-
Medical journals
- Career
Primary Intrabulbar Neurofibroma
Authors: A. Furdová 1; P. Babál 2
Authors‘ workplace: Klinika oftalmológie, Lekárska fakulta Univerzity Komenského a Univerzitná nemocnica, Nemocnica Ružinov, Bratislava 1; Ústav patologickej anatómie, Lekárska fakulta Univerzity Komenského, Bratislava 2
Published in: Čes. a slov. Oftal., 76, 2020, No. 2, p. 62-67
Category: Original Article
doi: https://doi.org/10.31348/2020/13Overview
Purpose: Eye globe enucleation due to other than a malignant tumor is very rare today. Solitary intraocular neurofibroma without other signs of neurofibromatosis is a rare benign tumor and few cases have been reported to date.
Material and Methods: In 10 year interval from Jan 1 2007 to Dec 31 2016 we analyzed non-malignant eye globe enucleations.
Results: Of the 49 enucleated blind eyes, each patient had visual acuity with no light perception, 34 (69.4%) were indicated for enucleation due to complications following previous postoperative surgery after trauma, 14 patients (28.6%) were due to secondary glaucoma and other complications following previous intraocular surgery, and in one patient (2%) the primary isolated intraocular neurofibroma was verified after enucleation.
Case Report: A patient with isolated intrabulbar neurofibroma has been monitored since childhood for intraocular lesion and histologically verified at adult age. At the time of enucleation, he was 25 years old, squint since childhood and was observed for hamartoma in his right eye since he was 13 years old. Due to the progression of intrabulbar lesion, loss of visual acuity (functional state - no light perception) and secondary glaucoma, the right eye globe was enucleated at adult age and histopathological examination confirmed intraocular neurofibroma in the absence of neurofibromatosis.
Conclusion: Every enucleated eye globe should be subjected to a thorough histopathological examination. Isolated intraocular neurofibromas can occur as isolated orbital or intrabulbar masses without systemic features.
Keywords:
neurofibromatosis – enucleation – eye globe – solitary intrabulbar neurofibroma
Sworn declaration
The authors of the study declare that no conflict of interest exists in the compilation, theme and subsequent publication of this professional communication, and that it is not supported by any pharmaceuticals company. The study has not been submitted to any professional journal or printed elsewhere, with the exception of congress abstracts and recommended procedures.
INTRODUCTION
In 1937, Stough described neurofibroma as a very rare case of intraocular tumour [21]. Neurofibroma is a benign tumour originating from the Schwann cells of the peripheral nervous system. It is usually linked with neurofibromatosis type 1 (NF1), with a multisystemic autosomal dominant disorder, upon which the nerve tissue generates multiple benign tumours which may cause compression of the nerves and other tissues, and thereby causes serious damage due to mechanical pressure [9]. The pathology affects the Schwann cells, as well as melanocytes and endoneural fibroblasts. The affected cells manifest biallelic inactivation of the gene NF1 in chromosome 17q, which codes protein neurofibromin [15].
Neurofibromas are described relatively frequently in the area of the head and neck [11,16,20], as well as elsewhere in the body [12–14].
In addition to its occurrence in connection with neurofibromatosis, isolated neurofibromas may also appear. Isolated intraocular neurofibroma or intraorbital neurofibroma is a very rare condition. With regard to the clinical characteristics, in differential diagnostics it is often mistaken for other benign, as well as malignant intraocular tumours [3,10]. Diagnosis of intraocular lesions with the aid of ultrasound often does not produce conclusive findings [6,7].
Neurofibromatosis type 2 (NF2) may be diagnosed by a DNA test obtained from a blood sample, but this test correctly identifies mutation only in two thirds of cases, and in rare cases neurofibromas may appear also later, following previous negative results. Patients with symptoms of NF2 are sent for magnetic resonance imaging (MRI) examination, which may confirm or exclude other benign tumours, for example in the region of the spinal cord and the brain. MRI is not routinely performed on patients with NF1, since they are asymptomatic [8].
As regards genetics, children of patients with NF2 have a 50 % chance of contracting this pathology [4].
Material and method
Within a 10-year period from 1 January 2007 to 31 December 2016 we analysed enucleated eyeballs due to causes other than malignancy.
Results
In a cohort with a total number of 49 patients, the age range was from 22 to 90 years (median 58 years). In the group of 49 enucleated eyeballs, in every patient visual acuity was without light perception, in which 34 (69.4 %) patients were indicated for enucleation due to complications following previous post-traumatic surgery, in 14 patients (28.6 %) the reason was secondary glaucoma and other complications following previous intraocular surgery, and in one patient (2 %) a primary isolated intraocular neurofibroma was verified after enucleation.
Case report of patient with isolated primary neurofibroma
In 2007, a young man was examined at the Department of Ophthalmology at the Faculty of Medicine, Comenius University and the University Hospital in Bratislava. Since the age of 13 years he had been monitored for peripapillary hamartoma. According to the documentation, the functions of both eyes were unchanged since adolescent age, according to a statement from the patient’s mother the eyeball had been unchanged in divergent position throughout childhood. The examination in 2007 confirmed visual acuity in the right of 6/24, uncorrected, in the left eye 6/6, intraocular pressure was within the norm. One year later the finding in the vitreous body was unchanged, the deposit peripapillary without haemorrhage, height of elevation according to ultrasound examination up to 6.6 mm, the patient was sent for magnetic resonance imaging (MRI), according to the result the deposit was stabilised in size and shape, without progression (Fig. 1, 2). A further follow-up examination was conducted in 2010, according to the MRI examination the size of the deposit had increased by 0.5 mm, the diameter of the lesion was unchanged, the deposit was not growing across the sclera, and was without haemorrhage. According to optical coherence tomography (OCT), macular edema had enlarged, the area of the macula was secondarily raised. Central visual acuity had decreased to hand movement in front of the eye. In 2012, according to MRI there was slight local progression of the intrabulbar tumour in the right eyeball. In 2013 there was a sudden deterioration of the condition, the patient was treated at an emergency department due to “red eye” and pain. Following local antiglaucomatous treatment, subjective pains receded, increased intraocular pressure above 30 Torr persisted. Objectively the eyeball was in divergent position, with mixed injection, presence of neovascularisation of the iris, the lens nucleus was opaque and haemorrhage was present in the vitreous cavity. According to ultrasound examination the deposit had a slightly raised elevation by 0.5 mm, with haemorrhage in the vitreous cavity. The patient was sent for a follow-up MRI examination and histologisation of the lesion was considered. In 2014, due to the functional condition of the eye – dubious light perception, and the local finding – beneath the disc of the optic nerve, following clarification of the vitreous area in both quadrants, there was a lesion of greyish-white colour, with prominence and encroachment up to the region of the macula, nasally secondary amotio, on the surface of the deposit secondary amotio, ballottement, clear subretinal fluid, at the edges exudates, minimal traces following laser coagulation. Despite local and general treatment of secondary glaucoma, pain persisted and enucleation was indicated.
1. MRI image of tumour deposit close to disc of optic nerve in 2008 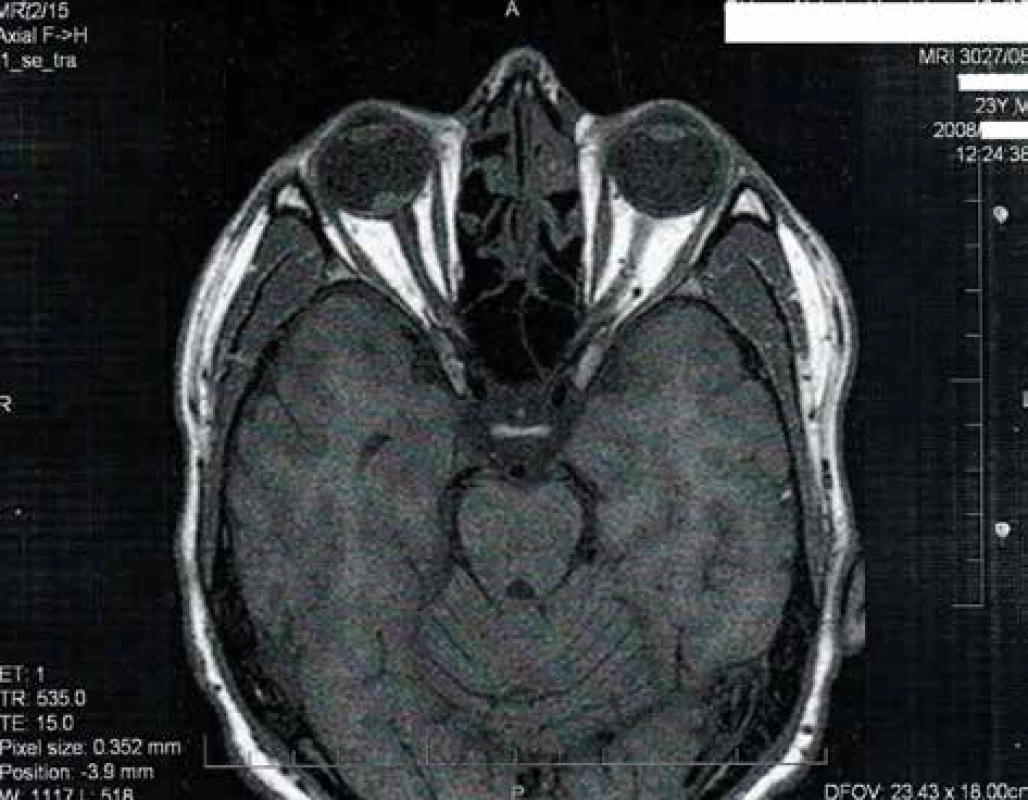
2. Ultrasound image of tumour deposit above disc of optic nerve in 2008 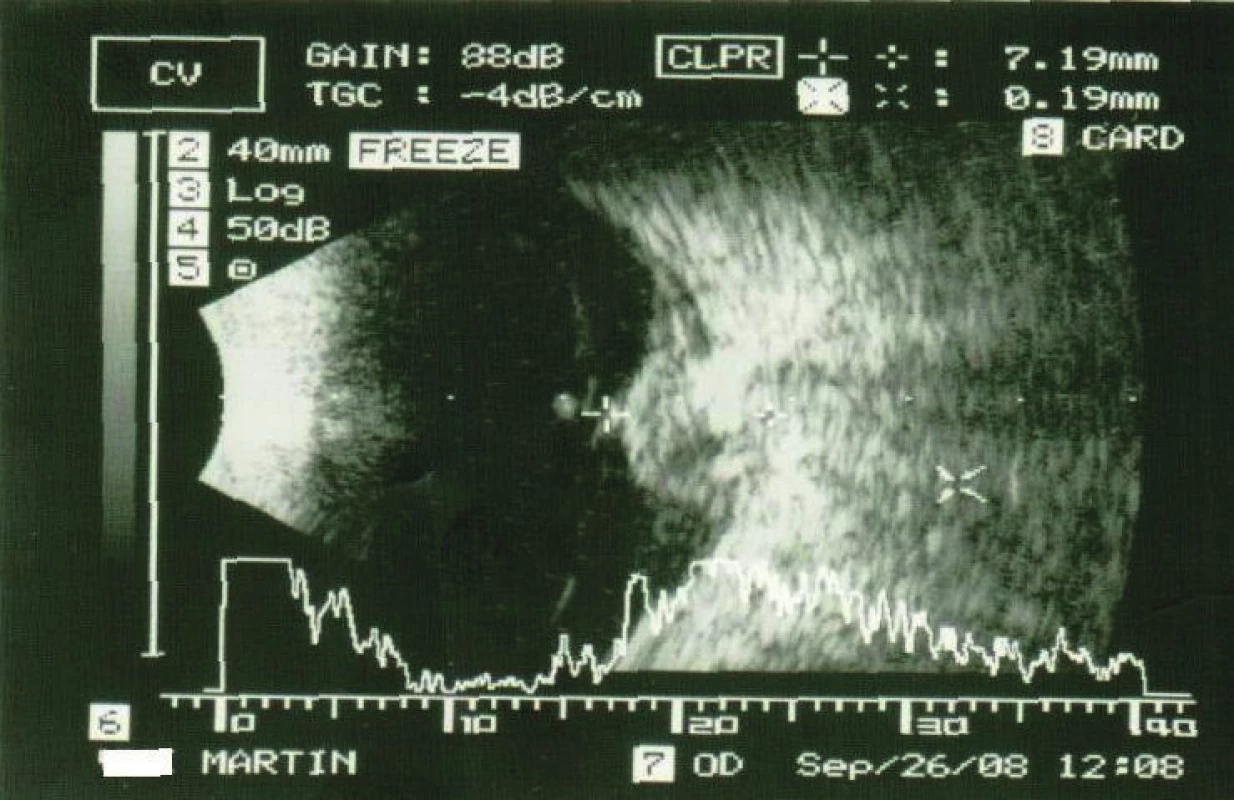
Histopathological examination – microscopic finding: tissue of eyeball, in close proximity to optic nerve disc detachment, gnarled formation is pressing on the wall formed by uncapsulated but well bordered lesion of relatively polymorphic polygonal to spindle cells, without mitotic activity, with few small deposits of older and fresher haemorrhage and deposits of ossification, at one edge a group of larger blood vessels. Tumour cells manifested pronounced positivity to vimentin and NSE, weaker to S100, isolated cells negative for GFAP, CD34, positive only in blood vessels, proliferative activity very low, almost zero, concerning neurofibroma. (Fig. 3, 4, 5, 6, 7, 8, 9).
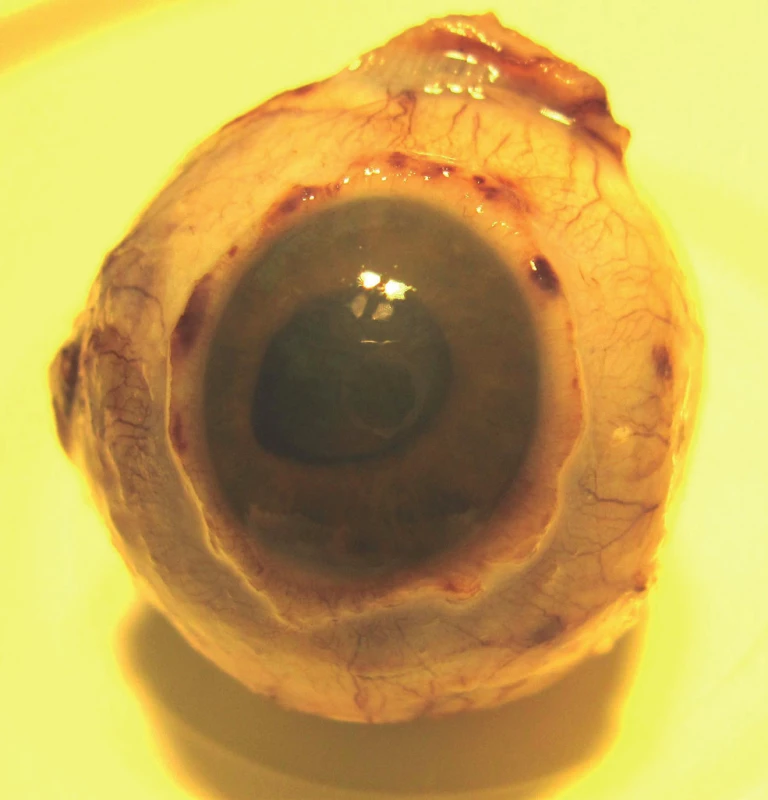
4. Eyeball after enucleation – lens turbid, secondary amotio 
5. Eyeball after enucleation – red arrow indicates tumour deposit and green arrow disc of optic nerve 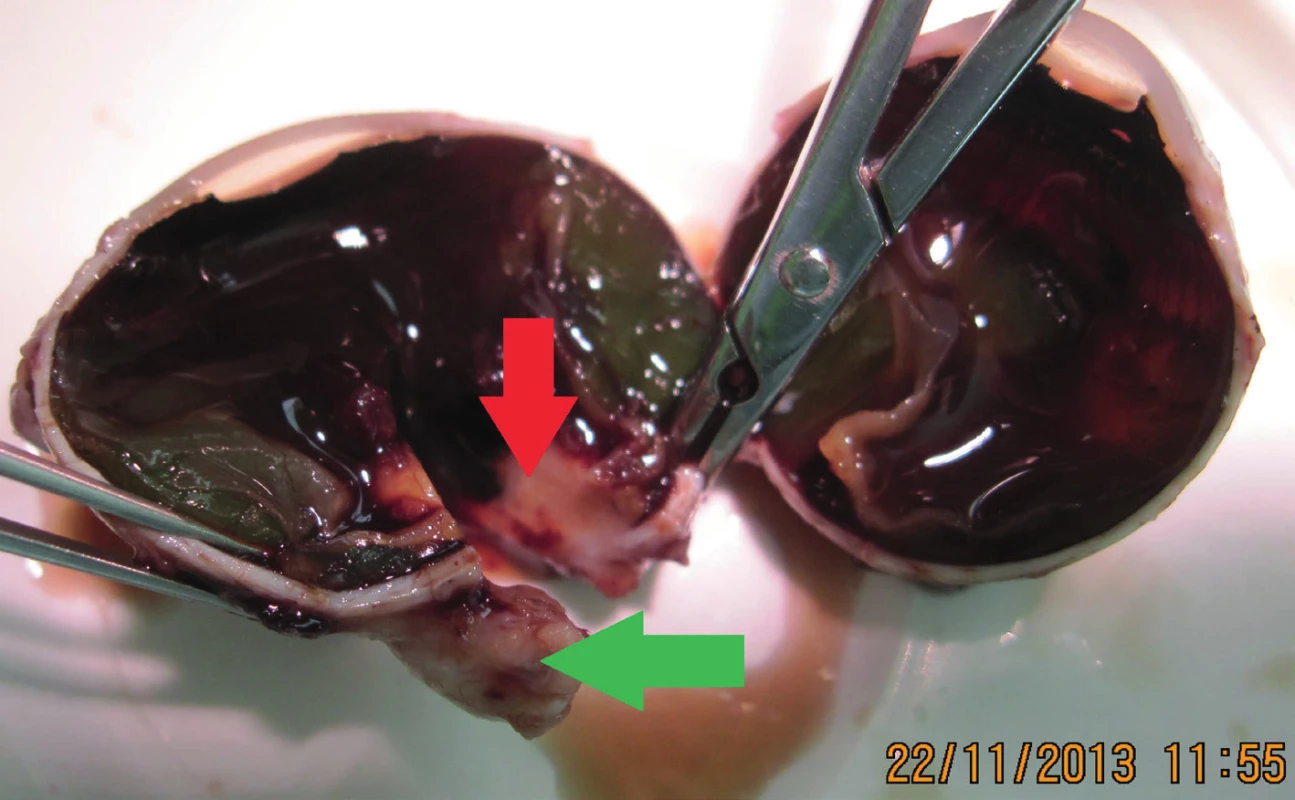
6. Eyeball after enucleation – detail of tumour deposit and secondary amotio 
7. Eyeball after enucleation – arrow indicates tumour deposit 
8. Neurofibroma growing inside eyeball (*) composed of elongated cells with slightly vacuum cytoplasm and vesicular nuclei (insertion), focally with formation of osteoid and ossification (short and long arrow); sclera (s), vitreous (v). Haematoxylin and eosin – 25x, detail – 200x 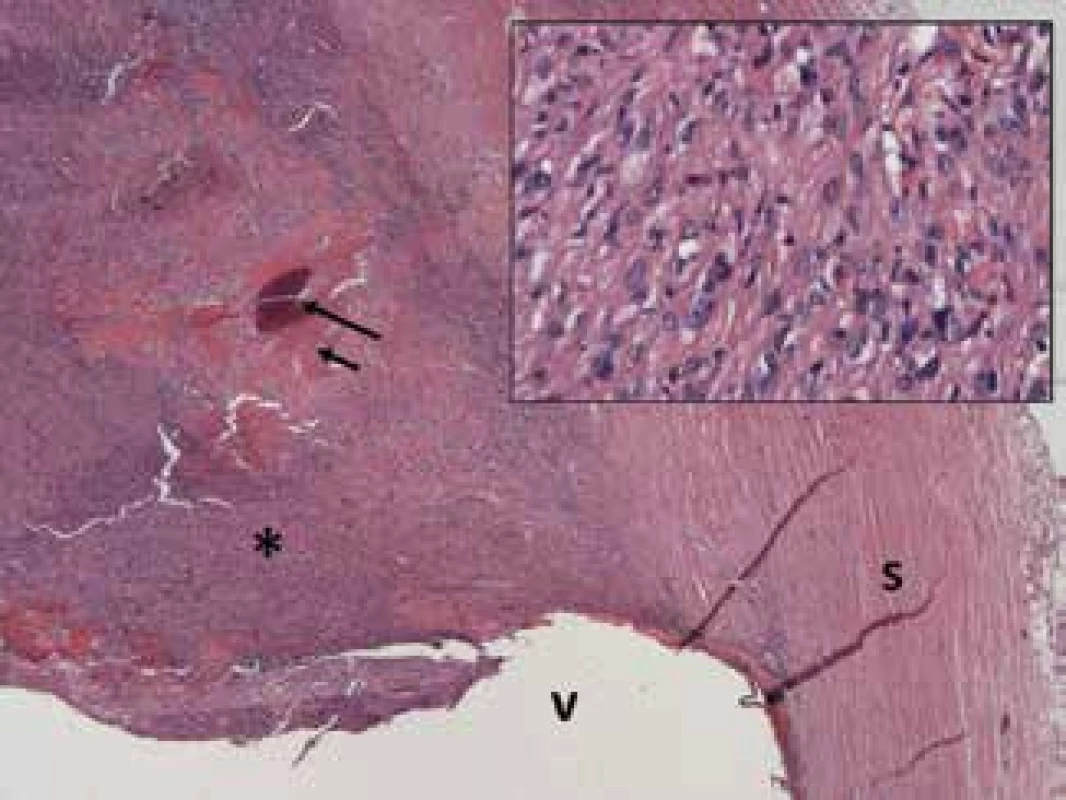
9. Neurofibroma growing inside eyeball with intensive neuron-specific enolase (NSE), vimentin and slight expression of protein S100. Haematoxylin and eosin - 100x 
After 5 years of observation since histologisation of the tumour, the young man now wears an individual prosthesis in the right eye, in 2019 still without signs of other neurofibromatous deposit. General, skin, genetic and neurological examinations excluded both NF1 and NF2. (Fig. 10, 11).
10. Clinical finding, condition after enucleation – conjunctival sac without recurrence in 2019 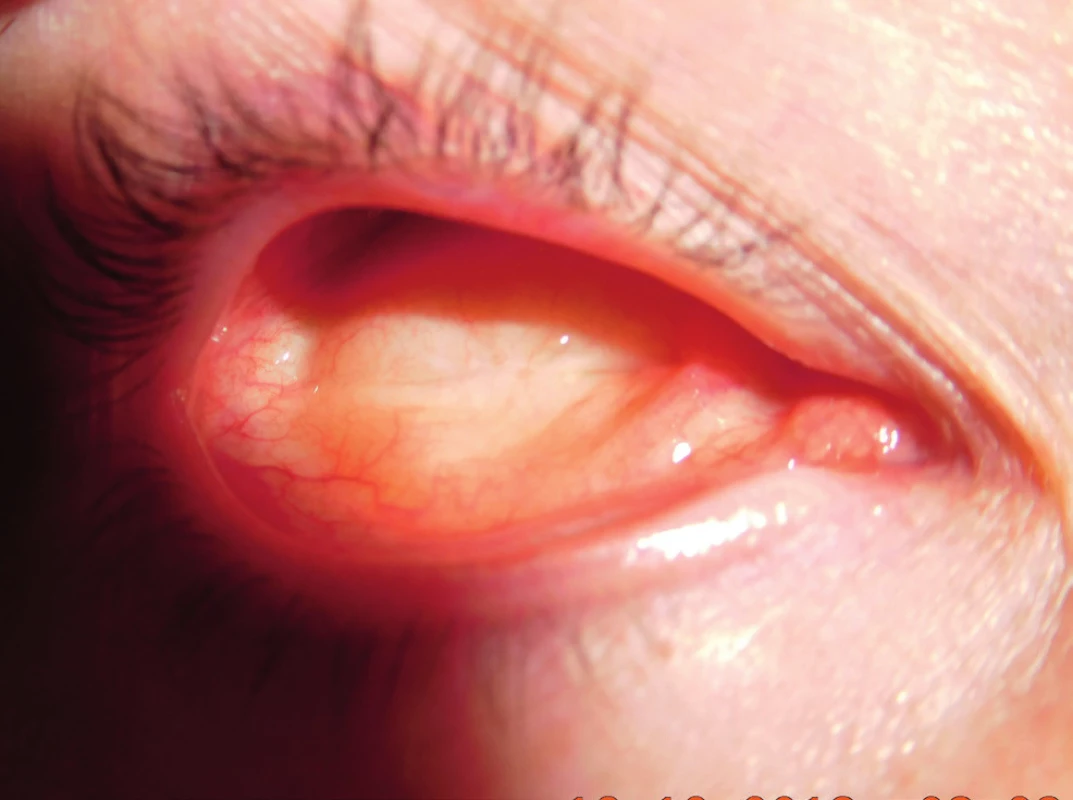
11. Macro-photo – patient with application of individual prosthesis in right eye in 2019 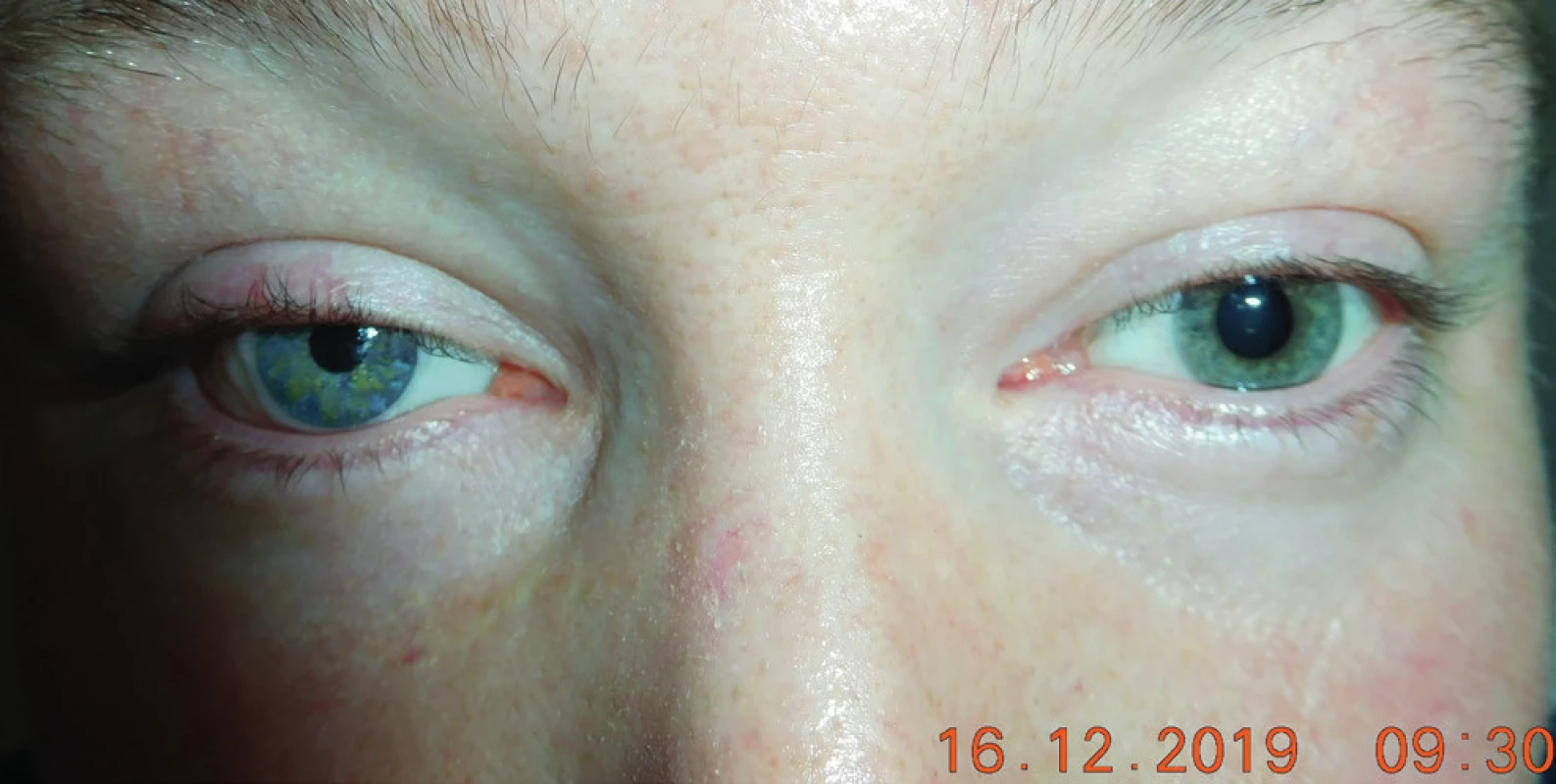
DISCUSSION
Neurofibromas are benign tumours of the nerves, characterised by proliferation of the nerve cells and Schwann cells together with intervening fibrous components. They are most often linked with neurofibromatosis 1, together with other systemic findings. Patients with NF1 are usually diagnosed in early childhood. Neurofibromas are resistant to radiotherapy, and infiltrating types are difficult to remove surgically. Neurofibromas in the region of the orbit are more common [2], but isloated cases of intraocular occurrence are rare.
It is difficult to determine the precise incidence of isolated neurofibromas, especially those of intraocular origin; however, its incidence is relatively rare.
According to a study by Rose et al. (1991), no case of isolated intraocular neurofibroma has been recorded. Very few cases of isolated orbital neurofibromas have been published. The study detected a 93 % incidence of benign neurilemmoma or neurofibroma among tumours of the sheath of the peripheral nerves [18]. A positive family anamnesis of systemic neurofibromatosis is described in one quarter of patients with solitary neurofibroma. In a cohort of patients with orbital tumours, only three cases of solitary neurofibroma were determined, occurring in persons of middle age as a slowly growing mass of the upper quadrant [17]. Alkatan HM (2007) reported a case of isolated neurofibroma of the orbit in a 25-year-old man [1]. Shields et al. (1990) described a case in which a patient had no manifestations of neurofibromatosis with three separate orbital lesions of the right eye [19].
Chawla et al. (2013) present a case report in which they describe isolated intraocular neurofibroma, in which it was difficult to determine the origin of the primary neurofibroma, namely from which structure or the optic nerve it originated, and whether or not phthisis of the eyeball preceded the development of neurofibroma and was therefore independent of it [5].
In our patient we recorded a lesion only intrabulbarly, in the surrounding area of the disc of the optic nerve.
CONCLUSION
Enucleation of the eyeball due to benign tumour is rare. It is necessary to subject every enucleated eyeball to a thorough histopathological examination. In rare cases, isolated intraocular neurofibroma may occur as an isolated orbital or intrabulbar mass, without systemic features.
Sources
1. Alkatan, HM.: Solitary neurofibroma in the absence of neurofibromatosis. Can J Ophthalmol, 42 (4);2007 : 628–9.
2. Alshomar, KM., Alkatan, HM., Alsuhaibani, AH.: Bilateral orbital isolated (solitary) neurofibroma in the absence of neurofibromatosis - A case report. Saudi J Ophthalmol, 32 (1);2018 : 83–5.
3. Baráková, D., Krásný, J., Kuchynka, P. et al.: Nádory oka. Praha, Grada Publishing. 2002,152 p.
4. Castellanos, E., Plana, A., Carrato, C. et al.: Early Genetic Diagnosis of Neurofibromatosis Type 2 From Skin Plaque Plexiform Schwannomas in Childhood. JAMA Dermatol, 154 (3);2018 : 341–6.
5. Chawla, U., Khurana, AK., Anand, N. et al.: A rare case of a solitary intraocular neurofibroma. Nepal J Ophthalmol, 5 (2);2013 : 262–4.
6. Čmelo, J.: 3D – trojrozmerná ultrazvuková diagnostika oka a očnice [3D ultrasonography diagnostics of the eye and orbit]. Cesk Slov Oftalmol, 64 (5);2008 : 188–192.
7. Damato, B.: Recent Developments in Ocular Oncology. In Grzybowski, A. (Ed), Current Concepts in Ophthalmology. Springer International Publishing, 2020,p. 275–93.
8. DiMario, FJ., Ramsby, G.: Magnetic resonance imaging lesion analysis in neurofibromatosis type 1. Arch Neurol, 55 (4);1998 : 500–5.
9. Ehara, Y., Koga, M., Imafuku, S. et al.: Distribution of diffuse plexiform neurofibroma on the body surface in patients with neurofibromatosis 1. J Dermatol, 47(2);2020 : 190–2.
10. Furdová, A., Oláh, Z.: Nádory oka a okolitých štruktúr. Brno, Akademické nakladatelství CERM,2010,152 p.
11. Jendi, SK., Khatib, S., Mistry, J. et al.: Ossifying Fibroma of Maxilla in a Female Affected by Neurofibromatosis Type 1. Indian J Otolaryngol Head Neck Surg, 71 (Suppl 3);2019 : 2087–90.
12. Matejcik, V.: Our experience with surgical treatment of the schwannomas of peripheral nerves. Bratisl Lek Listy, 103 (12);2002 : 477–9.
13. Matejcík, V.: Tumory periférnych nervov končatín a brachiálneho plexu a ich chirurgické riešenie [Tumors of peripheral nerves of extremities and the brachial plexus and their surgical treatment]. Rozhl Chir, 81 (10);2002 : 538–543.
14. Matejcík, V., Benetín, J., Danis, D.: Our experience with surgical treatment of the tumours of peripheral nerves in extremities and brachial plexus. Acta Chir Plast, 45 (2);2003 : 40–5.
15. Muir, D., Neubauer, D., Lim, IT. et al.: Tumorigenic properties of neurofibromin-deficient neurofibroma Schwann cells. Am J Pathol, 158 (2);2001 : 501–13.
16. Ramdurg, P., Puranik, SR., Dantu, R. et al.: Solitary Neurofibroma of the Soft Palate: A Rare Entity. Indian J Otolaryngol Head Neck Surg, 71 (Suppl 1);2019 : 38–41.
17. Rootman, J.: Neoplasia. In: Diseases of the Orbit: A Multidisciplinary Approach. Philadelphia, Lippincott Williams & Wilkins, 2003, p. 213–61.
18. Rose, GE., Wright, JE.: Isolated peripheral nerve sheath tumours of the orbit. Eye Lond Engl, 5 (Pt 6);1991 : 668–73.
19. Shields, JA., Shields, CL., Lieb, WE. et al.: Multiple orbital neurofibromas unassociated with von Recklinghausen’s disease. Arch Ophthalmol, 108 (1);1990 : 80–3.
20. Sleiman, Z., Abboud, L., Mehanna, E. et al.: Mandibular neurofibroma: Case report of a rare tumor. Clin Pract, 9 (4);2019 : 1143.
21. Stough, JT.: Intra-ocular neurofibroma: report of a case. Arch Ophthalmol, 18 (4);1937 : 540–6.
Labels
Ophthalmology
Article was published inCzech and Slovak Ophthalmology

2020 Issue 2-
All articles in this issue
- Zemřela prof. MUDr. Jarmila Boguszaková DrSc.
- Vzpomínka na doc. MUDr. Cigánka, CSc.
- EPIGENETIC CHANGES IN MALIGNANT UVEAL MELANOMA AND POSSIBILITIES OF THEIR THERAPEUTIC TARGETING
- Primary Intrabulbar Neurofibroma
- Does adjuvant intracameral triamcinolone acetonide increase the effectiveness of phacotrabeculectomy? A Case-Control Study
- Non-arteritic anterior ischaemic optic neuropathy: treatment and risk factors
- Aflibercept for Vascularised Serous Pigment Epithelial Detachment: One-Year Anatomical and Functional Results
- Betaxolol, Brimonidin and Carteolol in the Therapy of Normal-Tension Glaucoma
- Czech and Slovak Ophthalmology
- Journal archive
- Current issue
- Online only
- About the journal
Most read in this issue- Non-arteritic anterior ischaemic optic neuropathy: treatment and risk factors
- Vzpomínka na doc. MUDr. Cigánka, CSc.
- Betaxolol, Brimonidin and Carteolol in the Therapy of Normal-Tension Glaucoma
- Aflibercept for Vascularised Serous Pigment Epithelial Detachment: One-Year Anatomical and Functional Results
Login#ADS_BOTTOM_SCRIPTS#Forgotten passwordEnter the email address that you registered with. We will send you instructions on how to set a new password.
- Career