY, KH, ZINGULA, SN, ANTON, CG, et al. Pediatric elbow fractures: a new angle on an old topic. Pediatr Radiol. 2016, 46, 61–6 6. doi: 10.1007/ s00247-015-3439-0.
8. FARROW, L. et al. Early versus delayed surgery for paediatric supracondylar humerus fractures in the absence of vascular compromise: a systematic review and meta-analysis. Bone Joint J. 2018, 12, 1535–1541.
9. GARTLAND, JJ. Management of supracondylar fractures of the humerus in children. Surg Gynecol Obstet. 1959, 109, 145–154.
10. HAVRÁNEK, P. et al. Poranění lokte. V: Havránek, P. ed. Dětské zlomeniny. 2. doplněné a přepracované vydání. Praha : Galén, 2013. 112–1 64.
11. HERMAN, MJ, BOARDMAN, MJ et al. Relationship of the anterior humeral line to the capitellar ossific nucleus: variability with age. J Bone Joint Surg Am. 2009, 91, 2188–2193.
12. INCHLEY, J. et al. Adolescent obesity and related behaviours: trends and inequalities in the WHO European Region, 2002–2014. Observations from the Health Behaviour in School-aged Children (HBSC) WHO collaborative cross-national study. Copenhagen, WHO Regional Office for Europe, 2017.
13. LEICHT, KK, KAY, RM, FEMINO, JD et al. Treatment of multidirectionally unstable supracondylar humeral fractures in children. A modified Gartland type-IV fracture. J Bone Joint Surg Am. 2006, 88, 980–985.
14. NA, Y., BAI, R. et al. Comparison of lateral entry with crossed entry pinning for pediatric supracondylar humeral fractures: a meta-analysis. J Orthop Surg Res. 2018, 3, 68. doi: 10.1186/s13018-018-0768-3.
15. O’HARA, LJ, BARLOW, JW, CLARKE, NM. Displaced supracondylar fractures of the humerus in children. Audit changes practice. J Bone Joint Surg Br. 2000, 82, 204–210.
16. PRABHAKAR, P. et al. Delaying Surgery in Type III Supracondylar Humerus Fractures Does Not Lead to Longer Surgical Times or More Difficult Reduction. J Orthop Trauma. 2019, 33, 285–290.
17. SCHMALE, GA, GREGORY, A. et al. Lack of Benefit of Physical Therapy on Function Following Supracondylar Humeral Fracture: A Randomized Controlled Trial. Journal of bone and joint surgery. 2014, 96, 944–950. doi:10.2106/JBJS.L.01696
18. SILVA, M. Biomechanical testing of pin configurations in supracondylar humeral fractures: the effect of medial column comminution. J Orthop Trauma. 2013, 27, 275–280. doi: 10.1097/BOT.0b013e31826fc05e.
19. SKAGGS, DL, Flynn, JM. Supracondylar fractures of the distal humerus. In: Kasser JR, Beaty JH, editors. Rockwood and Wilkins’ fractures in children. Philadelphia : Lipincott Williams and Wilkins; 2010. p. 487–532.
20. ŠTICHAUER, R., Preis, J. et al. Poranění periferních nervů při suprakondylických zlomeninách humeru u dětí. Cesk Slov Neurol. 2017, 80, 440–444.
21. VAQUERDO-PICARDO, A. et al. Management of supracondylar fractures of the humerus in children: EFORT. Open Rev. 2018, 3, 526–540. DOI: 10.1302/2058-5241.3.170049
Labels
Surgery Traumatology Trauma surgery
Article was published inTrauma Surgery

2020 Issue 2
Most read in this issue- Supracondylar Fractures of Distal Humerus in Children – Results of Operative Treatment
- Splint rib osteosynthesis: our experience
- Axillary artery injury in low-energy shoulder injury
- Nekrolog Doc. MUDr. František Vyhnánek, CSc.
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career

