-
Medical journals
- Career
Analysis of the results of radiotherapy and chemoradiotherapy on the background of immunotherapy of patients with cancer of the oral cavity and oropharynx
Authors: H. A. Hirna
Authors‘ workplace: Ivano-Frankivsk National ; Medical University, Ivano-Frankivsk, Ukraine ; Department of Oncology and Department of Dentistry, Educational and Scientifi c Institute of Postgraduate Education
Published in: Klin Onkol 2022; 35(3): 222-231
Category: Original Articles
doi: https://doi.org/10.48095/ccko2022222Overview
Background: Advances in medicine, especially in the field of immunology in oncology, contribute to the development of new ways and methods of treating cancer of the oral cavity and oropharynx. Preclinical and clinical studies of cytokine and dendritic cell therapy, blockade of immune checkpoints, T cell uptake, treatment with monoclonal antibodies and peptide vaccines are performed. Some of these immunotherapeutic drugs are introduced into medical practice. Changes in the immune system of patients with cancer of the oral cavity and oropharynx justify the feasibility of further targeted research of new immunotherapeutic effects on malignant tumors. Materials and methods: The article represents the data of the analysis of antitumor immunity in 61 patients with cancer of the oral cavity and oropharynx who received (chemo) radiotherapy against the background of immunotherapy with the immune agent containing alpha/beta-defensins, and compares laboratory indices with clinical observation of tumor regression in patients. The influence of the immune agent containing alpha/beta-defensins was determined by analyzing the changes in the absolute and relative numbers of lymphocytes, the number of CD3+ T cells, natural killers (NK) and natural killer T cells (NKT cells). Results: The preparation containing alpha/beta-defensins has been found to enhance cytostatic antitumor effect of (chemo) radiotherapy, having a dose-dependent and cytoprotective effects considering NK cells, so the immune response to the tumor development is enhanced with the use of this agent. The data of laboratory examination of immune status correspond to the direct results of tumor regression in patients with cancer of the oral cavity and oropharynx. Clinically higher regression indices are in patients receiving radiotherapy with immunotherapy at doses of 40 and 60 mg. Conclusion: We confirmed the antitumor efficacy of the immunomodulatory agent containing alpha/beta-defensins in the treatment of patients with squamous cell carcinoma of the oral cavity and oropharynx and the reasonability of its use on the clinic.
Keywords:
oral cavity – immunotherapy – Oropharynx – cancer – regression
Introduction
In 2020, the WHO registered 377,713 cases of oral cancer, with a specific weight of 4.2 and ranking the 17th place among all oncopathologies. In Ukraine, this type of cancer is on the 19th place with an incidence of 3,422 cases and a specific weight of 4.5 [1].
The index of incidence of oropharyngeal cancer in the world is 98,412 (specific weight 1.1), and in Ukraine, this index is 1,593 (specific weight 2.2). In terms of prevalence, this disease ranks the 25th place in the world; in Ukraine, it ranks the 24th place [1].
The mortality from oral cancer is 177,757 in the world and 1,806 in Ukraine. Similarly, the mortality from oropharyngeal cancer is 48,143 and 876, respectively [1].
The abovementioned data show that in Ukraine there are high rates of morbidity and mortality from cancer of the oral cavity and oropharynx, so the inclusion of the latest methods of influence into the scheme of special therapy is relevant and necessary to improve the treatment and reduce the mortality.
Today, taking into account the new knowledge about immune defects and mechanisms of the immune system in the carcinogenesis of patients with cancer of the oral cavity and oropharynx, it is advisable to use immunotherapeutic methods of influence in the traditional treatment of patients [2].
Using the method of proteolysis of proteins of animal origin, scientists of the Research and Production Enterprise in Kyiv have obtained an immunopreparation – a complex of proteins and free aminoacids, more precisely, alpha - and beta-defensins [3,4]. This immune agent has antitumor properties, having been already used in the treatment of breast cancer [5] and lymphoma [6,7]. Previous studies have shown that it enhances the cytotoxic effect of macrophages against tumor cells and increases the number of T cells. A preparation containing alpha/beta-defensins has a direct as well as indirect effects on the patient’s immunity through the neuroendocrine system. It has also been used as an adjunct medicine to the special treatment to reduce the toxicity of (chemo) radiotherapy, and to accelerate recovery processes. It facilitates the increase of the level of serum interferon g, normalizes serum TNF-a (which acts on mast cells), affects inflammatory mediators (inhibits the production of pro-inflammatory cytokines – IL-4) and reduces sensitization of the organism to foreign proteins [3,4].
However, a preparation containing alpha/beta-defensins has not been used in any treatment of patients with cancer of the oral cavity and oropharynx, and the abovementioned inherent antitumor effects prompted us to study its effects in the treatment of patients with oropharyngeal cancer.
The aim of the study was an analysis of the antitumor efficacy of the immune agent containing alpha/beta-defensins in patients with cancer of the oral cavity and oropharynx according to clinical and laboratory tests.
Materials and methods
We have performed radiotherapy or chemoradiotherapy in 101 patients with squamous cell carcinoma of the oral cavity and oropharynx at the 1st stage of special treatment on the basis of the Municipal Non-Profit Enterprise “Precarpathian Clinical Oncology Center of Ivano-Frankivsk Regional Council”. Remote gamma therapy was performed using a cobalt-60 device according to the scheme: a single radiation dose of 2–2.5 Gy to the total radiation dose of 36–40 Gy. Chemoradiotherapy consisted of radiotherapy and chemotherapeutic potentiation with cisplatin through a catheterized superficial temporal or external carotid artery on one or both sides. Cisplatin infusion was performed intraarterially from the date of radiotherapy at a dose of 20 mg/m2 for 5 days [8]. To increase the effectiveness of antitumor treatment, additional immunotherapy using the immune agent containing alpha/beta-defensins was performed, according to two schemes of its administration. The first scheme meant intramuscular administration of 2.0 mL twice a day for 5 days, starting 2 days before the initiation of special treatment, and 2.0 mL once a day (total dose (TD) 40 mg) for the next 10 days. The second scheme of the introduction of the immune agent containing alpha/beta-defensins meant increasing the intramuscular dose to 2.0 mL twice a day for 10 days, starting 2 days before the beginning of special treatment, and 2.0 mL once a day for the next 10 days (TD 60 mg).
Depending on the method of treatment, patients were divided into groups: Group I (RT-IT) consisting of 25 patients who received radiotherapy and immunotherapy with preparation containing alpha/beta-defensins (40 mg); Group II (CT/RT-IT) consisting of 20 patients who received chemoradiotherapy and immunotherapy; Group III (RT-2IT) consisting of 16 patients who received gamma therapy against the background of immunotherapy in the increased doses (60 mg); Group IV (RT) consisting of 20 patients who received radiotherapy; Group V (CT/RT) consisting of 20 patients treated with chemoradiotherapy without immunotherapy. Groups IV and V were the comparison groups. All patients were acquainted with the treatment plan, which was certified by signing a written informed consent, following the principles of the Declaration of Helsinki. The Ethics Commission of Ivano-Frankivsk National Medical University approved the research protocol (protocol № 94/17, dated 16. 11. 2017).
Among all patients, there were 88 (87.1%) men and 13 (12.9%) women. Fifty-six (55.4%) patients were of working age (up to 60 years) and 45 (44.6%) patients were older than 60. The age range of the patients was 33–85 years.
The study included the highest number of patients with oropharyngeal cancer – 36 (35.6%), followed by 22 (21.8%) patients with tongue cancer, and with 16 (15.8%) and 12 (11.8%) patients with the cancer of mucous membrane of the lateral and the frontal parts of the oral cavity, respectively. The analysis of patients depending on the stage is as follows: most patients were in stage III – 49 (48.5%); there were 39 patients in stage IVa, 8 (7.9%) in stage II, 4 (3.9%) in stage IVb, and 1 (1%) in stage I. As it can be seen from Tab. 1, the distribution of patients depending on the degree of histological differentiation was heterogeneous. Squamous cell carcinoma G1 was seen in 31 (30.7%) patients, and G2 in 2 (51.5%) patients, who were the largest part of the population. The least part consisted of 18 (17.8%) patients who had squamous cell carcinoma G3. Among all patients, most of them, i.e. 65 (64.4%), had endophytic tumor growth, the smallest part of them consisted of 8 (7.9%) patients with an exophytic type and 28 (27.7%) patients had a mesophytic type.
1. Distribution of patients of all groups according to the localization, growth form, histological differentiation and stage of the tumor. 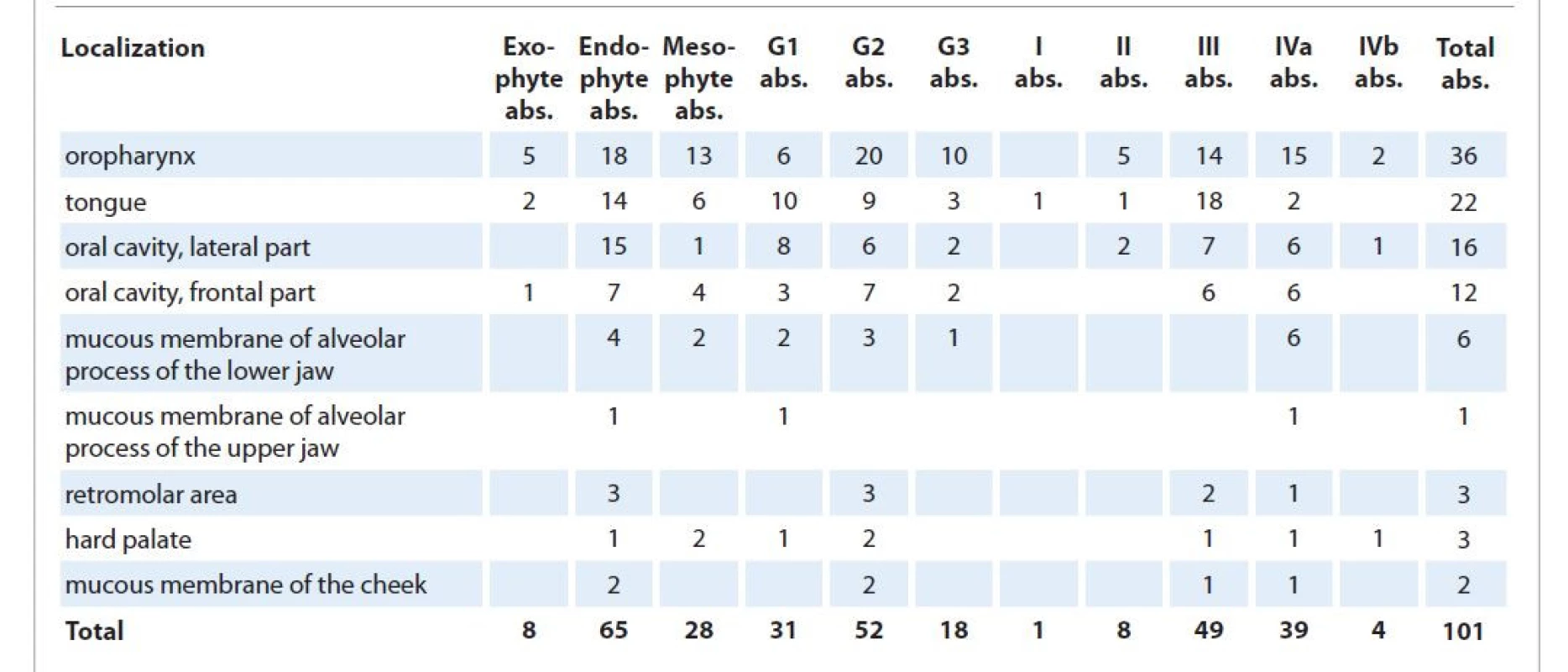
abs. – absolute number Analyzing the treatment in groups, in Group I there were 23 (92%) patients who received 44–38 Gy at the 1st stage of treatment and 1 (4%) patient who received 34 and 26 Gy on the background of immunotherapy with the immune agent containing alpha/beta-defensins (40 mg). In Group II, 19 (95%) patients received 40–36 Gy and 1 (5%) patient received 20 Gy. Regional intra-arterial chemotherapeutic potentiation was performed with cisplatin; the total dose in each patient was determined individually in the range 100–190 mg. Immunotherapy with the agent containing alpha/beta-defensins (40 mg) was also performed. Among the patients of Group III, 15 (93.7%) patients received the planned 36–44 Gy and 1 (6.3%) patient received 32 Gy, as well as immunotherapy with the agent containing alpha/beta-defensins in a higher dose (60 mg). The majority, i.e. 18 (90%) patients, of Group IV received 36–40 Gy and 1 (5%) patient received 22 and 20 Gy. There were 19 (95%) patients of Group V at the 1st stage of special treatment who received 40–36 Gy and 1 (5%) patient received 34 Gy. All patients received a total of 100–210 mg of chemotherapeutic potentiation with cisplatin according to the scheme.
According to clinical examination, laboratory diagnostics, ultrasound examination, computed tomography and magnetic resonance imaging, the size of the tumor and metastatic lymph nodes were assessed and compared with the initial data in patients who received special treatment with and without immunotherapy. Tumor regression was recorded halfway through treatment, at the end and before the 2nd stage of special treatment (3–4 weeks after the 1st stage).
Laboratory studies have allowed us to assess the antitumor immune response of the patient under the influence of immune agent alpha/beta-defensins. We have studied the systemic cellular antitumor immunity in the blood of patients: the number of CD3+ (T cells); CD3–CD16+CD56+ (natural killers – NK cells); CD3+CD16+CD56+ (natural killer T cells – NKT cells) using a set of monoclonal antibodies CD3-FITC/CD (16+CD56) with a single and triple label to CD markers of lymphocytes produced by IOTest. Cell identification was performed by indirect immunofluorescence, and cell counting was performed using an Epics XL (USA) laser flow cytofluorimeter based on the laboratory of immunology and molecular biology of the O. O. Bohomolets Scientific-Research Institute of Experimental and Clinical Medicine of the National Medical University. Laboratory studies as well as regression observations were performed before the treatment and after the completion of immunotherapy (at a dose of 20 Gy).
Statistical analysis of the results was performed using the IBM SPSS Statistics 23. The verification of the distribution was performed using the Shapiro-Wilk test. Most parameters did not reflect the normal distribution, so there were used nonparametric criteria: Kruskal-Wallis test and Dunn or Mann-Whitney tests for pairwise comparison, taking into account the Bonferroni correction. The differences in the groups were given in the form of P indicating the level of significance. It was believed that the data differ in P < 0.05. The median values were given to describe the data in the groups. The diagrams were provided in the form of columns with indications (95% CI).
Results and discussion
Comparative dynamics of tumor regression between patients of all groups on average at 20 Gy shows different data. The average rates of tumor regression were as follows: Group I – 37.60% (±2.83), Group II – 28.25% (±2.39), Group III – 33.44% (±2.69). In the comparison groups, the average rates of tumor regression were as follows: Group IV – 20% (±2.99) and Group V – 24.50% (±1.95). At this period of treatment according to average rates of tumor regression, the best results were in Groups I and III; the worst results were in Group IV.
According to Graph 1, it can be noted that in Groups I, II and III, there were high regression rates in the range of more than 25–50%, a small number of patients of the same groups, 20%, 5% and 6%, have high regression rates ≥ 50%. Among the control groups, the worst results were in the majority of patients from Group IV (85%), who had tumor regression up to 25%. Statistically significant results are between Groups I and IV, and II and IV (P < 0.05).
Graph 1. Comparative dynamics of tumor regression in patients of all groups with 20 Gy of (chemo)radiotherapy. 
After the treatment, tumor regression was > 50% in 40% of patients in Group I, and 63% in Groups II and III. Also, only in these groups receiving special treatment and immunotherapy, there was tumor regression more than 75% (Graph 2).
Graph 2. Comparative dynamics of tumor regression in patients of all groups who completed the 1st stage of (chemo)radiotherapy. 
The average values of tumor regression are 51.0% (±3.82) in Group I, 48.16% (±2.92) in Group II, 53.13% (±3.38) in Group III, 35.50% (±3.28) in Group IV and 42.5% (±3.0) in Group V. According to these data, reliable indicators of tumor regression are between Groups I and IV, II and IV, I and V (P < 0.01). The best results are in the group having received radiotherapy and immunotherapy in a higher dose (60 mg), although the average results of tumor regression differ slightly between Groups I, II and III. The results of Groups IV and V differ significantly in comparison and the lowest average index is in Group IV having received only radiotherapy.
Tumor regression was also determined in patients of all groups before the 2nd stage of treatment. Graph 3 shows high regression rates, more than 75% in Group I as well as in Group II. It should be noted that in Group I there were 2 patients and in Group III 3 patients with 100% regression of the tumor before the 2nd stage of treatment, and 1 patient in each of Groups IV and V.
Graph 3. Comparative dynamics of tumor regression in patients of all groups before the 2nd stage of special treatment. 
The average value of tumor regression was 74.05% (±4.32) in Group I, 63.67 (±4.04) in Group II and 71.25% (±4.27) in Group III. In the comparison groups, the average regression rates are slightly lower: 54.71% (±5.01) in Group IV and 58.42 (±4.46) in Group V. The data are reliable between Groups I and II, I and IV, I and V (P < 0.01).
Clinical observations of the antitumor effect of treatment in the laboratory were reflected in the following indicators of the antitumor part of immune system. Studies of the absolute and relative number of lymphocytes in patients with cancer of the oral cavity and oropharynx confirmed the immunosuppressive effect of radiotherapy and chemoradiotherapy. However, in Groups I, II and III, in which immunotherapy was used, their decrease was greater than in Groups IV and V (P < 0.05). In Group III, the decrease in the relative and absolute number of lymphocytes was more pronounced than in Group I. That is, we can talk about the increase of the effect of immunosuppressive methods of treatment under the influence of immune agent alpha/beta-defensins – the so-called adjuvant effect and the effect of deeper lymphocytopenia and dose-dependent influence of preparation alpha/beta-defensins (Graphs 4A, B).
Graph 4. Distribution of the absolute number of lymphocytes (A) and the relative number of lymphocytes (B) in patients of the study groups before and after the treatment. 
Decreased indicators of the absolute number of CD3+ T cells in the blood in Groups I and III show changes, i.e. the presence of the effect of the increase of cytostatic antitumor treatment with preparation alpha/beta-defensins (P < 0.05). It may be associated with more pronounced anticancer effect of both chemoradiotherapy and radiotherapy under the influence of an adjuvant, which is the preparation containing alpha/beta-defensins. There is also a dose-dependent effect – an even greater decrease in the absolute number of CD3+ T cells in the blood when using a higher dose of immunotropic agent (P < 0.05). There is a slight decrease in their indicators in the blood of patients of Group II, but the adjuvant effect of immune agent alpha/beta-defensins persists (Graph 5A).
Graph 5. Distribution of the absolute number of T-lymphocytes (A) and the relative number of T-lymphocytes (B) in patients in the study groups before and after the treatment. 
The study and comparison of the relative number of CD3+ T cells in the blood in all groups shows that it does not have such a pronounced immunosuppressive effect. The decrease in the number of cells in this subpopulation of lymphocytes in patients undergoing chemoradiotherapy with the immune agent containing alpha/beta-defensins is determined. In patients who had radiotherapy with preparation alpha/beta-defensins at a lower dose, according to laboratory studies, the immunosuppressive effect is lower and there is the disappearance of this effect with the increasing dose of preparation containing alpha/beta-defensins (Graph 5B).
Important components of the natural antitumor cytotoxic immune response are NK cells, which prevent tumor growth in the body [9]. We have studied the dynamics of changes in the indicators of NK cells in the blood of patients with cancer of the oral cavity and oropharynx of all groups. It was determined that patients who received radiotherapy with a higher dose of immune agent containing alpha/beta-defensins had the best results, in Group III, the relative number of NK cells increased significantly. Slightly less dynamics of the increase of these indicators was observed in Group I of patients who received a lower dose of immune agent containing alpha/beta-defensins and radiotherapy. In this case, the dose-dependent effect of immune agent containing alpha/beta-defensins on NK cells and the reliability of the results (P < 0.05) were observed. Patients receiving chemoradiotherapy had different results of the study of the relative number of NK cells in the blood; there was a decrease after treatment (immunotherapy) and their lowest rates were in Group V. Comparing the data of Groups V and II, there is a smaller decrease in NK cells (P < 0.05) in Group II, where there was immunotherapy, which can be explained by the positive effect of the preparation containing alpha/beta-defensins (Graph 6A).
Graph 6. Distribution of the relative number of natural killers (A) and the absolute number of blood natural killers (B) in patients of the study groups before and after the treatment. 
Processing of the results of the absolute number of NK cells in the blood, which are reduced in all groups of patients, testify to the immunosuppressive effect of (chemo) radiotherapy. In patients of Group II (with immunotherapy) the number of these cells is not as reduced as in Group V, which can be attributed to the effect of immunotherapy. In patients of Groups I and III, who received only radiotherapy and the preparation containing alpha/beta-defensins, its effect was not observed. In general, the analysis of lymphocyte counts and the absolute number of NK cells reveals that patients receiving special treatment against the background of immunotherapy with the immune agent containing alpha/beta-defensins have a certain adjustment of the subpopulation composition of blood lymphocytes (Graph 6B).
Cytostatic methods of treatment reduce the effectiveness of the body’s immune responses. Our study of the relative and absolute number of NK cells in the blood of patients with cancer of the oral cavity and oropharynx confirms this fact. It was also found that the immune agent containing alpha/beta-defensins has a cytoprotective effect on NK-cells, which enhance the patient’s antitumor resistance and provide an immune response to tumor development.
Indicators of the relative number of NKT cells in the blood of patients with cancer of the oral cavity and oropharynx do not show the effectiveness of immunotherapy with the immune agent containing alpha/beta-defensins (Graph 7A).
Graph 7. Distribution of the relative number of natural killer T-lymphocytes (A) and the absolute number of natural killer T-lymphocytes (B) in the blood of patients in the study groups before and after the treatment. 
The absolute number of NKT cells in the blood of patients (Graph 7B) who received radiotherapy and immunotherapy decreased with a dose-dependent tendency: the most profound deficiency of these cells was in patients of Group III, where a higher dose of immunotropic agent containing alpha/beta-defensins was used (P < 0.05). The difference in the absolute number of NKT cells in the blood of patients in Groups I and III corresponds to the results of the analysis of the absolute number of CD3+ T cells in the blood in the observation groups. Therefore, the inclusion of immunotherapy with the immune agent containing alpha/beta-defensins enhances the immunosuppressive effect of radiotherapy on NKT cells, as it was noted for CD3+ T cells.
Conclusions
1. Clinical observations of the effectiveness of the treatment show better results (higher rates of tumor regression) in groups of patients who received radiotherapy with immunotherapy.
2. There is no significant difference between the groups of patients who received different doses of immunotherapy according to clinical observations. The average data of tumor regression between Groups I and III differ slightly, but they are higher than in groups of patients who did not have immunotherapeutic effects.
3. At the laboratory level, the positive antitumor effect of the immune agent containing alpha/beta-defensins has been confirmed in the enhancement of radiotherapy and chemoradiotherapy, i.e. it has an adjuvant effect that is stronger in relation to radiotherapy and is dose-dependent.
4. The immunomodulatory effect of the immune agent containing alpha/beta-defensins is revealed – it promotes reorganization of subpopulation composition of blood lymphocytes.
5. There was observed its cytoprotective effect on NK cells, i.e. the effect on the preservation of the cellular cytotoxic immune response against the tumor during (chemo) radiotherapy.
6. The best clinical results of treatment in the groups of patients who received immunotherapy correspond to the favorable profile of antitumor immune part and indicate the effectiveness of immunotherapy in combination with radiotherapy.
Prospects for further research
Evaluation of local antitumor immunity of patients with cancer of the oral cavity and oropharynx and antitumor efficacy of the immune agent containing alpha/beta-defensins, which was used during (chemo) radiotherapy.
Acknowledgement
This work is a fragment of the scientific-research work “Clinical effectiveness of comprehensive treatment of diseases of the hard tissues of the teeth and periodontium in the population of environmentally unfavorable regions”, state registration number 0118U004 144.
The authors declare they have no potential conflicts of interest concerning drugs, products, or services used in the study.
Autoři deklarují, že v souvislosti s předmětem studie nemají žádné komerční zájmy.
The Editorial Board declares that the manuscript met the ICMJE recommendation for biomedical papers.
Redakční rada potvrzuje, že rukopis práce splnil ICMJE kritéria pro publikace zasílané do biomedicínských časopisů.Submitted/Obdrženo: 25. 9. 2021
Accepted/Přijato: 4. 11. 2021Halyna Anatoliyivna Hirna
Department of Oncology
and Department of Dentistry
Educational and Scientifi c Institute
of Postgraduate Education
Ivano-Frankivsk National Medical
University
Halytska Street 2
Ivano-Frankivsk
Ukraine
e-mail: halynagіrna@gmail.com
Sources
1. World Health Organization. International Agency for Research on Cancer: 2020. [online]. Available from: https: //gco.iarc.fr/today/online-analysis-table.
2. Raval RR, Sharabi AB, Walker AJ et al. Tumor immunology and cancer immunotherapy: summary of the 2013 SITC primer. J Immunother Cancer 2014; 2 : 14. doi: 10.1186/2051-1426-2-14.
3. Xu D, Lu W. Defensins: a double-edged sword in host immunity. Front Immunol 2020; 7 (11): 764. doi: 10.3389/ fimmu.2020.00764.
4. Zakharenko VV, Naishtetyk VI, Kudriavceva IH et al. Pharmacological properties of the drug Propes (experimental studies). [online]. Available from: http: //immunologs.com.ua/uploads/files/articles/234/4-propes-2010-151010.pdf#page=47
5. Lytvynenko АА. The role of immunocorrection in the complex treatment of breast cancer. [online]. Available from: http: //nbuv.gov.ua/UJRN/Zdzh_2012_1_12.
6. Sivkovich SA. Aspects of treatment of patients with malignant lymphomas. [online]. Available from: http: //immunologs.com.ua/uploads/files/articles/234/4 - propes-2010-151010.pdf#page=27.
7. Bullard RS, Gibson W, Bose SK et al. Functional analysis of the host defense peptide Human Beta Defensin-1: new insight into its potential role in cancer. Mol Immunol 2008; 45 (3): 839–848. doi: 10.1016/j.molimm.2006.11. 026.
8. Method of chemotherapeutic potentiation during radiation therapy of patients with oral cancer: Patent 142686 Ukraine № u201911428; stated 25. 11. 2019; published 25. 06. 2020, Biul. № 12. 3 p.
9. Maltsev DV, Hirna HА. The deficiency of natural killer cells and/or natural killer T cells as the cause of malignancies in humans. [online]. Available from: https: //www.clinicaloncology.com.ua/wp/wp-content/uploads/2018/03/666.pdf.
Labels
Paediatric clinical oncology Surgery Clinical oncology Haematology ENT (Otorhinolaryngology) General practitioner for adults Urology
Article was published inClinical Oncology

2022 Issue 3-
All articles in this issue
- Oslepení
- Changes of serum protein N-glycosylation in cancer
- New approaches in palliative systemic therapy of anal squamous cell carcinoma
- Metabolic plasticity of cancer cells
- Neurobiology of cancer – the role of cancer tissue innervation
- Direct and indirect impacts of the COVID-19 pandemic on patients with pulmonary and pleural malignancies – a retrospective analysis of patient outcomes treated at Department of Respiratory Diseases, University Hospital Brno, during the 2nd and 3rd coronavirus waves
- Meigs’ syndrome
- Informace z České onkologické společnosti
- Bone remineralization after palliative radiotherapy
- Aktuality z odborného tisku
- Prof. MUDr. Luboš Petruželka, CSc.
- Association of IL-8 -251T>A and IL-18 -607C>A polymorphisms with susceptibility to breast cancer – a meta-analysis
- Analysis of the results of radiotherapy and chemoradiotherapy on the background of immunotherapy of patients with cancer of the oral cavity and oropharynx
- Diffuse large B-cell lymphoma associated ileocecal intussusception in adulthood
- Clinical Oncology
- Journal archive
- Current issue
- Online only
- About the journal
Most read in this issue- Meigs’ syndrome
- Analysis of the results of radiotherapy and chemoradiotherapy on the background of immunotherapy of patients with cancer of the oral cavity and oropharynx
- Changes of serum protein N-glycosylation in cancer
- Metabolic plasticity of cancer cells
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career

