-
Medical journals
- Career
Functional variants of metalloproteinase MMP ‑ 1 and MMP ‑ 7 genes have no relationship to the severity of portal hypertension in patients with cirrhosis
Authors: R. Brůha 1; M. Jáchymová 2; K. Dvorak 1; J. Petrtýl 1; J. Smalcova 1; P. Urbánek 3; T. Svestka 1; L. Vítek 1,2
Authors‘ workplace: Institute of Clinical Biochemistry and Laboratory Diagnostics, 1st Faculty of Medicine, Charles University in Prague 2; Department of Internal Medicine, Central Military Hospital, Prague 3; th Department of Internal Medicine, 1st Faculty of Medicine, Charles University in Prague 14
Published in: Gastroent Hepatol 2015; 69(2): 116-120
Category: Hepatology: Original Article
doi: https://doi.org/10.14735/amgh2015116Overview
Cirrhosis is a final stage of chronic liver disease. High morbidity and mortality are mostly related to complications of portal hypertension. Remodelling of liver fibrotic tissue by matrix metalloproteinases (MMPs) is a permanent process leading to cirrhotic scar formation. The aim was to study the significance of functional metalloproteinase MMP‑ 1 and MMP‑ 7 gene variants in cirrhotic patients and their relationship to portal hypertension.
Patients and Methods:
179 patients with liver cirrhosis (mean age 55.2 ± 11.6 years) were examined for functional variants of MMP‑ 1 ( - A; rs1799750) and MMP‑ 7 (G/ A; rs17884789) genes. Measurement of hepatic venous pressure gradient, laboratory and ultrasound examination were performed in all patients. Literary data from a healthy population were used for comparison of allele frequencies with our cirrhotic patients.Results:
The frequency of rs1799750 (1G ‑ 1G 25%, 1G ‑ 2G 56%, 2G ‑ 2G 22%) genotypes in cirrhotic patients does not differ from the healthy population (p > 0.05). In MMP‑ 7 gene, one genotype (wild type GG) was found in our patients uniformly for rs17884789 variant. No relationship was found between the frequency of examined genotypes and either the severity of portal hypertension or Child ‑ Pugh or MELD score.Conclusions:
Functional variants of MMP‑ 1 and MMP‑ 7 have no relationship to portal hypertension in liver cirrhosis.Key words:
cirrhosis – fibrosis – genetic polymorphism – matrix metalloproteinase 1 – matrix metalloproteinase 7 –hypertension – portal
Liver cirrhosis is a final stage of different chronic liver diseases, associated with high morbidity and mortality. Major complications of cirrhosis such as bleeding from oesophageal varices, ascites, and hepatic encephalopathy are related to portal hypertension [1]. Fibrosis and scarring of liver parenchyma leading to cirrhosis is a continuous process controlled by many factors. With chronic liver disease the extracellular matrix undergoes a process of remodelling, leading to new collagen formation and deposition. The extracellular matrix in chronic liver disease consists of type I and type III collagen [2]. Tissue remodelling is regulated by molecular mechanisms, involving proteases, inhibitors and growth factors. The major role in extracellular matrix (ECM) degradation is played by matrix metalloproteinases (MMPs), a class of zinc and calcium ‑ dependent enzymes, and their tissue inhibitors (TIMPs) [3]. The three most relevant MMPs are gelatinase A (MMP ‑ 2), gelatinase B (MMP ‑ 9), and stromelysin (MMP ‑ 3), involved in the normal liver matrix degradation under physiological condition. In fibrotic liver there is net deposition of fibrillar matrix that is comprised predominantly of the interstitial collagens, types I and III. These triple helical molecules are relatively resistant to protease activity but are cleaved by interstitial collagenase MMP‑ 1 [4]. Another important collagenase is MMP‑ 7, which has been attributed to liver fibrosis under various pathological conditions [5,6], including cirrhosis and hepatocellular carcinoma [7].
The MMPs genes are located on chromosome 11q22 [8]. The gene for MMP‑ 1 (which degrades fibrillar collagen types I and III) carries a promoter dimorphism at position 21607, where either one (1G allele) or two (2G allele) guanines are detected. The importance of this functional variant in liver cirrhosis is not known. The single nucleotide polymorphism (SNP) in the MMP‑ 7 gene (Gly ‑ 137 3 Asp ‑ 137 [G137D]) was described to be susceptible to liver cirrhosis [9]. The relationship to portal hypertension is not known.
The aim was to study the significance of functional metalloproteinase MMP‑ 1 and MMP‑ 7 gene variants in cirrhotic patients and their relationship to portal hypertension.
Material and methods
Patients
A group of 179 patients with proven liver cirrhosis, indicated for invasive haemodynamic measurement of portal hypertension, was included in the study. Liver cirrhosis was diagnosed on the basis of biochemical tests, clinical and ultrasound findings and/ or liver biopsy, and the presence of portal hypertension diagnosed by hepatic vein catheterisation.
Hepatic vein catheterisation and a hepatic venous pressure gradient (HVPG) measurement were performed in all patients. The clinical data of patients with liver cirrhosis are given in tab. 1. The data for comparison of allele frequencies in our group of cirrhotic patients with healthy controls were obtained from literature [7,9].
1. Characteristics of patients with liver cirrhosis in the study. Tab. 1. Charakteristika pacientů s cirhózou jater zařazených do studie. 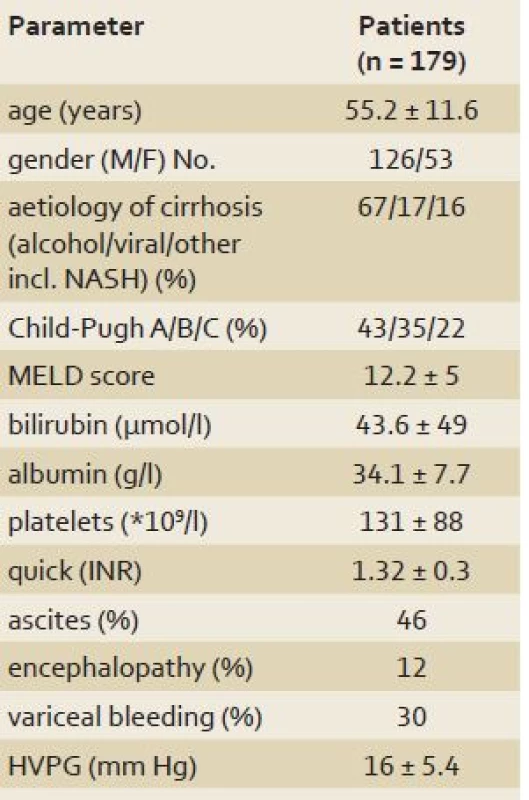
*Data expressed as mean ± SD; HVPG: hepatic venous pressure gradient. The study was approved by the local Ethics Committee, and the protocol conformed to the latest ethical guidelines of the Declaration of Helsinki. Informed consent was obtained from all subjects.
Method
Measurement of HVPG
Measurement of HVPG was performed using the classical wedged technique [10]. Shortly after overnight fasting, patients were transported to the catheterisation room in supine position. Under local anaesthesia, a 7F catheter introducer was placed in the right jugular vein using the Seldinger technique. Under fluoroscopic control, a 7F balloon ‑ tipped catheter (B. Braun Melsungen AG, Germany) was advanced into the right hepatic vein in order to measure both the free hepatic venous pressure and the wedged hepatic venous pressure. All measurements were performed in triplicate. HVPG was calculated as the difference between the wedged hepatic venous pressure and free hepatic venous pressure.
Laboratory analyses
Biochemical and haematology examinations were performed by routine techniques on automatic analysers. The severity of liver disease was evaluated by Child ‑ Pugh and MELD score.
Genotyping of the MMP
The functional variants of MMP‑ 1 ( – 1607 bp; – A; rs1799750) and MMP‑ 7 (Gly137Asp; rs17884789) genes were examined by standard PCR technique. Genomic DNA was isolated from peripheral blood leucocytes and the polymorphic sites of MMP‑ 1/ MMP‑ 7 genes were detected using both the polymerase chain reaction (PCR) and PCR restriction fragment length polymorphism technique.
Statistical methods
The data are expressed as the mean ± ± SD. Allele frequency was evaluated by the Chi ‑ square test. Either a two‑-sample t‑test or the Mann‑Whitney rank test for non‑Gaussian distributed variables was used to estimate the intergroup differences. One Way Analysis of Variance or Kruskal ‑ Wallis One Way Analysis of Variance on Ranks were used to estimate the differences between more than 2 groups. A p value of ≤ 0.05 was required for statistical significance. The statistics were computed using STATISTICA CZ v. 8 (StatSoft, Prague, Czech Republic).
Results
Characteristics of patients
One hundred and seventy nine patients were included in the study: 126 males and 53 females. No differences in the age, biochemical parameters and/ or the aetiology and stage of cirrhosis were present between both gender groups (data not shown). The clinical and laboratory parameters of all patients are given in tab. 1. Hepatocellular carcinoma developed in eight patients from our group.
Genotyping, comparison to controls and relationship to portal hypertension and liver dysfunction
The frequencies of MMP‑ 1 gene variations are presented in tab. 2. No statistical differences between the cirrhotic patients and literary controls regarding the frequencies of analysed genotypes were found. Female cirrhotic patients had lower frequency of 1G ‑ 1G genotype compared to male patients with liver cirrhosis (16% vs 25%) with borderline statistical significance (p = 0.04). No differences between clinical/ laboratory parameters were found in different genotype in cirrhotic patients (tab. 3); there were no relationships between different genotypes and either parameters of liver dysfunction, or portal hypertension. The distribution of 1G ‑ 1G, 1G ‑ 2G and 2G ‑ 2G did not differ between Child ‑ Pugh classes A, B and C. No relationship between above mentioned genotypes and MELD score was found.
2. Frequency of functional variants rs1799750 and rs17884789 in the genes for metalloproteases MMP-1 and MMP-2 in patients with liver cirrhosis. Tab. 2. Frekvence výskytu funkčních variant rs1799750 and rs17884789 genů pro metaloproteinázy MMP-1 a MMP-2 u pacientů s cirhózou jater. 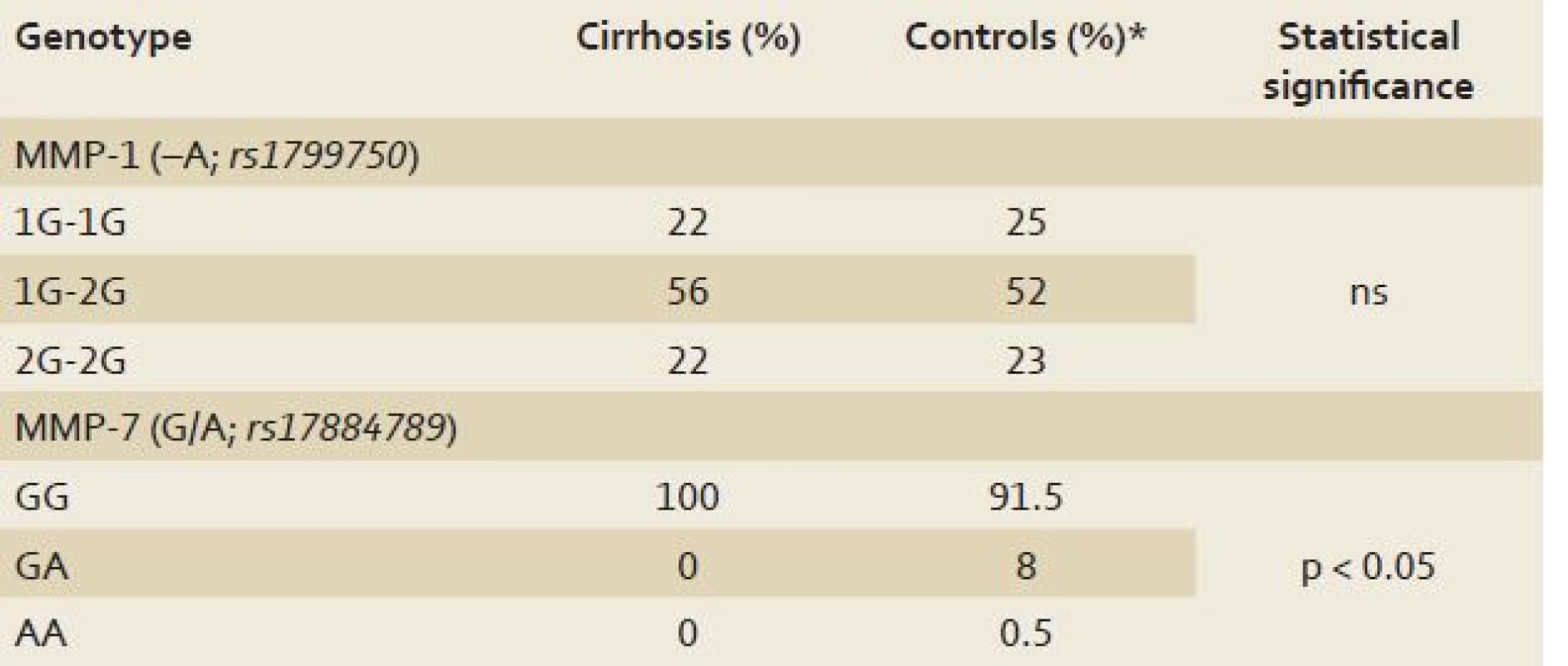
* Literary controls (7, 9); Data expressed as % of patients; ns: non-significant. 3. Clinical and laboratory parameters in patients with liver cirrhosis and different genotypes for MMP-1 (–A; rs1799750). Tab. 3. Klinické a laboratorní parametry u pacientů s cirhózou jater a různé genotypy pro MMP-1 (–A; rs1799750). 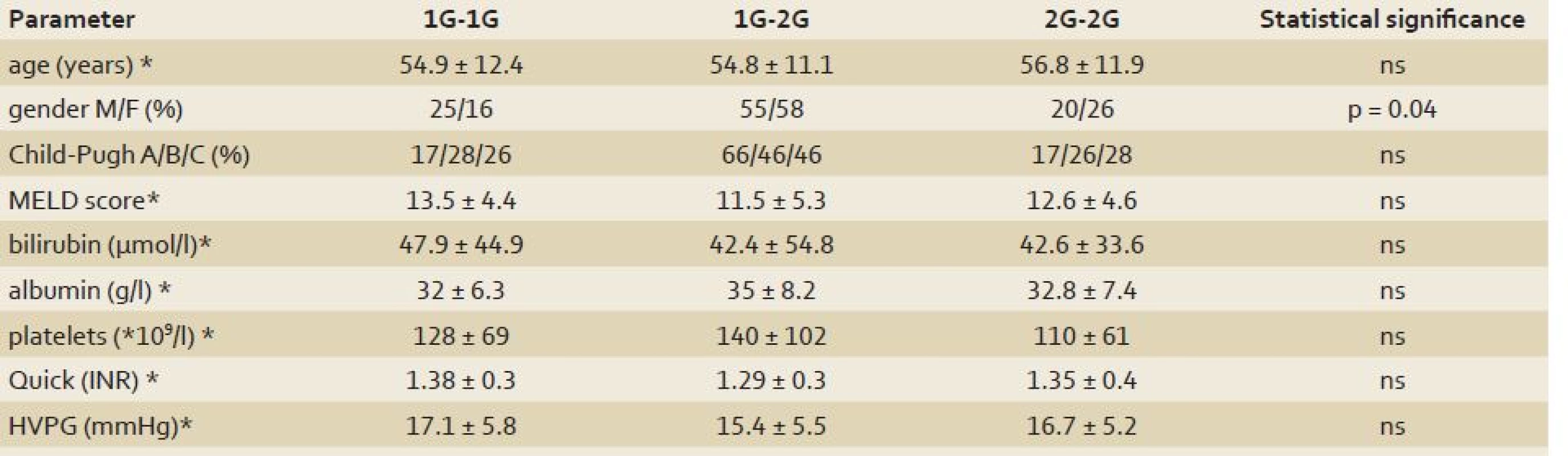
*Data expressed as mean ± SD. HVPG: hepatic venous pressure gradient. In MMP‑ 7 gene, only one genotype was found in all patients uniformly for rs17884789 variant (wild type GG).
Discussion
Liver fibrosis is a pathological process involving many cellular and molecular changes and leading to the deposition of excess matrix proteins in the extracellular space. When combined with ineffective regeneration and repair, increased distortion of the normal liver architecture results in cirrhosis. Liver fibrosis is a dynamic and bidirectional process, involving phases of progression and regression. In addition to increased matrix synthesis, the process of cirrhosis formation involves major changes in the regulation of matrix degradation.
In the extracellular space, matrix degradation occurs under physiological conditions as a consequence of the action of a family of enzymes called the matrix metalloproteinases (MMPs). These are secreted from cells into the extracellular space as proenzymes, which are then activated by a number of specific, usually cell surface‑associated cleavage mechanisms. The active enzymes are in turn inhibited by a family of tissue inhibitors of metalloproteinases (TIMP ‑ 1 to - 4). By this combination of mechanisms, extracellular matrix degradation is closely regulated, which prevents inadvertent tissue damage [4]. Specific MMPs and TIMPs are expressed on stellate cells, but the source of MMP1, which plays a crucial role in degrading the excess interstitial matrix in advanced liver disease, is still uncertain [11]. The major producers of matrix metalloproteinase ‑ 7 in the liver are the bile ductular epithelial cells, Kupffer cells and hepatocytes, as demonstrated by in situ hybridisation [5]. Huang et al. suggested that MMP‑ 7 is a major metalloprotease associated with the tissue remodelling during the progression of liver fibrosis, particularly in biliary atresia [5].
There is abundant evidence that fibrosis and even cirrhosis can be reversible under various clinical situations [12,13]. The crucial underlying mechanism of cirrhosis reversibility remains unclear. One factor that may prevent reversibility is reduced expression of enzymes that degrade matrix or sustained elevation of proteins that inhibit the function of these degradative enzymes [14].
Recently, naturally occurring sequence variation has been detected in the promoter of a number of MMP genes. These functional variants have been shown to have allele ‑ specific effects on the transcriptional activities of MMP gene promoters, and to be associated with susceptibility to many diseases like coronary heart disease, aneurysms, chronic pancreatitis and cancers. Significant association of the MMP‑ 1 - 1607 1G/ 2G (rs1799750) gene promoter polymorphism with chronic pancreatitis has been described, and it has been suggested that it could be considered a biological marker in the aetiology of chronic pancreatitis [15]. These findings indicate that variation in the MMP genes may contribute to inter ‑ individual differences in susceptibility to these common, complex diseases, likely through effects on the balance between the synthesis and degradation of extracellular matrix proteins [16]. Regarding liver diseases most important are MMP‑ 1 and MMP‑ 7. The MMP‑ 1 gene carries a promoter dimorphism at position 21607, where either one (1G allele) or two (2G allele) guanines are found. The 2G allele is associated with higher gene expression than the 1G allele [17].
All these data raises the question, whether different expression of these enzymes caused by specific gene variation could influence the course of liver fibrosis and cirrhosis. Based on our data the answer is clear – there is no association between the gene variants for MMP‑ 1 and MMP‑ 7 and liver cirrhosis, liver dysfunction or portal hypertension. This is partly in concordance with literature data, which are controversial. For example, Wiencke et al. studied Norwegian patients with primary sclerosing cholangitis and found no general associations of the MMP‑ 1 gene to liver disease [9]. Nevertheless, they described that specific alleles were associated to subsets of PSC patients with cholangiocarcinoma.
The relationship of different MMPs gene variants and carcinomas seems to be close, as MMP single‑nucleotide polymorphisms influence breast cancer behaviour and the MMP‑ 1 2G/ 2G genotype increases the risk of lymph node metastasis and predicts poor prognosis [18]. Based on meta‑analysis it seems that the polymorphism MMP1 – 1607 1G > 2G is significantly associated with a significantly increased risk of cancers like colorectal cancer and lung cancer [19]. In cirrhosis an association between MMP‑ 7 functional variants and hepatocellular carcinoma has been described [7]. Unfortunately our data do not provide any meaningful conclusion regarding the relationship between hepatocellular carcinoma and MMPs gene variants, as only a small number of patients with carcinoma has been detected (eight patients).
In our study no relationship between liver dysfunction and MMPs gene variants was found. There may be other factors involved, because in the study by Leeming et al. [20] the severity of portal hypertension and liver dysfunction correlated with extracellular matrix serological biomarkers. The authors even suggested that the combination of ECM serological markers with clinical scores may aid in the detection of the level of portal hypertension and the degree of liver dysfunction.
Hepatic mRNA expression of MMPs was studied also during the course of chronic hepatitis C, showing either steadily increasing mRNA expression with disease progression (MMP‑ 1, - 2, - 7 and - 14). The MMPs expression closely correlated to the parameters of fibrogenesis [21]. Unfortunately no data regarding the eventual gene variants are given in that paper.
Another issue is the gender difference. In our patients we found borderline differences in allele frequency for MMP‑ 1 gene variant between male and female. This observation has probably, in our opinion, no clinical relevance.
Limitation of our study is the absence of our own control population. Nevertheless the data from literature used for the comparison of cirrhotic patients and controls are highly relevant, originating from a Caucasian population [7,9].
Conclusion
In conclusion, our study demonstrates that the presence of functional variants in the gene for metalloproteases MMP‑ 1 (rs1799750) and MMP‑ 7 (rs17884789) do not carry any increased risk of liver cirrhosis. No relationship between different genotypes and portal hypertension or liver dysfunction was found. These data could probably indicate that the fibrotic process is too complicated to be affected by one single parameter.
Supported by Grant NT 12290/ 4 given by Internal Grant Agency, Czech Ministry of Health (IGA MZCR, http:/ / iga.mzcr.cz/ publicWeb/ ).
The authors declare they have no potential confl icts of interest concerning drugs, products, or services used in the study.
The Editorial Board declares that the manuscript met the ICMJE „uniform requirements" for biomedical papers.
Submitted: 11. 2. 2015
Accepted: 16. 3. 2015
Radan Bruha, MD, PhD
4th Department of Internal Medicine
General University Hospital
U Nemocnice 2, 128 08 Prague 2
bruha@cesnet.cz
Sources
1. Bosch J, García ‑ Pagán JC. Complications of cirrhosis I. Portal hypertension. J Hepatol 2000; 32 (1 Suppl): 141 – 156.
2. Guo J, Friedman SL. Hepatic fibrogenesis. Semin Liver Dis 2007; 27(4): 413 – 426.
3. Consolo M, Amoroso A, Spandidos DA et al. Matrix metalloproteinases and their inhibitors as markers of inflammation and fibrosis in chronic liver disease (Review). Int J Mol Med 2009; 24(2): 143 – 152.
4. Arthur MJ. Fibrogenesis II. Metalloproteinases and their inhibitors in liver fibrosis. Am J Physiol Gastrointest Liver Physiol 2000; 279(2): G245 – G249.
5. Huang CC, Chuang JH, Chou MH et al. Matrilysin (MMP ‑ 7) is a major matrix metalloproteinase upregulated in biliary atresia‑associated liver fibrosis. Mod Pathol 2005; 18(7): 941 – 950.
6. Amalinei C, Caruntu ID, Giusca SE et al. Matrix metalloproteinases involvement in pathologic conditions. Rom J Morphol Embryol 2010; 51(2): 215 – 228.
7. Hung TM, Chang SC, Yu WH et al. A novel nonsynonymous variant of matrix metalloproteinase ‑ 7 confers risk of liver cirrhosis. Hepatology 2009; 50(4): 1184 – 1193. doi: 10.1002/ hep.23137.
8. Formstone CJ, Byrd PJ, Ambrose HJ et al. The order and orientation of a cluster of metalloproteinase genes, stromelysin 2, collagenase, and stromelysin, together with D11S385, on chromosome 11q22 – q23. Genomics 1993; 16(1): 289 – 291.
9. Wiencke K, Louka AS, Spurkland A et al. Association of matrix metalloproteinase ‑ 1 and – 3 promoter polymorphisms with clinical subsets of Norwegian primary sclerosing cholangitis patients. J Hepatol 2004; 41(2): 209 – 214.
10. Groszmann RJ, Wongcharatrawee S. The hepatic venous pressure gradient: anything worth doing should be done right. Hepatology 2004; 39(2): 280 – 282.
11. Benyon RC, Arthur MJ. Extracellular matrix degradation and the role of hepatic stellate cells. Semin Liver Dis 2001; 21(3): 373 – 384.
12. Kweon YO, Goodman ZD, Dienstag JL et al. Decreasing fibrogenesis: an immunohistochemical study of paired liver biopsies following lamivudine therapy for chronic hepatitis B. J Hepatol 2001; 35(6): 749 – 755.
13. Dufour JF, DeLellis R, Kaplan MM. Reversibility of hepatic fibrosis in autoimmune hepatitis. Ann Intern Med 1997; 127(11): 981 – 985.
14. Iredale JP. Hepatic stellate cell behavior during resolution of liver injury. Semin Liver Dis 2001; 21(3): 427 – 436.
15. Sri Manjari K, Nallari P, Balakrishna N et al. Influence of matrix metalloproteinase ‑ 1 gene – 1607 (1G/ 2G) (rs1799750) promoter polymorphism on circulating levels of MMP ‑ 1 in chronic pancreatitis. Biochem Genet 2013; 51(7 – 8): 644 – 654. doi: 10.1007/ s10528 ‑ 013 ‑ 9594 ‑ 9.
16. Ye S. Polymorphism in matrix metalloproteinase gene promoters: implication in regulation of gene expression and susceptibility of various diseases. Matrix Biol 2000; 19(7): 623 – 629.
17. Rutter JL, Mitchell TI, Buttice G et al. A single nucleotide polymorphism in the matrix metalloproteinase ‑ 1 promoter creates an Ets binding site and augments transcription. Cancer Res 1998; 58(23): 5321 – 5325.
18. Hughes S, Agbaje O, Bowen RL et al. Matrix metalloproteinase single‑nucleotide polymorphisms and haplotypes predict breast cancer progression. Clin Cancer Res 2007; 13(22 Pt 1): 6673 – 6680.
19. Lu L, Sun Y, Li Y et al. The polymorphism MMP1 – 1607 (1G > 2G) is associated with a significantly increased risk of cancers from a meta‑analysis. Tumour Biol 2015; 36(3): 1685 – 1693.
20. Leeming DJ, Karsdal MA, Byrjalsen I et al. Novel serological neo ‑ epitope markers of extracellular matrix proteins for the detection of portal hypertension. Aliment Pharmacol Ther 2013; 38(9): 1086 – 1096. doi: 10.1111/ apt.12484.
21. Lichtinghagen R, Bahr MJ, Wehmeier M et al. Expression and coordinated regulation of matrix metalloproteinases in chronic hepatitis C and hepatitis C virus‑induced liver cirrhosis. Clin Sci (Lond) 2003; 105(3): 373 – 382.
Labels
Paediatric gastroenterology Gastroenterology and hepatology Surgery
Article was published inGastroenterology and Hepatology

2015 Issue 2-
All articles in this issue
- Noninvasive diagnostics in NAFLD
- Autochthonous case of hepatitis E virus in Slovakia
- Twenty years of experience with ERCP in the University Hospital Motol
- Esophageal motility disorders – The Chicago classification, v3.0
- Atypical picture of colon infiltration with lymphoma in a patient with chronic lymphocytic leukaemia
- Vedolizumab in the therapy of Crohn’s disease
- Novel oral anticoagulants – the advantages and drawbacks of the therapy
- Report of XXth Gastroforum
- ECCO – Inflammatory Bowel Diseases 2015
- IBD working days 2015, Hořovice
- New web platform of Gastroenterology and Hepatology journal and co-operation with the National Library of Medicine
- Informations from the editors
- Maltofer®
- Not only about hepatitis
- Therapy of chronic hepatitis C with simeprevir
- Functional variants of metalloproteinase MMP‑ 1 and MMP‑ 7 genes have no relationship to the severity of portal hypertension in patients with cirrhosis
- Gastroenterology and Hepatology
- Journal archive
- Current issue
- Online only
- About the journal
Most read in this issue- Maltofer®
- Atypical picture of colon infiltration with lymphoma in a patient with chronic lymphocytic leukaemia
- Novel oral anticoagulants – the advantages and drawbacks of the therapy
- Esophageal motility disorders – The Chicago classification, v3.0
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career

